Endoscopic Retrograde Cholangiopancreatography (ERCP)
- Introduction to Endoscopic Retrograde Cholangiopancreatography (ERCP)
- Clinical uses
- Preparation
- The procedure
- Complications
Introduction to Endoscopic Retrograde Cholangiopancreatography
Endoscopic Retrograde Cholangiopancreatography (ERCP) is a common investigative procedure that uses a side-viewing duodenoscope (long, slender and flexible tube) to view from the mouth to the duodenum (the initial curved section of the small intestine). Here instruments are passed down the tube to the ampulla of Vater (where the common bile duct empties into the duodenum). Contrast material is injected into the biliary tree and pancreatic ducts so they can be viewed by the physician and x-rays taken. ERCP is used primarily in the diagnosis and management of bile duct stones, and other conditions such as strictures (narrowing due to scars), leaks and malignancies (cancers).
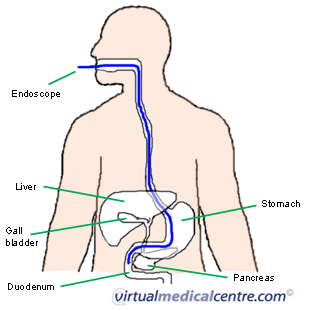
Clinical uses
ERCP is a common procedure performed in investigation of pancreatic and biliary disease. The pancreas is a glandular organ that produces both digestive juices and hormones. It secretes enzymes for digestion into a series of ducts that eventually enter the duodenum. Bile, on the other hand, is produced by cells of the liver, and is stored in the pear shaped organ called the gall bladder. Bile helps digest fats and is excreted via the bile ducts to the duodenum.
Diagnostically, ERCP may be used in patients with expected bile duct stones, recurrent pancreatitis and obstructive jaundice. In recurrent acute pancreatitis, ERCP can be used to look for possible causes such as small biliary stones (not detected by other imaging), abnormal duct structure or obstruction. Chronic pancreatitis can also be diagnosed by some mild changes in the pancreatic ducts.
ERCP is often performed preoperatively in patients with gallstones undergoing surgery to remove the gallbladder. If common bile duct stones are suspected, removal by ERCP before surgery produces a more favourable outcomes. ERCP may also be performed after the cholecystectomy (removal of the gall bladder).
Therapeutic indications have already been mentioned and include sphincterectomy (cutting open the muscle ring) to remove common bile duct stones and stenting of malignant or inflammatory strictures. Stents may be used in carcinoma (cancer) of the pancreas, bile duct or duodenum. Furthermore, biopsies for suspected malignancies can be taken. Finally, stents and sphincterectomy may be used in the management of bile leaks which are a possible complication of surgery, trauma, or other procedures.
Preparation
Generally, ERCP will require you to be in a fasted state to ensure the best results are obtained at minimal risk. You will not be able to eat or drink from midnight on the night before the procedure. It is also important to let the physician know of any allergies you have to medications or iodine, which is present in the contrast material.
The procedure
In ERCP, the side-viewing duodenoscope (long, slender, flexible tube) is passed all the way from the mouth to the duodenum. The camera allows the physician to identify the ampulla of Vater, which is where the bile ducts and pancreatic ducts empty their contents into the duodenum. In the centre of the duodenoscope there is a specialised equipment channel. Thin tubes called catheters and cannulas are passed through the duodenoscope and into the biliary tree at the ampulla of Vater.
Radiographic contrast material is injected so both the biliary tree and pancreas can be visualised and X-rayed. From these images small pale stones can be seen, along with any narrowing or other abnormalities of the ducts. Stones are small pebbles made of cholesterol or pigment that can get caught in the bile ducts and cause obstruction.
During the procedure, you will be laying down on an examination table. You will be awake but quite sedated due to the different medications. You take a number of medications to help you sleep, avoid pain, stop vomiting and prevent infection during the procedure and usually these will be administered a few hours before the procedure. The duodenoscope is passed down the back of your throat while you try to swallow it. The physician then examines the bile ducts using contrast and detects whether there are any stones.
If large stones (greater than 1cm) are present in the common bile duct, a procedure known as an endoscopic sphincterectomy can be performed. For this a small cut is made in the ring of muscle surrounding the ampulla of Vater to make a larger opening for the stones to pass out off. Fluid is then flushed through the tube and special equipment is used to suck and pull any stones out of the ducts.
If stones are too large to be removed this way they must be broken down using other processes. Small bile duct stones can be removed by inserting a balloon into the ducts without having to cut the muscle ring. Sometimes stents (small rigid plastic tubes) are inserted into the bile ducts to open up narrowings caused by inflammation or cancer. In addition, small samples of tissue (biopsies) may be taken for further testing.
Often ERCPs are done in the hospital whilst patients are admitted with gallstones or pancreatic disease. The whole procedure usually takes between 30 minutes and two hours. Generally, patients do not report feeling much pain or discomfort as the medications are designed to prevent this. It may take some time for the sedatives to wear off.
Complications
Complications occur in 2-3% of cases of ERCP and may be associated with significant morbidity and mortality. The following complications have been reported.
- Bleeding
- Pancreatitis occurs in 5-10% of patients undergoing ERCP and is the most common complication. Studies are been done to determine drugs that can help prevent this occurring.
- Perforation (tearing or rupture) can occur due to damage by instruments at the time of investigation.
- Cholangitis (infection of the bile ducts) can occur. Antibiotics are given to all patients with suspected bile duct obstruction to prevent infection.
References
- Bateson. ‘Gall bladder disease.’ British Medical Journal. 1999, vol. 318, pp. 1745-1748.
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 15th Edition. McGraw-Hill. 2001
- Brugge, Van Dam. ‘Pancreatic and biliary endoscopy.’ The New England Journal of Medicine. 1999, vol. 341, no. 24, pp 1808-1816.
- Burkitt, Quick. Essential Surgery. 3rd Edition.Churchill Livingstone. 2002.
- Corvera, Kirkwood. ‘Recent advances: General surgery.’ British Medical Journal. Vol. 315, pp. 586-589
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
Dates
Tags
Created by:

 Login
Login