- What is laser eye surgery?
- Laser photocoagulation
- Laser treatment for correcting refractive errors
- Which laser eye surgery?
- Conclusion
What is laser eye surgery?

The use of laser in eye diseases is known as “laser photocoagulation” or “laser photoablation”. Laser photocoagulation can be used to treat diabetic eye diseases, such as proliferative diabetic retinopathy or macular oedema. It can also be used to treat some cases of age-related macular degeneration, chronic open-angle glaucoma, retinal tears and even treat premature babies that have retinopathy of prematurity.
Laser photoablation is often used in laser eye surgery procedures such as laser-assisted in situ keratomileusis (LASIK) to correct refractive errors (inability of the eye to focus light due to a misshapen cornea). Lasers can be used to carefully reshape the cornea of the eye, to correct eye conditions like short-sightedness (myopia) or astigmatism. These procedures are increasingly common and show excellent results and can remove the need for corrective lenses, such as glasses or contact lenses.
Laser photocoagulation
Laser photocoagulation therapy is used in certain types of eye diseases due to diabetes. As diabetes advances, the tiny blood vessels in the retina are vulnerable to damage and can result in sight-threatening conditions such as diabetic retinopathy and diabetic macular oedema. These conditions can be treated by laser, which can also be used in combination with other treatments, such as injections of steroids or anti-vascular endothelial growth factor (anti-VEGF) therapies (treatments that block the activity of VEGF which is a chemical that normally promotes growth of new blood vessels) into the eye.
Diabetic retinopathy
Laser photocoagulation is used in diabetic retinopathy, as the retinal blood vessels have begun to leak due to vessel damage from diabetes. This leaking can cause damage to surrounding tissue, as well as preventing oxygen from reaching cells supplied by those blood vessels. Worse still, new, more fragile blood vessels may grow (proliferative diabetic retinopathy), which can also leak and cause damage. Laser photocoagulation can block off any abnormal blood vessels and stop the damaging leaks, as well as destroy tissue that is stimulating the growth of these new, abnormal blood vessels.
While a very effective treatment, laser photocoagulation is not without side effects. The procedure can be uncomfortable and individuals can experience transient blurring, glare sensitivity or difficulty with light-dark adaptation in the days and weeks after the procedure. Other possible side effects are rare and can also occur due to diabetic retinopathy itself. These include peripheral field constriction, night blindness, loss of eye muscle function, mild colour vision changes, retinal detachment, glaucoma or burns to the cornea, iris or lens.
 |
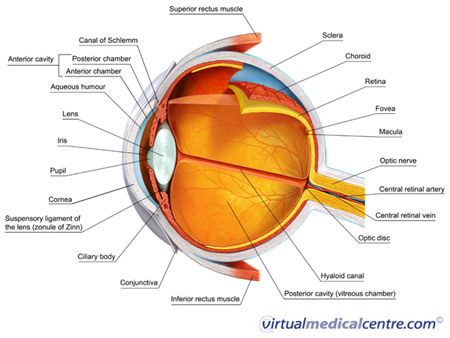
For more information about the structure and function of the eye, see The Eye and Vision. |
Diabetic macular oedema
Macular oedema is a swelling of the macula, which lies at the centre of the retina and is responsible for our most detailed vision. It can occur in some patients with diabetes. Laser therapy can stabilise macular oedema and prevent further fluid accumulating; it has been shown to reduce visual loss and increase the chances of visual improvement.
 |
For more information about the different forms of diabetic retinopathy including diagnosis and treatment, see Diabetic Retinopathy. |
Retinal tears
Small tears can occur in the retina, which can cause fluid from the eye to move under the retina and cause the retina to detach. If retinal tears are discovered before detachment, laser photocoagulation therapy can be used to put small burns around the tear. The scarred tissue adheres the retina nearest the tear to the underlying tissue, blocking it off and preventing retinal detachment.
Laser treatment for correcting refractive errors

- Photorefractive keratectomy (PRK);
- Laser assisted in-situ keratomileusis (LASIK); and
- Laser epithelial keratomileusis (LASEK).
What is PRK?
In PRK, the outer layer of the cornea is removed and the central cornea is treated with laser, reshaping it to the necessary specification. The outer layer is not replaced after the procedure, but regrows over the next few days. The cornea stabilises over the course of the next few months.
What is LASIK?
LASIK uses a precision cutting tool called a microkeratome to create a flap in the outer layers of the cornea. Once this flap is lifted, the underlying layer can then be treated with laser to the correct thickness. Once this is completed, the flap is replaced, allowing rapid healing.
What is LASEK?
LASEK is a hybrid procedure of PRK and LASIK. The outer layer of the cornea is treated with a chemical solution, making it easier to lift off. A corneal flap is then created and pulled back, so the inner layer of the cornea can be treated with laser. The outer layer is then repositioned and stabilises after 3 to 5 days. Another variant of this surgery is called Epi-LASIK, where the outer layer is separated mechanically rather than chemically.
All laser procedures have some side effects, primarily some discomfort after the procedure and temporary visual changes as the cornea heals. However, more serious side effects include:
- Scarring of the cornea, rendering contact lenses unwearable;
- Corneal infections;
- Dry eyes;
- Decrease in contrast sensitivity;
- Glare, haloes and light sensitivity;
- Problems with night driving;
- Red or pink patches within the white of the eye (usually temporary);
- Reduced vision or permanent vision loss; or
- Scratchiness.
LASIK has the lowest rate of side effects, including less post-operative pain and less haze in the cornea than PRK. Formation of haze in the cornea is the major drawback of PRK – approximately 1% of people develop this and it can take years to resolve. In addition, future corrective procedures following PRK are more complicated than for LASIK. However, for individuals undergoing laser eye surgery that only requires a mild or moderate correction, long-term outcomes for PRK and LASIK are very similar.
Which laser eye surgery?

- Individuals requiring only low to moderate corrections;
- Individuals with thin corneas;
- Individuals with recurrent erosion associated with Cogan’s dystrophy of the basement membrane (a condition causing thickening of the base of the outermost layer of the cornea);
- Individuals playing contact sports;
- If complications occurred during LASIK in the opposite eye;
- Patients with flat corneas, steep corneas, deep eye sockets or tight eyelids, causing poor exposure to tools for the LASIK procedure;
- Previous surgery on the conjunctiva; or
- Moderate dry eye prior to surgery.
LASEK has not yet had the benefit of large scale, long-term research; however, studies suggest it has less pain, faster visual recovery and less haze compared to PRK. By avoiding the flap complications of LASIK, LASEK may therefore prove to be the superior procedure in terms of outcomes and side effects. However, LASEK takes longer to perform and requires more instruments, as well as the use of ethanol, which may be associated with other complications for human eye tissue.
Conclusion
The use of lasers has revolutionised the treatment of eye diseases. However, ongoing research is required to determine the long-term outcomes and the best choice for every individual undergoing laser eye surgery.
References
- O’Neill D, Gregson R, McHugh D. Current uses of ophthalmic lasers. BMJ. 1992; 304(6835): 1161–1165. [Abstract | Full Text]
- Bansal AK, Veenashree MP. Laser refractive surgery: technological advance and tissue response. Biosci Rep. 2001; 21(4): 491-512. [Abstract]
- Soubrane G, Bressler N. Treatment of subfoveal choroidal neovascularisation in age related macular degeneration: focus on clinical application of verteporfin photodynamic therapy. Br J Ophthalmol. 2001; 85(4): 483–495. [Abstract | Full Text]
- American Diabetes Association. Standards of medical care in diabetes–2012. Diabetes Care. 2012; 35 Suppl 1: S11-63. [Abstract | Full Text]
- Kohner, EM. Photocoagulation in the prevention of blindness due to diabetic retinopathy: a review. J R Soc Med. 1984 March; 77(3): 227–233. [Abstract | Full Text]
- The Diabetic Retinopathy Study Research Group. Photocoagulation treatment of proliferative diabetic retinopathy. Clinical application of Diabetic Retinopathy Study (DRS) findings, DRS Report Number 8. Ophthalmology. 1981; 88(7): 583–600 [Abstract]
- Early Treatment Diabetic Retinopathy Study Research Group. Early photocoagulation for diabetic retinopathy. ETDRS report number 9. Ophthalmology. 1991; 98(5 Suppl): 766–785. [Abstract]
- Cheung N, Mitchell P, Wong TY. Diabetic retinopathy. Lancet. 2010; 376(9735): 124-36. [Abstract]
- Mitchell, P and Foran, S. NHMRC Guidelines for the Management of Diabetic Retinopathy [online]. Canberra, Australia; 8th June 2008 [cited 10th August 2012]. Available from: URL Link
- Wilkes SR. Current therapy of diabetic retinopathy: laser and vitreoretinal surgery. J Natl Med Assoc. 1993 Nov; 85(11): 841-7. [Abstract | Full Text]
- Diabetic Retinopathy Clinical Research Network (DRCR.net), Beck RW, Edwards AR, Aiello LP, Bressler NM, Ferris F et al. Three-year follow-up of a randomized trial comparing focal/grid photocoagulation and intravitreal triamcinolone for diabetic macular edema. Arch Ophthalmol. 2009 Mar;127(3):245-51. [Abstract | Full Text]
- Grover D, Li TJ, Chong CC. Intravitreal steroids for macular edema in diabetes. Cochrane Database Syst Rev. 2008; (1): CD005656. [Abstract | Full Text]
- Gillies MC, McAllisterIL, Zhu M, et al. Intravitreal triamcinolone prior to laser treatment of diabetic macular edema: 24-month results of a randomized controlled trial. Ophthalmology. 2011; 118(5): 866-72. [Abstract]
- Cho WB, Moon JW, Kim HC. Intravitreal triamcinolone and bevacizumab as adjunctive treatments to panretinal photocoagulation in diabetic retinopathy. Br J Ophthalmol. 2010; 94(7): 858-63. [Abstract]
- Elman MJ, BresslerNM, Qin H, et al. Expanded 2-year follow-up of ranibizumab plus prompt or deferred laser or triamcinolone plus prompt laser for diabetic macular edema. Ophthalmology. 2011; 118(4): 609-14. [Abstract | Full Text]
- Nguyen QD, Brown DM, Marcus DM, et al. Ranibizumab for diabetic macular edema: results from 2 phase III randomized trials: RISE and RIDE. Ophthalmology. 2012; 119(4): 789-801. [Abstract | Full Text]
- O’Keefe M, Kirwan C. Laser epithelial keratomileusis in 2010 – a review. Clin Experiment Ophthalmol. 2010 Mar; 38(2): 183-91. [Abstract]
- National Institutes for Health. LASIK eye surgery [online]. United States of America: Medline Plus, USNational Library of Medicine; 2nd June 2012 [cited 11th August 2012]. Available from: URL Link
- Ambrósio R Jr, Wilson S. LASIK vs LASEK vs PRK: advantages and indications. Semin Ophthalmol. 2003; 18(1):2-10. [Abstract]
- National Institutes for Health. Refractive error [online]. United States of America: Medline Plus, USNational Library of Medicine; 31st July 2012 [cited 26th August 2012]. Available from: URL Link
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.