New tool for early detection of melanoma
Australia has the world’s highest incidence of melanoma. In Western Australia, melanoma is the most common cancer diagnosed in the 15-39 year-old age group and the third most common cancer in men and women over 39 years of age. It is increasing in incidence by 3% per year. Currently over 1000 people die annually from the disease in Australia.
In its early stages, the 5-year survival rate of patients is greater than 90% following surgical excision of an in situ tumour. However, following metastasis of the tumour, the 5-year survival rate declines to 5-35%. Due to the correlation between metastasis and declining survival, research studies have attempted to identify potential metastasis as early as possible.
The cancer develops from melanocytes in the skin. When we are exposed to the sun, melanocytes produce more melanin, causing the skin to tan. This helps to protect the underlying cells from DNA damage. However, when we over-expose ourselves to the sun – that is if we are out in the sun all day without protection – we are exposed to too much UV. This UV causes DNA damage and the cells can grow abnormally and become cancerous.
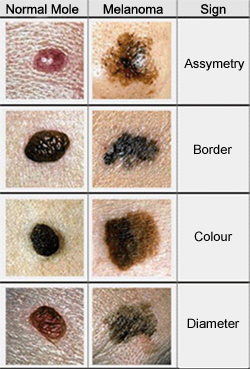
What to look for? Melanoma is characterised initially by appearance: the lesion is asymmetrical in shape, the borders of the lesion are irregular, the lesion may have many colours and a diameter greater than 2 mm – the ABCD rule.
Once a melanoma has started to grow, it can extend downward into the dermis of the skin and develop the ability to infiltrate the blood vessels. The melanoma cells in the blood can circulate in the body and attach to the surface of another organ. The cells group together to form what is known as a micrometastasis. This small group of cells is practically invisible to current diagnostic techniques and can go undetected for years. It is when the cells start to invade the new organ and grow into a tumour that the survival rate of the patient starts to decrease.
Mel Ziman, an Associate Professor at ECU, has developed precise techniques and identified correct genetic markers that can be used to detect cancer cells in the blood of patients with melanoma, even at very early stages.
A/Prof Ziman explained that the genetic markers she is using are able to detect melanoma cells in the blood of patients. These markers are not normally found in the blood of healthy volunteers with no melanoma.
"If the cells are detected in the blood stream early it will alert the medical specialists to be extra vigilant when treating the patient, and in specific cases will ensure entry into specific treatment and chemotherapy programs. It may even provide a set of molecular targets for chemotherapy in the future.
"These exciting results are now the basis of further research aimed at detecting and understanding melanoma metastasis.
"Surprisingly and of some concern is the finding that markers of melanoma cells are still detected in the blood of patients who had melanomas removed many years ago" she said.
A/Prof Ziman is not sure whether this implies that the tumour will spread but it is without doubt that further research is urgently needed to determine the parameters that cause a melanoma cell to form a metastatic tumour in other parts of the body.
A/Prof Ziman initiated the formation of the ECU Melanoma Research Foundation in 2007 to raise awareness of melanoma and to raise funds for this important research.

The Foundation is funded by local sponsors and supporters with matching funding from ECU. All funds received go to research, and donations are tax deductible.
Your help is urgently required in the research and with fundraising events, so please contact Mel on 63045171 or 0419929851, or email m.ziman@ecu.edu.au or visit the website.
Dates
Tags
Created by:

 Login
Login














