Fine Needle Aspiration Biopsy (FNA)
- Fine Needle Aspiration Biopsy (FNA): An introduction
- Performing a Fine Needle Aspiration Biopsy (FNA)
- Results of a Fine Needle Aspiration Biopsy (FNA)
- Effectiveiness of a Fine Needle Aspiration Biopsy
- Benefits and Risks of a Fine Needle Aspiration Biopsy
- Fine Needle Aspiration Biopsy or Core Biopsy?
Fine Needle Aspiration Biopsy (FNA): An introduction
A Fine Needle Aspiration (FNA) Biopsy is a simple procedure that involves passing a thin needle through the skin to sample fluid or tissue from a cyst or solid mass, as can be seen in the picture below. The sample of cellular material taken during an FNA is then sent to a pathology laboratory for analysis. Fine needle aspiration biopsies are often performed when a suspicious lump is found, for example a breast lump or enlarged lymph node, or if an abnormality is detected on an imaging test such as x-ray, ultrasound or mammography. Fine needle aspiration is a relatively non-invasive, less painful and quicker method when compared to other methods of tissue sampling such as surgical biopsy. A cyst aspiration can also be achieved with a FNA, where the fluid is drained from a cyst with no need for analysis. 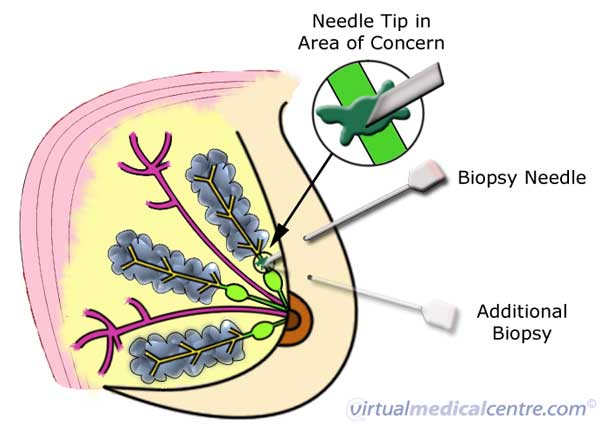
Information on re-publishing of our images
Performing a Fine Needle Aspiration Biopsy (FNA)
A fine needle aspiration biopsy is a simple and quick procedure. It is performed to collect a sample of cells or fluid from a cyst or solid mass, to allow the cells to be examined under a microscope. Local anaesthetic is not usually required for a fine needle aspiration, as the procedure should not be painful. Fine needle aspirations may be performed on palpable lumps (lumps which can be felt), or impalpable lumps which have been detected on ultrasound or x-ray. Once the skin has been cleaned at the needle entry point, the lump is then examined. If the lump can be felt, your doctor or surgeon will palpate the lump to position it for the needle. If the lump cannot be felt, imaging may be required to find the exact location. This can be done with ultrasound, where the surgeon will watch the needle on the ultrasound monitor and guide it to the area, or with a stereotactic mammogram (for the breast) which uses two mammograms at different angles and a computer to create exact coordinates.  The type of needle used for fine needle aspiration biopsy has a hollow interior and is much finer than a regular needle used to draw blood. You can see an example of what the needle may look like in the image to the right. The insertion of the needle is said to be similar to the sensation of a blood test. A vacuum or negative pressure is created in the needle and with an in and out motion of the needle, the sample is taken. Several needle insertions may be required to ensure that the sample is adequate. Once the test is completed, a small bandage will be placed over the site and you can continue your normal activities. There are generally no complications with this procedure, though you may experience some tenderness or bruising over the needle insertion site. If you experience any bleeding, swelling, fever or pain that is not relieved with paracetamol, contact your doctor immediately. It is not recommended that you use aspirin to relive pain as it may worsen any bruising.
The type of needle used for fine needle aspiration biopsy has a hollow interior and is much finer than a regular needle used to draw blood. You can see an example of what the needle may look like in the image to the right. The insertion of the needle is said to be similar to the sensation of a blood test. A vacuum or negative pressure is created in the needle and with an in and out motion of the needle, the sample is taken. Several needle insertions may be required to ensure that the sample is adequate. Once the test is completed, a small bandage will be placed over the site and you can continue your normal activities. There are generally no complications with this procedure, though you may experience some tenderness or bruising over the needle insertion site. If you experience any bleeding, swelling, fever or pain that is not relieved with paracetamol, contact your doctor immediately. It is not recommended that you use aspirin to relive pain as it may worsen any bruising.
Results of a Fine Needle Aspiration Biopsy (FNA)
The samples taken are examined by a pathologist under a microscope. A detailed report will then be provided about the type of cells that were seen, including any suggestion that the cells might be cancer. It is important to remember that having a lump or mass does not necessarily mean that it is cancerous; many fine needle aspiration biopsies reveal that suspicious lumps or masses are benign (non-cancerous) or cysts. Aspirate samples may be described as one of the following types:
- Inadequate/insufficient: The sample taken was not adequate to exclude or confirm a diagnosis.
- Benign: There are no cancerous cells present. The lump or growth is under control and has no spread to other areas of the body.
- Atypical/indeterminate, or suspicious of malignancy: The results are unclear. Some cells appear abnormal but are not definitely cancerous. A surgical biopsy may be required to adequately sample the cells.
- Malignant: The cells are cancerous, uncontrolled and have the potential or have spread to other areas of the body.
Effectiveiness of a Fine Needle Aspiration Biopsy
A fine needle biopsy is an effective tool in evaluating and diagnosing suspect lumps or masses. A quick diagnosis can mean that cancer is detected early, giving more options for treatment, or that benign lumps are diagnosed without the need for surgery. It is non-invasive and only slightly uncomfortable, compared to a surgical biopsy which requires a general anaesthetic, involves pain and the possibility of infection or scarring. Fine needle aspiration biopsies do require some expertise to perform and interpret. To ensure that an accurate result is achieved, it is important that the general practitioner, radiologist, surgeon, pathologist or oncologist who performs your procedure has experience in fine needle aspiration biopsy.
Benefits and Risks of a Fine Needle Aspiration Biopsy
A fine needle biopsy is a quick and effective test for determining the status of suspect tissue. Compared to a surgical biopsy, fine needle aspiration biopsy involves little possibility of scarring, infection or pain, and has a significantly shorter recovery time. It is also extremely useful in the diagnosis and treatment of cysts. The risks of fine needle aspiration biopsy include the possibility of cancer cells being trailed into unaffected tissue as the needle is removed, but this is rare when the test is performed by skilled practitioners. Because an FNA biopsy can only sample a small number of cells from a mass or lump, there is a risk that any abnormal cells may be missed and not detected. This may mean that a larger sample must be taken, for example by core needle biopsy.
Fine Needle Aspiration Biopsy or Core Biopsy?
Core Biopsy is another method of ’tissue diagnosis’ – that is, a way of sampling the cells in a suspicious lump or mass. It is sometimes used instead of fine needle aspiration biopsy, or vice versa. Core biopsy is a more invasive procedure than FNA, as it involves making a small incision (cut) in the skin. A large needle is then passed through this incision and several narrow samples of the tissue to be investigated (such as a lump) are taken. As with fine needle aspiration, ultrasound or mammographic guidance may be needed to locate the lump or area to be sampled. 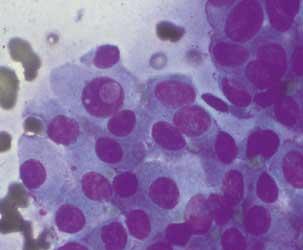 Core biopsy is done under local anaesthetic. The procedure usually takes between 30 minutes and 1 hour. After the procedure, the biopsy area will be covered with a simple dressing. A core biopsy may result in a small, very fine scar where the incision was made. The samples of tissue taken during a core biopsy differ from those taken during FNA. Because the cells from a fine needle aspiration biopsy are sucked up randomly into the needle, they are seen under the microscope as a disorganised jumble of cells (see the image at right). With a core biopsy sample, however, the larger needle allows the cells to be removed with their relationship to each other intact. This can sometimes help in diagnosis.
Core biopsy is done under local anaesthetic. The procedure usually takes between 30 minutes and 1 hour. After the procedure, the biopsy area will be covered with a simple dressing. A core biopsy may result in a small, very fine scar where the incision was made. The samples of tissue taken during a core biopsy differ from those taken during FNA. Because the cells from a fine needle aspiration biopsy are sucked up randomly into the needle, they are seen under the microscope as a disorganised jumble of cells (see the image at right). With a core biopsy sample, however, the larger needle allows the cells to be removed with their relationship to each other intact. This can sometimes help in diagnosis.
References
- Britton PD. Fine needle aspiration or core biopsy. The Breast 1999;8:1-4.
- National Breast Cancer Centre. Breast fine needle aspiration cytology and core biopsy: a guide for practice [online]. 2004 [cited 2007 February 16th]. Available from: http://www.nbcc.org.au/bestpractice/resources/FNA_fineneedleaspir.pdf
- National Breast Cancer Centre. 2001. Clinical practice guidelines for the management of early breast cancer: Second edition. National Breast Cancer Centre, Camperdown, NSW. [online] Available from: http://www.nhmrc.gov.au/publications/synopses/cp74syn.htm
- National Breast Cancer Centre. The investigation of a new breast symptom: a guide for General Practitioners [online]. 2006 [cited 2007 February 16]. Available from: http://www.nbcc.org.au/bestpractice/resources/IBS172_theinvestigationofan.pdf
- Murtagh J. General Practice 3rd ed. Sydney, McGraw-Hill, 2003.
Dates
Tags
Created by:

 Login
Login














