Dairy, calcium and hypertension
Two newly published research studies have helped clarify important aspects of the relationship between dairy foods, calcium and blood pressure.
A considerable body of evidence points to a small protective relationship between dairy foods or calcium, and raised blood pressure. It has not been easy to tell whether the ‘active ingredient’ in this relationship is simply the calcium in dairy, some other bioactive component, or the whole food. A fresh analysis from the large Women’s Health Study has attempted to separate the effect of these two dietary factors, as well as vitamin D.1 Observations were made on 28,886 US female health professionals (≥ 45 years of age) over a period of 10 years after initially having had their dietary history recorded. 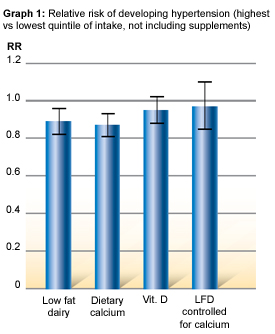
After adjusting for other known risk factors for elevated blood pressure, there was a greater than 10% reduction in the risk of developing hypertension over 10 years associated with being in the highest rather than the lowest quintile of initial dietary intake of low fat dairy and dietary calcium but not vitamin D (in the US, milk is fortified with vitamin D).
See Graph 1.
Importantly, however, no significant relationship with hypertension was seen in relation to intake of calcium or vitamin D as supplements. There was also no significant association between high blood pressure and regular fat dairy intake. Finally, when dairy consumption was controlled for calcium intake, the association of low fat dairy food with hypertension is not present. This is however not surprising, since dairy foods account for 80% of dietary calcium intake in this population.
The authors concluded that these results support the findings of several human clinical trials in which a more consistent blood pressure lowering effect has been obtained when whole foods were used, compared with when supplemental calcium was given. They believe this suggests "the importance of a complete nutritional profile for the BP effects".
This notion of the importance of whole diet was strengthened by results from a new clinical trial that was conducted in an important, but often neglected, patient population – adolescents with high blood pressure.2 The trial compared blood pressure outcomes in 57 US adolescents with borderline or actual hypertension. The subjects were randomised to receive advice to follow either a routine outpatient dietary recommendation (consistent with national guidelines for hypertension) or a DASH diet, which emphasises 3 daily servings of low fat dairy foods, along with 8 servings of fruits and vegetables. This was maintained for 3 months, with a further follow-up 3 months post-intervention. In the 46 subjects who completed the intervention, there was a significantly greater fall in systolic blood pressure after treatment completion in DASH vs routine diet (10.4 vs 1.9 mm Hg, p<0.01). The difference between treatment groups persisted to the follow-up visit, but fell below statistical significance. Although, when all the subjects’ data was incorporated (including those who did not complete the trial), the difference was significant (6.8 vs 2.8 mm Hg, p<0.05). It was interesting that the blood pressure falls were not related to any differences in weight loss between the two groups.
References:
- Wang L, et al. Dietary intake of dairy products, calcium, and vitamin D and the risk of hypertension in middle-aged and older women. Hypertension. 2008; 51(4): 1073-9.
- Couch SC, et al. The efficacy of a clinic-based behavioral nutrition intervention emphasizing a DASH-type diet for adolescents with elevated blood pressure. J Pediatr. 2008; 152(4): 494-501.
Dates
Tags
Created by:

 Login
Login














