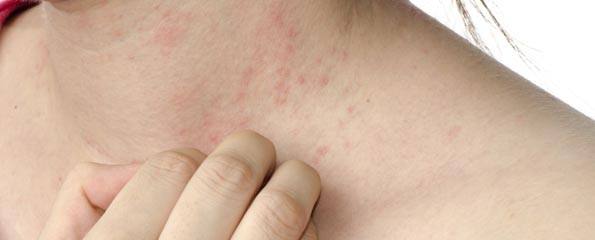
The future of treating psoriasis is biologic
Psoriasis is an incurable skin disorder, underpinned by abnormal autoimmune response,1 which has a significant and negative impact on quality of life.2 A range of treatments are available, and effective treatment has been shown to improve quality of life.2 However, the most appropriate treatment varies depending on the extent of skin lesions, their impact on quality of life and the patient’s priorities.1 Therapy has improved considerably in the last 5 years with the approval of biologics for the treatment of severe disease.3 However, these treatments remain inaccessible to the majority of patients3 and are an expensive treatment option.1 The challenge for practitioners is to apply the rapidly expanding evidence base for psoriasis treatment to the patient’s individual circumstances, to determine the most effective treatment plan. For more information about the different treatment options for psoriasis and when they should be used, see Treatment Options for Psoriasis.
Developing a treatment plan
An individualised approach to treatment is mandatory.1 Psoriasis affects 2.5% of the Australian population4 and the primary symptom of the condition is papulosquamous skin rash.5 However, often there are also other physical symptoms (e.g. arthritis), comorbidities (e.g. autoimmune and nutritional conditions6) and an adverse impact on quality of life.7 When determining the best course of management, the extent, severity and site of psoriatic lesions are not the only important factors. The impact of the disease on quality of life and daily functioning is of key importance.1,8
“Treatments need to be implemented that match the impact that the disease is having on quality of life. A severe impact may warrant more aggressive treatments while over-the-counter topical medications are appropriate when the impact is minimal,” says Professor Rodney Sinclair, a Melbourne University academic and consultant dermatologist at Epworth Specialist Centre. While the severity of a patient’s skin lesions influences their psychological response to the condition, it’s important to realise that the extent of physical symptoms does not predict the quality of life impact of psoriasis.7 Practitioners must, therefore, communicate effectively with patients to understand not only what skin and other physical symptoms they experience, but also how, and to what extent, these reduce quality of life.2
It’s also important to bear in mind that treatment itself can have a considerable impact on daily functioning because it is time consuming2 and/or inconvenient.9 Making treatment more convenient is just as important for many patients as their clinical outcomes.9 The side effects of psoriasis treatment can be substantial1 and evidence about these should be considered when determining a management strategy.10 Professor Sinclair believes that, “the most important consideration when determining a treatment plan for someone with psoriasis is, ‘is the treatment worse than the disease itself?’”
Unfortunately the most safe and effective treatments, new-age biological agents, are rarely the most feasible. “The annual cost of biologic agents approaches the gross domestic product per person in Australia and so it is simply not possible for the Government to subsidise their use for all psoriasis sufferers,” says Professor Sinclair. “The challenge for Government is to make these treatments available to those that really need them: The people with severe psoriasis for whom all other treatments have not been effective.”
Practitioners play a vital role in trialling less effective treatments, to determine an affordable and effective treatment regimen for each patient.1 Before starting a patient on biological agents, it is usual to trial topical, photo, and systemic therapies, and this step-up approach to treatment is mandatory for patients to be eligible for Pharmaceutical Benefits Scheme subsidy.3
Topical treatments
The majority of psoriasis patients (87%) use topical therapies, either as monotherapy,1 or in combination. This approach allows dose reduction for relatively aggressive systemic or photo therapy,2 both of which have more severe, and often dose-limiting, side effects.3 Topical treatments are safe and effective and there are numerous options.11 “Common topicals used to treat psoriasis include tar, dithranol, topical corticosteroids and vitamin D analogues,” Professor Sinclair said, adding that, “People often combine topical treatments.”
The best trial evidence for topical therapies is a fixed dose combination of corticosteroid/vitamin D analogue. As monotherapy, vitamin D analogues and corticosteroids have similar efficacy; however, corticosteroids have a favourable side effect profile. Dithranol and coal tar therapy are effective but unpopular with patients because they are unsightly and cause localised skin reactions.11 Preparations which are difficult to apply may reduce patient compliance and the effectiveness of treatment.12
In cases of mild psoriasis (affecting < 5% of body surface area) topical agents alone are typically sufficient to control skin lesions.1 However, up to 20% of patients who experience moderate to severe psoriasis14 require more aggressive treatment and in these cases topical treatments may be used in combination with UV or systemic therapy.11
UV Therapy
UV exposure controls psoriatic skin lesions by inducing apoptosis of T lymphocytes in the affected dermal and epidermal tissues. Phototherapy should be considered for adult patients with moderate-severe psoriasis and those who fail to respond adequately to topical treatments.1 There are two types of phototherapy approved for the treatment of psoriasis; targeted UVB therapy,1 and PUVA photochemotherapy, a combination treatment involving psoralen and UVA exposure.13 PUVA therapy is most appropriate for thick lesions which UVB rays cannot penetrate. UVB phototherapy should be trialled in patients with thin lesions and those which respond to sun exposure.1
“A dermatologist will normally recommend a 6 week course of [UVB] therapy involving about 20 individual treatment sessions. This therapy can lead to complete remission of psoriasis and is particularly useful for people who don’t have regular access to sunlight or who have a skin type that gives them a higher risk for skin cancer,” says Professor Sinclair. PUVA therapy is also effective with 60% of patients achieving good response after 12 weeks treatment.1 However, side effects including erythema, pruritus and nausea can occur3 and there is an increased risk of skin cancer associated with UV therapy.1 Phototherapy is also inconvenient because it requires frequent clinic attendance.1
Systemic therapy
Systemic therapies are effective; however, with the exception of the oral retinoid acitretin (e.g. Neotigason) (10–50 mg orally) they all have immune-suppressing effects.3 Acitretin, which inhibits helper T lymphocyte activity is more effective in higher doses. It has a relatively slow onset of action, taking 3–6 months to achieve control of psoriatic lesions. Many patients withdraw from treatment before control has been achieved because they are unable to tolerate the skin and mucosal side effects.1 Lower doses which may limit side effects are less effective1 and acitretin has limited effectiveness in the treatment of chronic plaque psoriasis (the type responsible for up to 90% of cases).3
The immune-suppressing effects of other systemic agents are typically dose-limiting, for example with cyclosporin (e.g. Cyclosporin Sandoz, Neoral, Sandimmun) (2–5 mg/kg daily)3 which controls psoriasis by inhibiting the translocation of activated T lymphocytes and in doing so blocks the inflammatory skin response.1 While effective in up to 70% of patients,1 it is usually limited to 12–24 months use due to side effects including hypertension, nephrotoxicity and malignancy.3 It may be used in combination or in rotation with topical therapies so that the dose can be reduced and the period of treatment extended. Drug-drug interactions warrant consideration when prescribing cyclosporin as it is metabolised by the cytochrome P450 system.1
Some patients achieve adequate control with methotrexate (5–25 mg weekly orally or by intramuscular injection),3 which is the systemic drug of choice.1 It controls psoriatic lesions by decreasing RNA and DNA synthesis in the T lymphocytes and keratinocytes of affected skin and also acts downstream by decreasing cytokine and messenger protein production. Methotrexate has a favourable side effect profile compared to acitretin and fewer drug-drug interactions compared to cyclosporin.1 However, it takes up to 3 months (about twice as long as cyclosporin) to achieve remission, partly because it is necessary to start at a low dose and titrate gradually to reduce side effects. In addition, regular monitoring (monthly during dose titration and bimonthly once a stable dose has been found) including full blood count and liver function tests are mandatory, as is folate supplementation to reduce the risk of gastrointestinal and bone marrow toxicity.3 Up to 70% of patients achieve a good response with methotrexate.1
Systemic therapies should be considered for patients with moderate and severe disease (affecting > 5% and > 20% of body surface area respectively). It should also be prescribed for patients who fail to respond to topical therapies even if disease is mild (affecting < 5% of body surface area). Similarly, systemic treatment is necessary for all patients with psoriatic lesions affecting the hands or under the nails, as well as those with comorbid psoriatic arthritis.1
Biological agents
Biological agents target the processes which underpin the development of psoriatic lesions, for example by inhibiting pro-inflammatory cytokines or T cells.3 They may be used to complement traditional therapies or to replace them in cases of refractory disease, and are being rapidly developed.1 “In the last few years six or seven additional new treatments have become available,” says Professor Sinclair. “Clinical trials are currently underway to assess a further three new agents for the treatment of psoriasis.” These include seven trials enrolling Australians with psoriasis who would like to be involved in testing the new drugs (see table at the bottom of this article for details).
Although immunosuppressive effects and lack of long-term safety data are of concern,3 biological therapies for psoriasis treatment have favourable short-term safety and efficacy profiles compared to traditional therapies.1 “Biologic therapies work magnificently, with few side effects and excellent response rates,” says Professor Sinclair. For example, anticytokine drugs, the most effective of the biologics trialled to date achieve good response in the majority of patients with moderate disease who have failed to respond to traditional therapies,1 and appear to be effective regardless of previous response to traditional therapies.3
In Australia, three anticytokine agents which target tumour necrosis factor alpha (TNF-α) are approved, etanercept (e.g. Enbrel) (50–100 mg per week for up to 12 weeks reducing to 50 mg weekly), infliximab (e.g. Remicade) (5 mg/kg at 2, 4, 6 and 12 weeks initially then every 6–8 weeks for maintenance), and adalimumab (e.g. Humira) (80 mg starting dose followed by 40 mg one week later with fortnightly maintenance with 40 mg).3 Infliximab, a murine human immunoglobulin G chimera which targets membrane-bound TNF-α, has the best demonstrated efficacy achieving good response in 64–82% of patients at 10 weeks. Adalimumab, a fully human monoclonal IgG antibody which targets both soluble and membrane-bound TNF-α, achieves good response in 49–60% of patients receiving fortnightly maintenance doses and up to 75% of those receiving weekly maintenance doses. Etanercept, a soluble dimeric fusion protein which targets TNF binding sites on immunoglobulin G1, is less effective, with 47–49% of patients achieving response after 12 weeks treatment.1
A further class of anticytokine biologics used in psoriasis treatment target interleukins (IL). Ustekinumab (e.g. Stelara) works by blocking IL-12 and IL-23 preventing them from activating T cells. Trials conducted to date have reported up to 63.4% good response rate at 12 weeks with a 45 mg dose and > 70% response at 12 weeks with 90 mg dose. The side effect profile is similar to placebo.1
T-cell targeted therapies (efalizumab and alefacept), have proven less effective than anticytokines to date. Alefacept blocks interaction between T cells and antigen presenting cells, preventing activation of T cells. However, alefacept is effective for only 20–25% of patients at 12 weeks.1 Efalizumab a chimeric monoclonal anti-CD11a antibody which inhibits interaction between dendritic and T cells. It is about twice as effective as alefacept; however, it was withdrawn in the US1 and Australia15 after four cases of the deadly progressive multifocal leukoencephalopathy were reported in association with its use.1
Currently cost1 and the limited availability of PBS subsidies are key factors limiting their use.3 “If these agents were cheaper, all people with psoriasis would use them. With some agents a single injection will maintain complete remission of psoriasis for 3 months. If I had not seen it in my own patients I would have said the results are ‘too good to be true’. However, these agents are relatively new, having only been available for the last 5 to 10 years and, therefore, the long-term effects of using them are still not known.”
The future looks biologic
Despite a need for long-term safety and efficacy data, biological agents have already proven highly effective. “Given how effective the current generation of biologic agents is in treating psoriasis, the challenge for future development is to make them cheaper. Biologic agents are manufactured using bacteria and the process is difficult to automate. Hopefully advances in manufacturing will lead to cost reduction and make biologic agents accessible to a greater proportion of psoriasis sufferers.”
Given the significant psychological and quality of life implications of the disease,2 and its high prevalence in the general population,4 cheaper biological agents offer great promise for psoriasis sufferers.1 While traditional topical, systemic and photo therapies are still the mainstay of treatment, biological agents are almost certain to play a more prominent role in psoriasis therapy in the near future.1
 |
For more information about psoriasis including types, treatments and more, see Psoriasis. |
Study name | Drug tested | Locations | Contact details |
A Long Term Study To Evaluate The Safety And Tolerability Of CP-690,550 For Patients With Moderate To Severe Chronic Plaque Psoriasis NCT01163253 For full eligibility inclusion, click here. | CP-690,550 | NSW- Pfizer Investigational VIC- Pfizer Investigational | United States- PfizerCT.gov |
A Multiple Dose Escalation Study of ASKP1240 in Subjects With Moderate to Severe Plaque Psoriasis For full eligibility inclusion, click here. | ASKP1240 | SA- CMAX Adelaide WA- Linear Research | Astellas Pharma |
Safety, Tolerability, Pharmacokinetics, Pharmacodynamics, and Clinical Effects of AMG 811 in Subjects With Psoriasis NCT01510951 For full eligibility inclusion, click here. | AMG 811 | QLD- Herston WA- Nedlands | Amgen Call Centre (United |
A Phase 3 Study in Participants With Moderate to Severe Psoriasis (UNCOVER-2) NCT01597245 For full eligibility inclusion, click here. | Ixekizumab AND | NSW- Sydney (recruiting) St Leonard (not yet VIC- Box Hill (not yet Malvern East (not yet | Eli Lilly (United States) |
SHP-141C in Plaque Type Psoriasis For full eligibility inclusion, click here. | SHP-141C and | VIC- Nucleus Network | Jeffery Wong |
A Phase 3 Study in Participants With Moderate to Severe Psoriasis (UNCOVER-1) For full eligibility inclusion, click here. | LY2439821 | NSW- Kogarah (recruting) QLD- Benowa (recruiting) Woolloongabba(recruiting) SA- Adelaide (not yet recruiting) VIC- Carlton (recruiting) Parkville (not yet recruiting) WA- Fremantle (recruiting) | Eli Lilly (United States) |
A Double Blind Study in Pediatric Subjects With Chronic Plaque Psoriasis, Studying Adalimumab vs. Methotrexate NCT01251614 For full eligibility inclusion, click here. | Adalimumab | NSW- Kogarah (not yet | Susan Williamson (United |
References
- Herrier RN. Advances in the treatment of moderate-severe psoriasis. Am J Health Sys Pharm. 2011; 68: 795-806. [Abstract ]
- Krueger G, Koo J, Lebwohl M, et al. The impact of psoriasis on quality of life: Results of a 1998 National Psoriasis Foundation patient-membership survey. Arch Dermatol. 2001; 137(3): 280-4. [Abstract | Full text]
- Sullivan R, Preda V. Treatments for severe psoriasis. Australian Prescriber. 2009; 32: 14-18. [Full Text]
- Magin P, Adams J, Heading G, et al. Patients with skin disease and their relationships with their doctors: a qualitative study of patients with acne, psoriasis and eczema. Medical Journal of Australia. 2011; 190: 62-64. [Full Text]
- Griffiths CE, Barker JN. Pathogenesis and clinical features of psoriasis. Lancet. 2007; 370(9583): 263-71. [Abstract]
- Christophers E. Psoriasis: Epidemiology and clinical spectrum. Clin Exp Dermatol. 2001; 26(4): 314-20. [Abstract]
- Barankin B, DeKoven J. Psychosocial effects of common skin disorders. Can Fam Phys. 2002; 48: 712-8. [Abstract | Full Text]
- Foulkes AC, Grindlay DJC, Griffiths CEM, et al. What’s new in psoriasis? An analysis of guidelines and systematic reviews published in 2009-10. Clin Experimental Dermatol. 2011; 36: 585-9. [Abstract | Full text]
- Merideth F, Ormerod AD. Patient preferences for psoriasis treatment: process characteristics considered more important than outcome attributes. Exp Rev Pharmacoecon Outcomes Res. 2012; 12(2): 145-7. [Abstract | Full Text]
- Chuh A, Wong W, Zawar V. The skin and the mind. Aust Fam Phys. 2006; 35(9): 723-5. [Full Text]
- Murphy G, Reich K. In touch with psoriasis: topical treatments and current guidelines. J Eu Acad Dermatol Venereol. 2011; 25(S4): 3-8. [Abstract | Full text]
- Traub M, Marshal K. Psoriasis- Pathophysiology, conventional and alternative approaches to treatment. Alt Med Rev. 2007; 12(4): 319-31. [Abstract | Full Text]
- Stern RS, Lunder EJ. Risk of squamous cell carcinoma and methoxsalen (psoralen) and UV-A radiation (PUVA): A meta-analysis. Arch Dermatol. 1998; 134(12): 1582-5. [Abstract | Full text]
- Gelfand JM, Neimann AL, Shin DB, et al. Risk of myocardial infarction in patients with psoriasis. JAMA. 2006; 296(14): 1735-41. [Abstract | Full text]
- Sullivan JR, Preda V. Treatments for severe psoriasis: update. Australian Prescriber. 2009; 32(50). [Full Text]
Dates
Tags
Created by:

 Login
Login