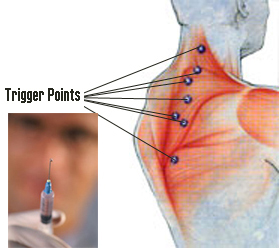
- An introduction to trigger point injection of local anaesthetic
- What are trigger points?
- Clinical presentation of trigger points
- Management of trigger point pain
- Trigger point injection of local anaesthetic
- Are there any risks of trigger point injections?
- What should be expected after a trigger point injection?
An introduction to trigger point injection of local anaesthetic
Myofascial pain syndrome is associated with trigger points, which are discrete spots that are painful on compression and produce referred pain and tenderness as well as muscle dysfunction. One effective treatment for trigger point pain is trigger point injection of local anaesthetic.
What are trigger points?
Trigger points, as illustrated above, are discrete, focal, hyperirritable spots that are painful on compression and can produce referred pain or tenderness as well as problems with muscle function. Trigger points are seen in myofascial pain syndrome, a common painful muscle disorder.
Clinical presentation of trigger points
Patients often report regional persistent pain resulting in decreased range of movement of the muscle in question, which are often muscles involved in maintaining posture. In the head and neck region, trigger point pain may manifest as tension headache, tinnitus, temporomandibular joint pain, eye symptoms or torticollis. In the arm, the pain may mimic bursitis or tendonitis, and in the legs the pain can be a cause of limited range of movement of the knee or ankle.
Management of trigger point pain
Approaches to treatment of trigger point pain include:
Non-pharmacological:
- Trigger point injections of local anaesthetic.
- Other supportive measures, including acupuncture, massage, heat (see article on Analgesia).
The long-term effectiveness of various therapies has not been proven in clinical studies.
Pharmacological:
- Simple analgesia including paracetamol and NSAIDs
- Muscle relaxants
- Antidepressant medication as coanalgesia
Trigger point injection of local anaesthetic
Trigger point injection can effectively inactivate trigger points and provide prompt symptomatic relief.
Who should have a trigger point injection?
Patients with myofascial pain syndrome who have symptomatic trigger points.
Who should not have a trigger point injection?
If you have:
- Anticoagulation or bleeding disorders
- Aspirin ingestion within three days of injection
- The presence of local or systemic infection
- Allergy to anesthetic agents
- Acute muscle trauma
- Extreme fear of needles
Are there any risks of trigger point injections?
- Vasovagal syncope (fainting)
- Skin infection
- Collapsed lung (very rare)
- Haematoma formation; avoid by applying direct pressure for at least two minutes after injection.
What should be expected after a trigger point injection?
- Post-injection soreness is to be expected in most cases. This should not be confused with failure of treatment. This soreness usually lasts 3 to 4 days.
- You should remain active following the trigger point injections but avoid strenuous activity for the first 3 to 4 days after the injection.
References
- Alvarez, D. Rockwell, P. Trigger points: diagnosis and management. Am Fam Physician. 2002; 65: 653-60.
- Han, S. Harrison, P. Myofascial pain syndrome and trigger point management. Reg Anesth. 1997; 22: 89-101.
- Imamura, S. Fischer, A. Imamura, M. et al. Pain management using myofascial approach when other treatment failed. Phys Med Rehabil Clin North Am. 1997; 8: 179-96.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.