What is breathlessness?
Breathlessness is a common symptom of advanced cancer which is both distressing and frightening for patients and carers. Lung cancer is one of the most common cancers worldwide and one of the most difficult to treat. Breathlessness is particularly problematic in the later stages of lung cancer but may be present even early in the disease. Numerous other cancers may also lead to breathlessness if they spread to the lungs or heart or if they lead to the development of malignant pleural effusion or anaemia. Management focuses on treating your underlying cancer if at all possible, then controlling your breathing symptoms using drugs or by draining fluid from around your lungs. However, these approaches can prove inadequate if effort is not made to address anxiety and other emotional components of breathlessness.
Breathlessness (also called dyspnoea) refers to the sensation of difficulty breathing or shortness of breath. It is a subjective sensation so doctors rely on your description of your symptoms and cannot measure your level of breathlessness by any external means. Breathlessness is a common symptoms in lung cancer and other cancer related illnesses. Approximately half of all cancer patients complain of breathlessness at some point in time and it can be a particularly distressing symptoms for both patients and their carers.
In general, there are four main mechanisms that cause breathlessness in cancer:
- Decreased oxygen levels in the blood stream.
- Increased levels of carbon dioxide in the blood stream.
- Decreased ability of the lung to expand.
- Increased workload associated with normal breathing.
Causes of breathlessness
Cancer of the lung and breast are the most common cancers to cause breathlessness. The former causes breathlessness by invading and obstructing airways in the lung. Breast cancer on the other hand, causes malignant pleural effusions rather than blocking an area in the lungs.
There are however numerous reasons why a patient with cancer may become breathless which can make diagnosis of the cause difficult for clinicians. The main reasons are listed below:
- Lung cancers (either primary or spread to the lungs) can cause obstruction of airways (mass effects), collapse of parts of the lung, pneumonia (due to trapping of bacteria in obstructed airways) or abscess formation. Inflammatory processes in the lung such as fibrosis and lymphangitis (thickening of the lymphatics in the lung which may be caused by cancer cells) can also contribute to shortness of breath. Removal of part of the lung and scarring associated with surgery will lead to shortness of breath.
- Heavy smoking history and coexisting chronic bronchitis or emphysema will also lead to increased breathlessness.
- Malignant pleural effusions (fluid on the lungs) cause breathlessness by impairing the lung’s ability to expand.
- Patients with cancer are also at risk of pulmonary embolism (PE) (clots in the lungs) due to surgery or other prolonged periods of immobility.
- Heart damage- Cancer of the pericardium (membrane surrounding the heart ) can limit the heart’s ability to pump blood to the body. Heart failure causes congestion of blood in the lungs which also causes breathlessness.
- Chemotherapy and radiotherapy treatments can cause pulmonary toxicity and damage to the lungs or heart.
- Anaemia is characterised by insufficient red blood cells to transport oxygen around the body. This leads to a compensatory increase in blood flow and cardiac output in the short term, which can cause later cardiac damage and worsening of angina and congestive heart failure. Anemia is common in leukaemias and other cancers affecting the blood cells.
- Pain does not cause breathlessness in itself, but can result in the patient getting inadequate oxygenation as they are reluctant to take deep breaths.
- General fatigue and cachexia may also cause symptoms of dyspnoea due to the respiratory effort required.
- Anxiety and other emotional factors may also contribute to breathlessness in patients with cancer. A cycle of respiratory panic can develop because the sensation of breathlessness can cause you to become anxious or worried which leads to further breathlessness.
Assessment of breathlessness
Treatment of breathlessness relies on an accurate diagnosis of the likely cause for the symptoms. In order to do this your doctor will take a thorough history and examine your breathing, respiratory system and heart. History will include details of your cancer, treatment to date and detailed questioning about the breathlessness including its onset, severity, timing, associated symptoms and affect on your daily activities. Your doctor may perform some basic tests and investigations to confirm the cause of your breathlessness. The most important of these is the chest x-ray which identifies the cause in the majority of cases. CT may be performed as they can more accurately detect obstruction and lung lesions. Your doctor may also use pulmonary function tests or bronchoscopy (looking into the bronchi) to detect obstruction.
Other tests that may help with a diagnosis include:
- Blood tests to check haemaglobin levels (if anaemia is the suspected cause) and infection markers.
- Oxygen saturation of blood using pulse oximetry.
- ECG (measures electrical activity of the heart), echocardiogram (scan of the heart structure), heart enzymes (if heart attack is a possibility).
- Lung perfusion scans if a clot in the lungs is suspected.
- Biopsy (taking a sample of lung tissue for analysis)
Treatment of breathlessness
Treatment of dyspnoea in cancer patients concentrates on treating the cancer itself and addressing the underlying causes. A multidisciplinary approach is taken, with input from such disciplines as oncology, respiratory physicians, radiation oncologists, surgeons, and palliative care. Treatment of specific problems is highlighted below:
Pleural effusion
Fluid accumulation around the lung prevents it from expanding normally, giving it a sensation of shortness of breath. In cases of large pleural effusion, gas transfer can become compromised. Anti-cancer treatments can improve pleural effusions by killing cancer cells and reducing irritation of the pleura, eventually leading to absorption of the fluid and reduced size of the effusion. Large effusions may need to be drained surgically.
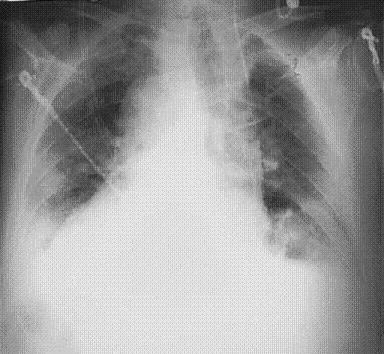
Obstruction of the airways
Airways obstruction may be relieved by shrinking the tumour itself using chemotherapy or radiotherapy or by relieving local obstruction using stents and laser. Treatment should be done to relieve symptoms and improve quality of life even if the cancer itself is not curative.
Lymphangitis/inflammation
Lymphangitis occurs when the lymphatic cells within the lung become thickened with tumour cells. Potent anti-inflammatory drugs such as steroids can reduce the congestion within the lymphatic ducts and improve breathing. Corticosteroids may also be used to decrease the amount of inflammation and oedema around a tumour. Steroids are considered the easiest and most effective drugs for treating dyspnoea but long-term use can cause several side effects that need to be considered.
Oxygen
In conditions where oxygen levels in the blood stream are reduced, symptoms can be improved with the administration of oxygen. Increasing the amount of oxygen breathed in into the lungs causes a larger diffusion gradient between the air in the lungs and the blood stream. This has the effect of causing oxygen to enter the blood stream quicker and increasing circulating oxygen levels in the blood. This can alleviate the shortness of breath. Caution must be taken in people with long standing conditions such as chronic obstructive pulmonary disease (COPD) as oxygen administration can impair respiratory drive. Thus oxygen is only used in patients with what is called reversible hypoxia.
Analgesia
Morphine or narcotic drugs (analgesic agents) are often used in cancer patients to relieve symptoms of breathlessness. Strong opioids such as morphine are also indicated to prevent and eliminate pain in cancer patients.
Coexisting diseases
Patients with lung cancer can get breathlessness from a number of coexisting diseases. As fore mentioned, if the tumour is blocking the airways, bacteria can accumulate behind the tumour and lead to a localised pneumonia. This is also a cause of shortness of breath and should be treated with antibiotics. Often, especially in cigarette smokers, there is an element of emphysema or chronic bronchitis as well as the lung cancer. Sometimes this may respond well to bronchodilators such as Ventolin which opens up the airways.
References
- Cotran, Kumar, Collins 6th edition. Robbins Pathologic Basis of Disease. WB Saunders Company. 1999.
- Houston. Dyspnea Is a Common Symptom of Lung, Breast Cancer. Oncology News 1998; 7(9). Available [online] at URL: http://www.cancernetwork.com/journals/oncnews/n9809ll.htm
- Klee M. Dyspnoea. Symptom Control Info. 2004. Available [online] at URL: http://www.symptomcontrol.com/84.0.html
- Kumar, Clark, 5th edition. Clinical Medicine. W.B. Saunders, London, 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. New York. 2004. [Page 438- Symptom control in severe cancer]
- Murtagh J. General Practice, 3rd Ed. McGraw-Hill, Australia, 2003.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







