Jaundice is defined as yellow discolouration due to increased serum bilirubin level. This is usually found in the skin, sclerae (the white part of eye) and mucus membranes. The image displayed shows marked discolouration of the patient’s sclera, called scleral icterus. This sign may be present before discolouration of the skin is noticed and is used to clarify the prescence of jaundice. 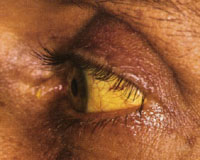
- There is too much bilirubin produced due to too many red blood cells being destroyed.
- The liver fails to process the bilirubin to be excreted.
- Something blocks the passage of bile into the gut.
Jaundice itself does not cause many problem except for cosmetic reason. However the diseases that cause jaundice need to be assessed and treated. These diseases usually have other significant symptoms such as tiredness, ankle swelling, confusion, coma, gastrointestinal bleeding, ascites, etc. There are many causes of jaundice. However most can be identified fairly quickly using clinical investigations.
Causes
The causes of jaundice can be divided as follows:
- Increased bilirubin production due to increased red blood cells being destroyed (this is known as haemolysis): collection of blood in the tissue, increased red blood cells destruction leading to tiredness, lethargy, etc (also known as haemolytic anaemia).
- Failure of the liver to process the bilirubin to be excreted: many diseases that affect the liver such as viral infection, genetic diseases, excessive accumulation of chemicals (copper and iron), or tumour can cause jaundice by this means. A disease known as Gilbert’s syndrome is a common but harmless genetic disease that causes jaundice through this method.
- Blockage of the passage of bile into the gut: this include gallstones and cancer of the bile duct or liver.
Other causes include pregnancy and neonatal jaundice where this happens in newborn babies.
Assessment
The complete assessment of jaundice will include clinical history, clinical examination, general and specific investigations. In clinical history, a complete routine medical history needs to be obtained. From history alone most of the causes of jaundice can be suspected. Features that will be asked include pale stool, dark urine, generalised itchiness, gallbladder pain, tummy pain, and others. In clinical examination, a thorough general examination will be carried out. Specifically, the liver and spleen should be felt for any enlargement. Other features to look for include signs of anaemia (lack of red blood cells in the body). As for general investigations, routine blood tests to check for the liver and blood system will be done. The urine will be tested as well. In order to find the exact cause, most likely some specific investigations will be done. This include ultrasound for the liver and tummy, CT of the tummy, or even direct visualisation of the bile ducts in the tummy. Ocassionally, a sample of the liver tissue may be required to make the diagnosis (this is called liver biopsy).
Treatment
The treatment of jaundice varies according to the causes. A haematologist (specialist in the blood system), surgeon, or physician might be involved in treating the causes of jaundice.
References
- MedicineNet.com: Jaundice [online]. 2005. [Cited 2005 September 23rd]. Available from: URL: http://www.medicinenet.com/jaundice/article.htm#toca
- Surgical tutor: Obstructive Jaundice [online]. 2005. [Cited 2005 September 23rd]. Available from URL: http://www.surgical-tutor.org.uk/default-home.htm?system/abdomen/jaundice.htm~right
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







