- Introduction to tooth whitening
- History of bleaching
- Why do teeth become discoloured?
- How we are able to bleach teeth
- Possible side effects of bleaching
- Indications and contraindications
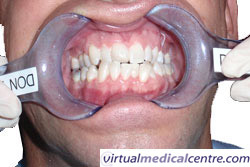
Introduction to tooth whitening

The way our teeth look is of great importance to many people. About a third of us think that our smile is not white enough to be called an attractive smile. Although an attractive smile may be perceived by some as not a big issue, studies have confirmed that a whiter smile plays an important role in perceived self-esteem and success.
These are the following ways in which teeth can be made to appear whiter in order of increasing cost and time:
- Removal of surface stain by the dentist;
- Tooth whitening techniques, which will be discussed throughout this page; and
- Dental restorations that are designed to correct colour and shape of teeth i.e. crowns and veneers.
History of bleaching
The following have been used as bleaching agents for our teeth:
- chlorinated lime;
- oxalic acid;
- chlorine compounds and solutions;
- sodium peroxide;
- sodium hypochlorite;
- mixtures consisting of 25% hydrogen peroxide in 75% ether (pyrozone).
One of the most accepted whitening treatments was proposed in 1961, which was only able to be used on teeth that have a root canal treatment. Putting sodium perborate with water into the tooth and then putting a temporary filling over it was described as the “walking bleach technique.” Nowadays, dentists usually use the modified ‘walking bleach technique’ using a combination of 30% hydrogen peroxide and sodium perborate. Sodium perborate, hydrogen peroxide, and carbamide peroxide are the most used whitening agents today.
Power bleaching, involves the dentist bleaching the outside of the tooth in their clinic. It often involves hydrogen peroxide. This process was modified in 1991 when conventional curing lights were used to help the bleaching process.
A further modification to the light system was when the argon laser was brought out, to once again aid bleaching.
Light sources are not essential to bleaching in dentistry but they do assist with the whitening process.
Why do teeth become discoloured?
The dentist must work out exactly what was the cause of the staining or discolouration so that the appropriate choice of treatment is completed.
Tooth colour is determined by the colour of the dentine, enamel and any stains that may be on the tooth. A combination of these colours forms the overall colour of the tooth.
Dietary causes of discolouration

- wine;
- coffee;
- tea;
- carrots;
- oranges;
- liquorice;
- chocolate;
- tobacco; or
- mouthrinses.
Discolouration that we cannot control
Certain causes of discolouration are beyond our control such as:
- drug-related (tetracycline);
- the way the tooth forms: dystrophic calcification, fluorosis; and
- genetic: congenital erythropoietic porphyria, amelogenesis imperfecta, and dentinogenesis imperfecta.
Other causes related to problems or conditions inside the tooth include:
- death of the nerve;
- root canal treated teeth;
- fillings;
- resorption of teeth; and
- an increase in the thickness of the dentine.
How we are able to bleach teeth
We do not know exactly how bleaching works. Basically, bleaching is a decolourisation or whitening process that can occur in any solution or surface.
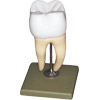
We often use hydrogen peroxide and carbamide peroxide as our bleaching agents, and these work by diffusing through the enamel, and then applying their effect on the underlying dentine.
Figure 1: Teeth whitening (bleaching)
Information on re-publishing of our images
Possible side effects of bleaching
The most commonly reported side effects that bleaching may cause are tooth sensitivity, and irritations on your gums. Typically, the irritation on the gums is caused due to poorly fitting bleaching trays, strong gels being placed for too long, not removing excessive gel, to name but a few of the main causes. Other reported side effects include sore throat, pain in the jaws due to long-term tray use, and minor tooth movement.
Tooth sensitivity is by far the most common side effect reported, and is thought to affect more than half the people who undergo bleaching treatments. The sensitivity is caused mainly because the bleaching agents can diffuse through the tooth structure, and go into the tooth (the pulp) and cause inflammation in this area, which causes pain.
Many bleaching agents also cause dehydration of the teeth, which also makes teeth look whiter. This dehydration can also lead to tooth sensitivity. The sensitivity related to tooth whitening is generally mild, occurs early when the bleaching agent is placed on the tooth, and generally decreases as treatment continues with sensitivity going away following removal of the bleaching agent.
The best way to avoid sensitivity is to use a fluoride gel or sensitive toothpaste prior to using the bleaching agent. Using sensitive toothpaste following the treatment will also help minimise sensitivity. You may also consider using the bleaching tray once every two days rather than once every day.
Additionally, use of potassium nitrate plus fluoride toothpaste two weeks before whitening and during the whitening treatment may be used to minimise sensitivity.
 |
For more information, see Tooth Sensitivity (Dentine Hypersensitivity and Pulpal Disease) |
Whitening agents have been found to negatively impact the look of existing fillings in the mouth as well. In general, dental fillings appear not to change colour at all, or as much as surrounding teeth during the bleaching treatment.
Indications and contraindications

Tooth whitening may be right for you if you have:
- Generalised stains on your teeth;
- Ageing teeth;
- Smoking and dietary stains such as those of tea and coffee;
- Dental fluorosis – fluorosis with multiple spots on teeth may benefit from whitening;
- Tetracycline staining – not all cases of those who have suffered from tetracycline staining will be fully corrected, but many will improve dramatically; and
- There have been changes inside your tooth e.g. death of the nerve or root canal treatment.
Tooth whitening is not right for you if:
- You expect a miracle to happen;
- Your dentist tells you that you have decay in your mouth, gum disease, or infections underneath you teeth;
- You are pregnant;
- You have tooth sensitivity, cracks and exposed dentine – once treated, these teeth can be suitable for whitening;
- You have existing crowns or large fillings in the smile zone – existing crowns or fillings that need to be changed following bleaching may be an indication that bleaching isn’t right for you due to costs; and
- You are in the later years of life and have gum shrinkage and visible yellow roots.
How successful is whitening?
Tooth bleaching is successful in the research that has been done for it, and most importantly, it is inexpensive and less time consuming than other methods to make your teeth look whiter. It is estimated that 90% of people are successful in their whitening treatment.
The following factors affect the success of tooth whitening:
- Age – those who are younger experience a greater reduction in yellowness immediately;
- The type of bleaching done – carbamide peroxide-based products stay active for a lot longer than hydrogen peroxide-based products;
- The concentration of bleaching agent used – the higher the concentration of the agent, the more likely there will be side effects. However, the faster results will be noticed by you;
- The amount of discolouration you have and the cause of the discolouration;
- How much you decide to whiten you teeth at home; if you only whiten your teeth once a twice a month, there will be minimal improvement;
- The design of the tray that is made for you; and
- The number of bleaching treatments done and the time bleached for.
 |
 |
|
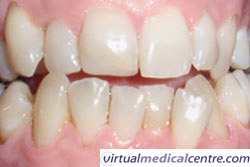
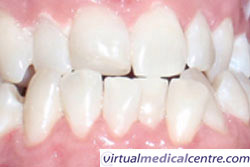
| Figure 2: Pre-bleaching | Figure 3: Post-bleaching |
Who will have the best results?
It is very difficult to know who will respond well to whitening systems. Some people will experience very minor improvement and others will have marked changes.
For instance, it is relatively predictable to bleach teeth of older people with yellowish teeth as this is a normal physiological response of the teeth, and bleaching agents are able to effectively treat this problem.
White dental fluorosis spots do not tend to bleach but will become less obvious as a result of the lightening of the surrounding tooth area.
Some people with staining due to tetracycline ingestion as an infant or toddler may require bleaching for several months before any noticeable change occurs.
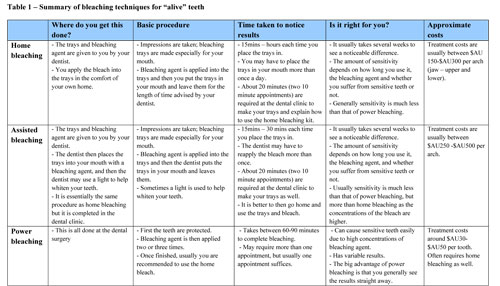
Tooth whitening of teeth that are “alive”
Those teeth that have a blood supply are said to be ‘alive’. A number of methods and approaches for teeth that are alive have been researched. There are methods using different bleaching agents, concentrations, time of usage, method of usage and use of additional activities such as using heat or lasers.
The following table is a basic summary of each technique (click on table to view):
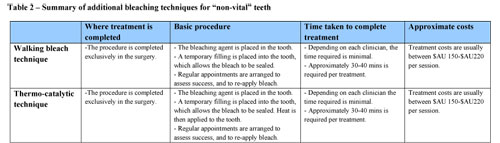
Non-vital whitening
Changes associated with the inside of the tooth can also be a major cause of tooth discolouration. Trauma, previous root canal treatment and death of the nerve can all cause a tooth to become dark yellow, grey, or black. Non-vital teeth are those teeth that do not have a blood supply and have had a root canal treatment completed, or require a root canal treatment.
When bleaching those teeth with changes inside the tooth, more avenues of bleaching can be considered. The following table is a basic summary of each technique (click on table to view):
Kindly written by Dr Akhil Chandra BDSc. (Hons UWA)
Dentist, Whitfords Dental Centre andEditorial Advisory Board Member of the Virtual Dental Centre
More information
 |
For more information on various bleaching techniques for teeth, including home bleaching, assisted bleaching, power bleaching, the thermocatalytic technique and the walking bleach technique, see Teeth Whitening. |
References
- Plotino G, Buono L, Grande NM, Pameijer CH, Somma F. Nonvital tooth bleaching: a review of the literature and clinical procedures. J Endod. 2008 Apr;34(4):394-407.
- Joiner A. The bleaching of teeth: a review of the literature. J Dent. 2006 Aug;34(7):412-9.
- Patzer GL. Measurement of physical attractiveness: truth-of-consensus. J Esthet Dent. 1994;6(4):185-8.
- Dunn JR. Dentist-prescribed home bleaching: current status. Compend Contin Educ Dent. 1998 Aug;19(8):760-4.
- Sulieman M. An overview of bleaching techniques: I. History, chemistry, safety and legal aspects. Dent Update. 2004 Dec;31(10):608-10, 12-4, 16.
- dos Santos Medeiros MC, de Lima KC. Effectiveness of nightguard vital bleaching with 10% carbamide peroxide – a clinical study. J Can Dent Assoc. 2008 Mar;74(2):163-e.
- Reyto R. Laser tooth whitening. Dent Clin North Am. 1998 Oct;42(4):755-62, xi.
- ten Bosch JJ, Coops JC. Tooth color and reflectance as related to light scattering and enamel hardness. J Dent Res. 1995 Jan;74(1):374-80.
- Joiner A, Thakker G, Cooper Y. Evaluation of a 6% hydrogen peroxide tooth whitening gel on enamel and dentine microhardness in vitro. J Dent. 2004;32 Suppl 1:27-34.
- Mello HS. The mechanism of tetracycline staining in primary and permanent teeth. J Dent Child. 1967 Nov;34(6):478-87.
- Kihn PW. Vital tooth whitening. Dent Clin North Am. 2007 Apr;51(2):319-31, viii.
- Haywood VB, Leech T, Heymann HO, Crumpler D, Bruggers K. Nightguard vital bleaching: effects on enamel surface texture and diffusion. Quintessence Int. 1990 Oct;21(10):801-4.
- Leonard RH, Jr., Haywood VB, Phillips C. Risk factors for developing tooth sensitivity and gingival irritation associated with nightguard vital bleaching. Quintessence Int. 1997 Aug;28(8):527-34.
- Titley KC, Torneck CD, Smith DC, Chernecky R, Adibfar A. Scanning electron microscopy observations on the penetration and structure of resin tags in bleached and unbleached bovine enamel. J Endod. 1991 Feb;17(2):72-5.
- Barghi N, Godwin JM. Reducing the adverse effect of bleaching on composite-enamel bond. J Esthet Dent. 1994;6(4):157-61.
- Burrows S. A review of the efficacy of tooth bleaching. Dent Update. 2009 Nov;36(9):537-8, 41-4, 47-8 passim.
- Haywood VB. A comparison of at-home and in-office bleaching. Dent Today. 2000 Apr;19(4):44, 6, 8 passim.
- Sulieman M. An overview of bleaching techniques: 2. Night Guard Vital Bleaching and non-vital bleaching. Dent Update. 2005 Jan-Feb;32(1):39-40, 2-4, 6.
- Pretty IA, Ellwood RP, Brunton PA, Aminian A. Vital tooth bleaching in dental practice: 1. Professional bleaching. Dent Update. 2006 Jun;33(5):288-90, 93-6, 99-300 passim.
- Sulieman M. An overview of bleaching techniques: 3. In-surgery or power bleaching. Dent Update. 2005 Mar;32(2):101-4, 7-8.
- Abbott, P.V. Endodontics and dental traumatology: An overview of modern endodontics. Perth: International Federation of Endodontic Associations 1999.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.