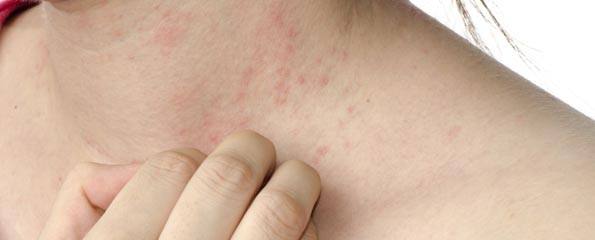
Summer and psoriasis: Helping patients get the sun they need and want
Summer is approaching and most patients (and their doctors!) are thinking of ways to devote as much of their busy schedules as possible to soaking up the summer sun. Not so for the 2.5% of Australians who experience psoriasis;1 these patients are more likely to be strategising how to get through the summer without wearing shorts, t-shirts and other clothes which expose their psoriatic skin. Psoriasis can be embarrassing at any time of year, but the psychological impact is greater in summer, when patients have to choose between soaking up the sun and swimming at the beach, or covering up their skin lesions to avoid humiliation. Yet these activities are not just important for summer fun, they are also important treatment measures; exposure to summer sun and salt water reduces psoriatic lesions. Patients who can get their condition under control before summer begins and find the confidence to expose their skin will not only enjoy the sun and surf, they’ll also be treating their condition at the same time. For more information about psoriasis including types, treatments and more, see Psoriasis.
Recognising psoriatic skin
The key symptom of psoriasis is papulosquamous skin rash.2 Skin lesions may occur at any site,3 although the elbows, knees, scalp and trunk are most commonly affected.4 The proportion of body surface area affected depends on the severity of disease. While the majority (80%) of patients have mild disease which affects < 2% of body surface area, a substantial minority of patients (20%) have extensive lesions.3 There are also physical symptoms including itching and burning sensations.5 However, according to Dr Rodney Sinclair, a Professor of Dermatology at Melbourne University and consultant Dermatologist at the Epworth Specialist Centre, “the biggest issue for people with psoriasis is a feeling of embarrassment,” about the appearance of their skin.
Why psoriasis presentations increase in summertime
Summer weather and clothing which exposes the skin go together. Psoriasis patients who have hidden their skin lesions with clothing in the cooler seasons may therefore be more likely to seek treatment in the summer months. Professor Sinclair noted that, “people with psoriasis commonly seek treatment in summer when they want to expose their skin regularly… so that they can begin treatment, get the condition under control and then get out and enjoy the season.”
Although UV exposure is a treatment option for the condition and spontaneous remission of psoriatic lesions is more common in summer,6 the need to expose more skin to cope with warmer conditions means that psychological comorbidities may be exacerbated at this time,7 when “there is a desire to wear summer clothing … People with psoriasis often find themselves in situations where, due to embarrassment, they have to exclude themselves from activities. For instance, they may avoid going to the beach for a swim because they don’t want to be in a situation where removing clothing is required,” said Professor Sinclair.
A large proportion of psoriasis patients report feeling embarrassed to participate in swimming and other sports due to their skin lesions. About two-thirds (64%) report avoiding short sleeved shirts, summers dresses and shorts in an attempt to hide their condition.8 However, wearing long pants, skirts or sleeves which are inappropriate for the summer weather can also draw unwanted attention.7
Summer fun is a great prevention strategy
Getting out and enjoying the summer sun is a useful strategy for preventing psoriasis. “Sunlight and salt water help psoriasis,” Professor Sinclair said. However, summer recreation is also an opportunity to relax, enjoy the weather and get some exercise, all of which are important measures for reducing stress,9 a key risk factor for psoriasis.10
When managing psoriasis to control symptoms before summer, measures to reduce stress at work and at home can also be instituted. Resolving personal conflicts and postponing major life changes like moving house might be important measures for some patients. Others might need support to say ‘no’ to too much responsibility at work and put aside time for rest and recreation. Techniques such as muscles relaxation and deep breathing can also help patients deal with stress.10
Another important prevention measure is quitting smoking. Smoking patients require support in their attempt to quit.
Getting psoriasis under control
Getting treatment started early is an important measure to help psoriasis patients enjoy their summer. Professor Sinclair notes that the topical treatments are the mainstay of psoriasis therapy but, “must be used daily for 6–8 weeks to achieve and maintain benefit.” While topical treatments are safe and effective for many patients, those with severe disease usually need to combine topicals with systemic and/or phototherapies to achieve adequate symptom control.11
Instituting treatment well before the start of summer allows time to step up to more aggressive treatments, should topical therapy fail to achieve adequate results. Professor Sinclair believes, “Treatments [need to] match the impact that the disease is having on quality of life.” Thus, in summertime when the psychological impact of psoriasis is increased, more aggressive treatment may be warranted. Recent advances in treatment, including the approval of numerous biological therapies, provide greater and more effective treatment options.12
 |
For more information about the different treatment options for psoriasis and when they should be used, see Treatment Options for Psoriasis. |
Soaking up the summer sun without psoriasis
The range of treatments currently available for psoriasis means it is possible to get the associated skin symptoms under control2 before summer, and allowing patients to enjoy the summer sun. The combination of sun, salt water and recreation all have positive effects on psoriatic skin lesions.6,10 Practitioners should focus on identifying patients in need of treatment before the onset of summer and exacerbation of psychological morbidity. Instead of strategising to avoid skin exposure, psoriasis patients need support and advice which will enable them to confidently show off their skin and soak up the summer sun.
References
- Magin P, Adams J, Heading G, et al. Patients with skin disease and their relationships with their doctors: a qualitative study of patients with acne, psoriasis and eczema. Medical Journal of Australia. 2011; 190: 62-64. [Abstract | Full text]
- GriffithsCE, Barker JN. Pathogenesis and clinical features of psoriasis. Lancet. 2007; 370(9583): 263-71. [Abstract]
- Gelfand JM, Neimann AL, Shin DB, et al. Risk of myocardial infarction in patients with psoriasis. JAMA. 2006; 296(14): 1735-41. [Abstract | Full text]
- Dediol I, Buljan M, Buljan D, et al. Associations of psoriasis and alcoholism: psychodermatological issues. Psychiatria Danube. 2009; 21(1): 9-13. [Abstract | Full Text]
- Krueger G, Koo J, Lebwohl M, et al. The impact of psoriasis on quality of life: Results of a 1998 National Psoriasis Foundation patient-membership survey. Arch Dermatol. 2001; 137(3): 280-4. [Abstract | Full text]
- Lassus A, Geiger JM, Nyblom M, et al. Treatment of severe psoriasis with etretin. Br J Dermatol. 1987; 117(3): 333-41. [Abstract]
- Barankin B, DeKoven J. Psychosocial effects of common skin disorders. Can Fam Phys. 2002; 48: 712-8. [Abstract | Full Text]
- Ramsey B, O’Reagan M. A survey of the social and psychological effects of psoriasis. Br J Dermatol. 1988; 118(2): 195-201. [Abstract]
- Beyond Blue. Fact Sheet 6: Reducing stress. 2010. [cited 22 September 2012]. Available from: [URL Link]
- Chuh A, Wong W, Zawar V. The skin and the mind. Aust Fam Phys. 2006; 35(9): 723-5. [Full Text]
- Murphy G, Reich K. In touch with psoriasis: topical treatments and current guidelines. J Eu Acad Dermatol Venereol. 2011; 25(S4): 3-8. [Abstract | Full text]
- Herrier RN. Advances in the treatment of moderate-severe psoriasis. Am J Health Sys Pharm. 2011; 68: 795-806. [Abstract]
Dates
Tags
Created by:

 Login
Login