Scars
What is a scar?
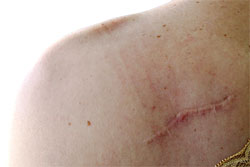 In humans, injured skin cannot regenerate, or ‘grow back’. Instead, the damaged tissue is replaced with scar tissue. A scar (also known as a cicatrix) is fibrous tissue that is visible following healing of a wound. The formation of scars is a normal part of the healing process.They occur when a skin wound extends deeper than the outer layer of skin (epidermis) into the deeper layer of skin (dermis).
In humans, injured skin cannot regenerate, or ‘grow back’. Instead, the damaged tissue is replaced with scar tissue. A scar (also known as a cicatrix) is fibrous tissue that is visible following healing of a wound. The formation of scars is a normal part of the healing process.They occur when a skin wound extends deeper than the outer layer of skin (epidermis) into the deeper layer of skin (dermis).
Collagen is the substance the body uses to heal areas of damage in the body. It forms a dense, fibrous connective tissue. Scars occur because collagen is not the same texture or colour, and does not have the same properties, as the skin that it is replacing. The epidermis regrows over the top, but the normal ridges (that form fingerprints) are not replaced.Extra structures in the skin such as sweat glands and hair follicles are also not present in scar tissue.
Scar tissue is less strong and less functional than the tissue it is replacing, and may result in functional, psychological and cosmetic problems. The collagen in scar tissue is laid down in a disorganised fashion, so scars only reach a maximum of 70% of the strength of normal skin. In some people, scarring may be excessive to that required to heal a wound, and this is known as hypertrophic or keloid scarring.
When do scars occur?
Scars can occur following any event that damages the skin tissue. Such events include:
- Injuries such as cuts and scrapes (abrasions);
- Burns (sunburn, thermal burns etc);
- Sores (lesions) such as diabetic or pressure ulcers, insect bites etc;
- Surgery;
- Infections (eg chickenpox); and
- Skin conditions (acne, psoriasis etc). Scars affect 30% of people with moderate or severe acne.
What types of scars occur?
Acne that has recently healed may result in scars with the appearances outlined below:
- Pink or purple flat small patches (post inflammatory erythema);
- Brown marks (pigmentation) seen in people who tan easily (post inflammatory pigmentation);
- White or pale marks (post inflammatory hypopigmentation); and/or
- Ice pick scars: tend to be small (less than 2mm diameter), deep and pitted. They commonly occur on the cheeks.
- Depressed or boxcar scars are around 1.5-4mm in diameter and may be shallow (<0.5mm) or deep (>0.5mm). Their walls are steep, and they are sharply defined.
- Soft rolling scars are often greater than 4mm in diameter, and can be circular or linear, with gently sloped edges that merge with normal skin.
- Atrophic scars, flat, thin scars with a slightly wrinkled texture.May be somewhat pigmented. Atrophic scars may develop following skin damage other than that which occurs in acne.
- Hypertrophic and Keloid scars (discussed below).
Hypertrophic scars are raised scars, confined to the anatomical boundaries of the original injury.Hypertrophic scarring is more common in fair skin, and in children.
They tend to occur when there is tension (pull) on a wound, or when there are deep wounds, such as following surgery or burns.
They develop around four weeks following injury.Hypertrophic scars may become smaller over time.
Keloid scars grow beyond the boundaries of the original wounds.Keloid scarring occurs more commonly in darker skin and may develop following trivial injuries including insect bites, vaccination, or piercing.
Rates of keloid occurrence have been reported as high as 16% in predominantly Black populations. They are uncommon in children and the elderly.
They tend to develop more than three months after the original injury, do not generally get smaller, and usually recur after they are cut out. Keloids commonly occur on the cheeks, earlobes, chest, upper arms and the shoulders.They may be associated with pain and itching. The cause of keloid scars remains unclear.
Stretch marks are faded, linear marks, perpendicular to the line of greatest skin tension. They occur following damage to the deep layer of the skin (dermis) due to stretching or hormonal changes.
Stretch marks are initially red, they become violet, before assuming their final appearance as white lines.
Stretch marks commonly occur on the breasts, hips, buttocks, thighs and abdomen.They develop following physical stretching of the skin, such as in obesity, weightlifters, from growth spurts, or during hormonal changes, such as in pregnancy (striae gravidarum) and Cushing’s disease.
What factors affect scarring?
 Size and depth of wound
Size and depth of wound
Larger, deeper wounds tend to result in more prominent scarring.
Part of the body affected
Factors such as blood supply, sun exposure, skin thickness, and mechanical stress vary between body parts. These factors impact on scar formation. Areas with poor blood supply, thin skin, increased stress (such as front of the knee), and increased sun exposure may be more likely to scar. Scars are more obvious in areas where skin is pulled tightly (such as the jawbone) than where it is soft (such as the cheek).
Age
Younger skin tends to form larger thicker scars, because the healing response produces stronger repairs.
Inherited tendency to scar
Tendency to develop keloid scarring may be inherited.
Skin colour
Hypertrophic scarring is more common in fair skin, while keloid scarring is more common in darker skin.
Length of time it takes the skin to heal
Wounds that take a long time to heal may be more likely to scar.
Physical features of the scar
The physical characteristics of a scar affect its visibility and therefore its cosmetic ‘severity’. If a scar is indented or raised, irregular shadows form which increase the visual impact of the scar. Scars that cross natural expression lines are more apparent, because they do not look like naturally occurring lines such as wrinkles.
How do scars change over time?
True scarring, where significant amounts of fibrous tissue are laid down to heal a wound, will never completely go away. This is because the fibrous tissue remains in the skin, and will never have the same appearance as undamaged skin tissue.
Appearance of scars usually improves over time. Scars tend to appear red and thick at first, and fade slowly over months.Changes include a decrease in the ‘tightness’ of scars (contractures), flattening, softening, and change of colour (repigmentation).
In some cases, such as skin colour changes following acne, it may take many months for the scar to become invisible. Improvement in the appearance of scars, even without treatment, may continue to occur for 6-18 months.
Keloid scars tend to recur, despite treatment that initially appears successful.
References
- American Academy of Dermatology. What is a scar [online] 2004 [cited 2009 Mar 28] Available from: http://www.aad.org/ public/ publications/ pamphlets/ cosmetic_scar.html
- Hantash BM. Zhao L. Knowles JA. Lorenz HP. Adult and fetal wound healing. Frontiers in Bioscience. 2008;13:51-61.
- Bolognia J, Jorizzo J, Rapini R, editors. Dermatology. 2nd ed. USA: Mosby; 2007.
- Reish R, Eriksson E. Scars: A Review of Emerging and Currently Available Therapies. Plastic and Reconstructive surgery. 2008;122(4):1068-78.
- Rhett J, Ghatnekar G, Palatinus J, O’Quinn M, Yost J and Gourdie R. Novel therapies for scar reduction and regenerative healing of skin wounds. Trends in Biotechnology 2007; 26 (4):123-80.
- Broughton G, Janis J. Wound Healing: An Overview. Plastic and reconstructive surgery. 2006;117 (1e-S): 1-32e-S.
- Miller M, Nanchahal J. Advances in the Modulation of Cutaneous Wound Healing and Scarring. Biodrugs 2005; 19 (6): 363-81.
- New Zealand Dermatological Society Incorporated. Acne Scarring [online] 2008 [cited 2009 Mar 28]. Available from: http://www.dermnetnz.org/ acne/ acne-scarring.html
- Rivera A. Acne scarring: A review and current treatment modalities. Journal of the American Academy of Dermatology. 2008; 59 (4):659-76.
- Jacob CI, Dover JS, Kaminer MS. Acne scarring: a classification system and review of treatment options. J Am Acad Dermatol 2001;45:109-17.
- O’Brien L, Pandit A. Silicon gel sheeting for preventing and treating hypertrophic and keloid scars. Cochrane Database of Systematic Reviews 2006, Issue 1. Art. No.: CD003826. DOI: 10.1002/14651858.CD003826.pub2.
- Yosipovitch G. DeVore A. Dawn A. Obesity and the skin: skin physiology and skin manifestations of obesity. Journal of the American Academy of Dermatology. 2007;56(6):901-16.
- Salter SA. Kimball AB. Striae gravidarum. Clinics in Dermatology. 2006;24(2):97-100.
- Singh G. Kumar LP. Striae distensae. Indian Journal of Dermatology, Venereology & Leprology. 2005;71(5):370-2.
- Reish R and Eriksson E. Scar Treatments: Preclinical and Clinical Studies J Am Coll Surg. 2008; 206 (4)719- 730.
Dates
Tags
Created by:

 Login
Login














