Diabetes
- Diabetes mellitus
- Blood glucose and dietary controls
- Diabetic eye disease
- Diabetes insipidus
- Supportive care
Diabetes mellitus
Diabetes mellitus type 1 (insulin dependent, juvenile onset)
 | Type 1 diabetes mellitus is a chronic metabolic syndrome defined by an inability to produce insulin, a hormone which lowers blood sugar. It is predominantly a disease of the young, usually developing before 20 years of age. |
For more information, see Diabetes Mellitus Type 1 (Insulin Dependent, Juvenile Onset).
Diabetes mellitus type 2 (non-insulin dependent, mature age onset)
 | Type 2 diabetes mellitus is defined by resistance to the hormone, insulin. This leads to inappropriate hyperglycaemia (increased blood sugar levels) and deranged metabolism of carbohydrate, fats and proteins. Rates are increasing presumably due to the aging population and increased rates of obesity. |
For more information, see Diabetes Mellitus Type 2 (Non-Insulin Dependent, Mature Age Onset).
Gestational diabetes mellitus
 | GDM is a temporary condition that usually disappears after pregnancy. However, for some women the condition becomes chronic. It is important that GDM is diagnosed and treated, because without treatment it may lead to significant health problems for a mother and her baby. |
For more information, see Gestational Diabetes Mellitus.
Blood glucose and dietary control
Blood glucose control
 | Our blood glucose level, or blood sugar level, is the amount of glucose (sugar) in the blood. Glucose levels are measured most commonly to diagnose or to monitor diabetes. Raised glucose levels can cause long term complications. |
For more information, see Blood Glucose Control.
Glycaemic index (GI)
 | Glycaemic index (GI) measures the effect that a carbohydrate containing food has on blood glucose levels compared to the effect of the same amount of pure glucose, on blood glucose levels. Studies have shown that if a patient with diabetes adheres to a diet rich in healthy and low GI foods, the long term complication rate is reduced |
For more information, see Glycaemic Index (GI).
Glycaemic load (GL)
 | Different foods may contain similar amounts of carbohydrate, but have different glycaemic effects. The GL is defined as a system for ranking the carbohydrate content in food products based on the GI and serving size. It is determined by multiplying the GI value of the food by the carbohydrate content of the food. |
For more information, see Glycaemic Load (GL).
Diabetic eye disease
Diabetes and eye diseases
 | Diabetes is common, chronic condition that affects the body’s ability to control sugar levels. This can be due to autoimmune damage to the pancreas (Type 1 diabetes), or due to decreased effects of insulin due to poor diet, such as in the much more common Type 2 diabetes. Both these types of diabetes are associated with a wide range of complications, such as kidney disease or diabetic eye diseases. |
For more information, see Diabetes and Eye Diseases.
Non-proliferative diabetic retinopathy
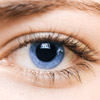 | Non-proliferative diabetic retinopathy, previously called background retinopathy, is the earliest stage of diabetic eye disease. It is characterised by changes to the blood vessels in the eye’s retina which restrict blood flow to the eye. Non-proliferative diabetic retinopathy does not affect vision but can progress to proliferative retinopathy or cause macular oedema. These are both sight-threatening conditions. |
For more information, see Non-Proliferative Diabetic Retinopathy.
Proliferative diabetic retinopathy
 | Proliferative diabetic retinopathy is a sight-threatening eye disease that affects diabetics and sometimes people with metabolic abnormalities such as metabolic syndrome. It is characterised by neovascularisation in the eye, and fibrous growth in the retina and surrounding vitreous fluid. Early treatment can help prevent future vision loss, but not restore sight that has already been lost. |
For more information, see Proliferative Diabetic Retinopathy.
Diabetic macular oedema
 | Diabetic macular oedema is a sight-threatening eye condition. It is characterised by the leaking of blood from damaged vessels of the retina (light sensing layer of the eye) into the macula (the section of the eye which enables clear, sharp vision). Diabetic macular oedema affects diabetics with proliferative or non-proliferative diabetic retinopathy. |
For more information, see Diabetic Macular Oedema.
Diabetes insipidus
Diabetes insipidus
 | Diabetes insipidus causes impaired vasopressin (hormone that regulates the kidneys) secretion or renal resistance to its action. Symptoms include excessive and persistant discharge of urine, that leads to dehydration and extreme thirst. |
For more information, see Diabetes Insipidus.
Diabetes insipidus – central
 | DI caused by a lack of the anti diuretic hormone (ADH) is called central diabetes insipidus. ADH is a hormone produced in a region of the brain called the hypothalamus. Central diabetes insipidus is caused by damage to the hypothalamus or pituitary gland as a result of surgery, infection, tumour, or head injury. |
For more information, see Diabetes Insipidus – Central.
Diabetes insipidus – nephrogenic
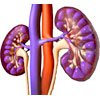 | When DI is caused by failure of the kidneys to respond to ADH, the condition is called nephrogenic diabetes insipidus. Most commonly, it is an acquired disorder. Precipitating factors include drugs, electrolyte disorders and urinary obstruction. |
For more information, see Diabetes Insipidus – Nephrogenic.
Supportive care
Diabetes Australia NSW
 | Diabetes Australia NSW is the third oldest diabetes organisation in the world and one of the largest member based groups in Australia with more than 53,000 members. It has existed since 1937 and is a non-profit charity, with funds going towards research, education, public awareness and advocacy. |
For more information, see Diabetes Australia NSW.
Dates
Tags
Created by:

 Login
Login














