- Recovery from a vaginal delivery
- Benefits of a vaginal delivery
- Risks associated with a vaginal delivery
What is a vaginal birth?
 |
|
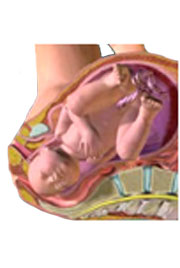
Image courtesy of Blausen Medical Communications. |
Vaginal birth is the delivery of a baby from the uterus (womb), out through the vagina. Occasionally forceps or a vacuum device are required to assist, and this is known as instrumental delivery.
70% of Australian women have vaginal births, while 30% have caesarean deliveries. Of all women delivering babies in Australia:
- 58.1% had a spontaneous vaginal birth;
- 0.4% had a vaginal breech birth (baby is delivered bottom or feet first rather than head first);
- 3.5% were delivered using forceps; and
- 7.2% required vacuum extractions.
The entire process of labour and vaginal birth takes an average of 13 hours in women giving birth for the first time, and 8 hours in women who have given birth before. However, the exact duration varies a great deal from one woman to another. 18 hours of first stage is considered ‘prolonged’, and 1.5-2 hours of second stage is considered ‘prolonged’.
There are three stages of labour:
- The first stage of labour is from the onset of labour until the cervix is fully dilated
- The second stage of labour occurs from when the cervix is fully dilated till the delivery of the baby.
- The third stage is from the delivery of the baby till delivery of the placenta and membranes.
What happens during vaginal birth?
On arrival at hospital, the general condition of the woman is assessed, including the vital signs of pulse, blood pressure, breathing and temperature. The condition of her baby is also checked with a monitor which measures the baby’s heart rate and the length and frequency of contractions of the uterus (CTG).
The woman is encouraged to empty her bladder regularly,and to eat and drink as desired throughout labour. She is also taught breathing techniques which focus on a long slow breath out and on relaxing with the breath out.
Moving around is generally encouraged during the first stage of labour, as this assists with the delivery progressing, and may help the woman to manage her pain.
In terms of preparation, there is no evidence that shaving of the pubic hair, or routine use of an enema (to empty the bowels) on admission has beneficial effects during delivery.

In 90% of cases, contractions start before the waters break. In 10% of cases, the waters breaking is the first sign of labour.
Labour is considered ‘term’ if it occurs from 37 weeks of pregnancy to 41 weeks. Babies born before 37 weeks are known as ‘preterm’. Some women go into labour extremely early, and their baby will require care at a specialist centre. The earliest a baby could survive early delivery if they are in a specialist centre is at 23-24 weeks of pregnancy, however there may be some long term health problems due to the fact it is not well developed before birth.
A doctor or midwife will confirm labour by doing a vaginal examination (inserting a gloved finger into the vagina) in order to check the dilation of the cervix, and whether the membranes have ruptured.
The criteria for labour are regular rhythmical contractions of the uterus (womb), causing cervical effacement (the progressive shortening and thinning of the cervix) and cervical dilation (the increase in cervical opening diameter). The doctor or midwife will also feel the tummy to check how low the baby’s head is in the pelvis, what position it is lying in, and which part of the baby is coming out first. This is called the ‘presentation’ and may be head first (also known as vertex), bottom/feet (or breech) or shoulder first.
Women who have been found to have group B strep (GBS) in their vagina (taken by routine vaginal and rectal swab at 36 weeks) will be given a penicillin injection while they are in labour. This is to reduce the risk of serious infections in the baby.
Monitoring the progress of labour
Once labour has been confirmed, the doctor/midwife will assess progress by monitoring:
- changes in cervical effacement and dilation;
- how far down the birth canal the baby’s head is;
- the quality of contractions of the uterus; and
- the wellbeing of the baby.
Once the cervix is fully dilated (10cm), the woman is said to be in the second stage of labour. Once the baby’s head is on the perineum, the woman is encouraged to assume her preferred birthing position and to push. Contractions may decrease just prior to feeling the urge to push. During the actual pushing stage, the contractions are usually strong and forceful, and may be accompanied with a strong urge to push. This allows the woman to push in time with the contractions of the uterus. Most women feel an increased pressure in their lower back, perineum (area between the vagina and the anus) and rectum during this stage. To many women, the rectal pressure can feel the same as having a bowel movement. In some instances, the doctor may request the women delivers in the lithotomy position (lying on her back with her legs up in stirrups), so that he or she can access the area more easily to deliver the baby or carry out procedures or maneuvers.

There is no evidence that this ‘coaching’ has any benefit over the woman pushing according to her urge to push (which is a reflex), pain of her contractions, and pressure felt from the baby’s head. If epidural anaethesia has reduced the sensation to bear down, coaching is likely to be required.
Pushing against a closed glottis is not generally recommended as it increases blood pressure in the mother, and does not carry an obvious benefit.
If the baby’s heartbeat is reassuring, and the woman is making progress, a woman having her first baby may continue pushing in second stage for up to two hours, or if she has an epidural in place (regional anasethesia) for up to three hours. If pushing lasts longer than this, there is risk to the baby and to the mother’s pelvic floor, so interventions to assist delivery (such as forceps or vacuum) may be required.
The delivery of the baby’s head is generally controlled in part by the doctor/midwife, who places their hand against the baby’s head to keep it flexed (chin towards the chest). The person assisting the delivery may ask the woman to pant or make only small efforts at pushing while the head is crowning, in an attempt to reduce the likelihood of a perineal tear. As the head is being delivered, the woman will feel a stretching or burning sensation. If needed, this process may be assisted by the use of forceps or a vacuum suction cup. If forceps are required, an episiotomy (surgical cut to make the opening of the vagina wider) may be carried out to make more room for the baby to be delivered.
Episiotomy is no longer carried out ‘routinely’. It should only be used when:
- there is high risk of severe perineal tears;
- the baby is getting stuck due to soft tissue blocking their exit (soft tissue dystocia); or
- to speed up the delivery of a baby that is in significant distress.
Once the baby’s head is delivered, the doctor/midwife will feel around the neck for the umbilical cord. If the cord is present around neck, it will either be slipped over the baby’s head or doubly clamped, cut, and unwound from around the neck before the rest of the body is delivered. The rest of the body is generally easier to deliver, requiring more gentle contractions from the woman. The baby may be delivered up and directly onto the mother’s stomach so she can have a cuddle while waiting for the placenta to be delivered. This early ‘skin to skin’ contact helps successful breastfeeding, reduces crying, keeps the baby warm, and improves mother-baby interaction.
When the whole body is delivered, the woman enters the third stage of labour, during which the placenta is delivered.
The delivery of the placenta only requires gentle pushing, and is usually much easier to deliver than the baby. It is essential that the doctor or midwife makes sure that the entire placenta is delivered, and that no parts are left behind, which may result in bleeding or infection.
There are two options for delivery of the placenta and membranes:
- Expectant (passive, physiologic) management – the placenta is delivered naturally, without the use of drugs to contract the uterus (uterotonic agents), clamping the cord, or cord traction (gently pulling on the cord to assist delivery of the placenta); or
- Active management- the cord is usually clamped early, there is controlled traction of the cord, and a drug (such as oxytocin) is given to cause the uterus to contract. The oxytocin is usually given as an intra-muscular injection while the baby is crowning, to reduce the risk of uterine atony (where the uterus does not contract down) which can cause large blood loss after the baby is born (post partum hemorrhage).
A large review studyfound that active management of the third stage of labour resulted in reduced blood loss from the mother, lower risk of postpartum hemorrhage (blood loss of more than 500ml), and reduced risk of prolonged third stage of labour. For this reason, the study concluded that active management should be the routine management of choice for women expecting to deliver a baby by vaginal delivery in a maternity hospital.
After delivery of the placenta, the whole process of labour is complete. The doctor/midwife will examine the placenta and the membranes to ensure that they are intact. The patient’s abdomen will also be felt to check that the uterus is contracting in order to stop the bleeding that occurs when the placenta is torn away.
The woman will also be examined for tears to the cervix or vagina. If present, these may need to be sutured (stitched). If an episiotomy was carried out, it will need to be sutured.
Recovery from a vaginal delivery

Although friends and family are likely to want to visit the new baby, it is important that the mother has plenty of rest. Your partner may need to encourage others to visit in a few days once you have recovered and got to know your baby a little. Managing the expectations of loved ones regarding visiting prior to having the baby may assist with this.
Women are often discharged from hospital the day after the birth, though they may stay longer, particularly in the private setting. It is important to get rest whenever you can, possibly napping when the baby sleeps. Eat well, and drink plenty of fluids. Accept help from others when it is offered. Cleaning and other domestic tasks may need to wait. The hormone relaxin, which softens the joints in the body to allow birth, remains in the system for several weeks after birth. It is important to maintain good posture and avoid heavy lifting following delivery, in order to protect joints and minimise back pain.
High impact exercise is not a good idea in the first weeks after birth as it may damage the joints. Walking or exercise in the water is a better idea initially. A physiotherapist at the hospital may have provided you with gentle abdominal exercises. ‘Sit ups’ are not safe for the first 6 weeks or so after delivery, as they put the back at risk.
Sex may take place whenever you and your partner feel comfortable to do so. This may take a little longer if stitches (which are usually absorbable, so don’t need to be removed) were required for a tear or episiotomy. See sex after childbirth for more information.
Benefits of a vaginal delivery
For a normal low-risk pregnancy, vaginal birth is a safe option for women and their baby. Advantages of vaginal delivery compared with caesarean section include:
- Babies born by vaginal delivery have been found to have a lower incidence of respiratory problems, as it is thought that the contractions that occur during labour help prepare the baby’s lungs for breathing;
- There is less risk of blood loss and infections to the mother;
- Vaginal delivery is a natural process, and one which women’s bodies are designed for. Some women feel a sense of accomplishment and pride at having laboured through a ‘natural’ childbirth; and
- Despite the process of labour and birth itself being painful, women who give birth vaginally usually recover more quickly. However, three months after delivery, there is no difference in pain scores between caesarean and vaginal deliveries.

Risks associated with a vaginal delivery
The risks of vaginal birth include:
- If the baby is in a breech position (bottom or feet first), or if there is an emergency that requires the baby to be delivered quickly, vaginal delivery may be more risky than caesarean section. Babies delivered vaginally in breech position are at risk of oxygen deprivation as a result of cord prolapse (when the umbilical cord enters the vagina despite the baby still being in the womb) or prolonged cord compression due to head entrapment. In some cases, vaginal delivery is simply not possible, and without a caesarean section, the life of the mother or baby may be at risk. Some midwives and doctors are not prepared to attempt vaginal delivery of a baby presenting in a breech position for this reason.
- If there is severe tearing of the perineum during delivery, there can be significant damage to the pelvic floor. This should be repaired by an experienced clinician at the time, and may heal well. In some women, there may be long term consequences, including bladder or bowel incontinence, painful intercourse, or vaginal prolapse (when the walls of the vagina weaken and the bladder or bowel bulges out into the vagina). Women who experience these problems should seek advice and treatment from doctors, midwives, or Women’s Health Physiotherapists.
- If the labour is too prolonged, particularly pushing in the second stage for more than two hours, the blood supply to the nerves that supply the pelvic floor muscles is decreased, reducing the function of these nerves. Rarely, there is long term loss of function of the muscles supplied by these nerves, which may cause incontinence.
More information
 |
For information on birthing statistics,stages of labour, various birthing types and other information related to giving birth, see Birth. |
References
- Symonds E, and Symonds I. Essential Obstetrics and Gynaecology (4th ed). Oxford: Churchill Livingstone; 2003.
- AIHW National Perinatal Statistics Unit. Australia’s mothers and babies [online]. 2006 [Cited 2009 Sep 6] Available from: URL http://www.npsu.unsw.edu.au/NPSUweb.nsf/page/ps22
- Enkin M et al. A guide to effective care in pregnancy and childbirth. (4th ed).Oxford: Oxford University Press; 2000.
- Kerr-Wilson, RH, Parham, GP, Orr, JW Jr. The effect of a full bladder on labor. Obstet Gynecol 1983; 62:319.
- Read, JA, Miller, FC, Yeh, S, Platt, LD. Urinary bladder distention: effect on labor and uterine activity. Obstet Gynecol 1980; 56:565.
- Tranmer, JE, Hodnett, ED, Hannah, ME, Stevens, BJ. The effect of unrestricted oral carbohydrate intake on labor progress. J Obstet Gynecol Neonatal Nurs 2005; 34:319.
- Lawrence A, Lewis L, Hofmeyr GJ, Dowswell T, Styles C. Maternal positions and mobility during first stage labour. Cochrane Database of Systematic Reviews 2009, Issue 2. Art. No.: CD003934. DOI: 10.1002/14651858.CD003934.pub2
- Bloom, SL, McIntire DD, Kelly MA, et al. Lack of effect of walking on labor and delivery. N Engl J Med 1998; 339:76.
- Roberts, CL, Algert, CS, Olive, E. Impact of first-stage ambulation on mode of delivery among women with epidural analgesia. Aust N Z J Obstet Gynaecol 2004; 44:489.
- Basevi V, Lavender T. Routine perineal shaving on admission in labour. Cochrane Database of Systematic Reviews 2008, Issue 1. Art. No.: CD001236. DOI: 10.1002/14651858.CD001236
- Reveiz L, Gaitán HG, Cuervo LG. Enemas during labour. Cochrane Database of Systematic Reviews 2007, Issue 3. Art. No.: CD000330. DOI: 10.1002/14651858.CD000330.pub2
- The Royal Women’s Hospital. Normal labour and birth – low risk [online]. 2006 [cited 2009 Sep 4]. Available from: URL: http://www.thewomens.org.au/NormalLabourandBirthLowRisk
- Beischer N, E MacKay, Colditz P. Obstetrics and the Newborn. 3rd ed. Saunders; London: 1997.
- World Health Organisation. Managing complications in pregnancy and childbirth – A guide for midwives and doctors [online]. 2009 [cited 2009 Sep 4]. Available from: URL: http://www.who.int/reproductive-health/impac/Clinical_Principles/Normal_labour_C57_C76.html#C59 Diagnosis
- Pacifici, GM. Placental transfer of antibiotics administered to the mother: a review. Int J Clin Pharmacol Ther 2006; 44:57.
- Bloom, SL, Casey, BM, Schaffer, JI, et al. A randomized trial of coached versus uncoached maternal pushing during the second stage of labor. Am J Obstet Gynecol 2006; 194:10.
- Yildirim, G, Beji, NK. Effects of Pushing Techniques in Birth on Mother and Fetus: A Randomized Study. Birth 2008; 35:25.
- American College of Obstetricians and Gynecologists. Dystocia and augmentation of labor. ACOG Practice Bulletin # 49, American College of Obstetricians and Gynecologists, Washington, DC 2003.
- Carroli G, Mignini L. Episiotomy for vaginal birth. Cochrane Database of Systematic Reviews 2008, Issue 3. Art. No.: CD000081. DOI: 10.1002/14651858.CD000081.pub2
- Moore ER, Anderson GC, Bergman N. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database of Systematic Reviews 2007, Issue 2. Art. No.: CD003519. DOI: 10.1002/14651858.CD003519.pub2
- Lainez Villabona, B, Bergel Ayllon, E, Cafferata Thompson, ML, Belizan Chiesa, JM. Early or late umbilical cord clamping? A systematic review of the literature. An Pediatr (Barc) 2005; 63:14.
- Rabe, H, Reynolds, G, Diaz-Rossello, J. Early versus delayed umbilical cord clamping in preterm infants. Cochrane Database Syst Rev 2004; :CD003248.
- Cernadas, JM, Carroli, G, Pellegrini, L, et al. The effect of timing of cord clamping on neonatal venous hematocrit values and clinical outcome at term: a randomized, controlled trial. Pediatrics 2006; 117:e779.
- Chaparro, CM, Neufeld, LM, Tena Alavez, G, et al. Effect of timing of umbilical cord clamping on iron status in Mexican infants: a randomised controlled trial. Lancet 2006; 367:1997.
- Strauss, RG, Mock, DM, Johnson, KJ, et al. A randomized clinical trial comparing immediate versus delayed clamping of the umbilical cord in preterm infants: short-term clinical and laboratory endpoints. Transfusion 2008; 48:658.
- Mercer, JS, Vohr, BR, McGrath, MM, et al. Delayed cord clamping in very preterm infants reduces the incidence of intraventricular hemorrhage and late-onset sepsis: a randomized, controlled trial. Pediatrics 2006; 117:1235.
- Yao, AC, Lind, J. Effect of gravity on placental transfusion. Lancet 1969; 2:505.
- Liu S, Liston RM, Joseph KS, Haeman M, Sauve R, Kramer MS. Maternal mortality and severe morbidity associated with low-risk planned caesarean delivery versus planned vaginal delivery at term. Canadian medical association journal. 2007; 17(4): 455-60.
- Spencer P. Controlled cord traction in management of the third stage of labour. Br Med J 1962; 1:1728.
- Elbourne, DR, Prendiville, WJ, Carroli, G, et al. Prophylactic use of oxytocin in the third stage of labour. Cochrane Database Syst Rev 2001; 4:CD001808.
- Prendiville, WJ, Elbourne, D, McDonald, S. Active versus expectant management in the third stage of labour. Cochrane Database Syst Rev 2000; :CD000007.
- Sweet B, Tiran D. Mayes Midwifery: A textbook for midwives (13th ed). Bailliere Tindall; Oxford:1997.
- Villar J, Carroli G, Zavaleta N et al. Maternal and neonatal individual risks and benefits associated with caesarean delivery: multicentre prospective study. British medical journal. 2007; 335: 1025-35.
- Hannah, ME, Hannah, WJ, Hodnett, ED, et al. Outcomes at 3 months after planned cesarean vs vaginal delivery for breech presentation at term: the international randomized Term Breech Trial. JAMA 2002; 287:1822.
- Romano A. Research summaries for normal birth. The journal of perinatal education. 2006; 15(4): 46-9.
- Eason et al. Preventing Perineal Trauma at Childbirth: A Systematic Review. Obs & Gynae 2000;95 (3):464-71.
- McCandlish et al. A randomised controlled trial of care of the perineum during second stage of normal labour. Br J Ob. Gynae. 1998;105:1262-72.
- Mayerhofer et al. Traditional Care of the perineum during birth. A prospective, randomized, multicenter study of 1076 women. J Reprod. Med. 2002;47:477-82.
- De Souza Caroci da Costa and Riesco. A comparison of “hands off” versus “hands on” techniques for decreasing perineal lacerations during birth. J Midwifery and women’s health. 2006;51:106-11.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







