- What is oral thrush?
- Statistics of oral thrush
- Risk factors for oral thrush
- Progression of oral thrush
- Symptoms of oral thrush
- Clinical examination of oral thrush
- How is oral thrush diagnosed?
- Prognosis of oral thrush
- Treatment of oral thrush
- Oral thrush prevention
- References
What is oral thrush?

As the Candida species are a part of the normal flora that lives in the mouth, it is the change in the normal oral environment, rather than the actual exposure or ‘infection’ per se, that results in the occurrence of this disease.
Statistics of oral thrush
Oral thrush is most common in the very young, the very old or the very sick. It is most commonly associated with HIV. It is estimated that 95% of individuals who are HIV positive will at some point develop oral thrush.
It is also seen frequently in people undergoing chemotherapy and those in healthcare facilities. Healthy adults and children can also present with oral thrush if they do not maintain good oral hygiene, although this is uncommon.
About 45% of infants on breastmilk and almost 60% of people who wear loose or ill-fitting dentures develop oral thrush.
Risk factors for oral thrush
Candida species are a part of the normal flora of the mouth. Any changes in the oral environment can cause the Candida species to multiply and colonise the mouth, leading to oral thrush.
Immunocompromised people, such as those with HIV/AIDS or cancer, have the highest risk of developing the disease. Age can also be a factor, since the disease is more common in the very young and very old. Saliva plays a major role in the prevention of Candidal overgrowth; therefore, disturbances to normal salivary physiology and decreased salivary flow represent major risk factors for oral thrush.
Medications like antibiotics, steroids and immunosuppressants in the treatment of malignancies are all also causative factors of the occurrence of oral thrush.
Oral thrush can also occur due to some behavioural factors such as poor oral hygiene, dehydration and insufficient nutrition to the body.
Progression of oral thrush
Oral thrush progresses slowly in healthy individuals and can resolve on its own when the oral environment becomes normal. Oral antifungal medication often helps in the regression of the disease.
However, if it is left untreated in people with HIV/AIDS, it can progress rapidly to the throat, causing difficulty in swallowing medication and food, leading to an early death.
Symptoms of oral thrush

- Burning pain in the mouth;
- Altered taste sensation;
- Difficulty swallowing liquids and solids; and/or
- Creamy white cheesy or curd-like plaques.
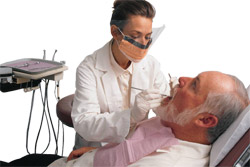
Clinical examination of oral thrush
On examination, the dentist will most commonly see white cheesy or curd-like plaques on the tongue, inner cheek or palate which, when scrubbed, will leave a reddish site that may bleed slightly on contact. Although there are different clinical manifestations of oral thrush, the most familiar one is called the pseudomembranous type, and has the above characteristics.
How is oral thrush diagnosed?
Oral thrush is characterised as a white lesion in the mouth. Misdiagnosis is likely if individuals try to diagnose themselves, as there are many other white lesions that can also occur in the mouth. It is therefore necessary to seek professional advice before self-treatment.
Clinical signs and symptoms, in conjunction with a thorough medical history, are generally used by the dentist to make a provisional diagnosis of oral thrush. Laboratory tests are done to confirm the diagnosis. These may include:
- Swabbing: Using sterile wooden spatulas, the lesion is scraped for a sample and tested;
- Imprint culture: Sterile plastic foam pads are dipped in a special solution and pressed against the mucosal surface for 60 seconds;
- Collecting saliva: 2 mL of mixed whole unstimulated saliva is spat into a sterile universal container, which is vibrated on a bench vibrator for 30 seconds to disaggregate the organisms;
- Oral rinse sample: The mouth is rinsed with 10 mL of phosphate-buffered saline (0.1 M, pH 7.2) for 60 seconds which is collected in a sterile container;
- Incisional biopsy: A sample of the lesion is cut and removed to be tested in the lab.
Prognosis of oral thrush
With effective and appropriate treatment, the prognosis of oral thrush is good. However, relapse of the disease can occur if the underlying predisposing factors have not been treated.
Treatment of oral thrush
Maintaining good oral hygiene and using topical antifungal medication are usually adequate for uncomplicated oral thrush. Tablets can be used in case of severe infection, and these are normally available through a prescription. The topical medication, however, may be readily available over-the-counter in pharmacies. Nevertheless, further dental advice is essential if the disease persists for more than 7–10 days or recurs.
Oral thrush prevention
- Maintaining good oral hygiene, which includes brushing and flossing;
- For those who wear dentures, it is important to use well-fitted dentures;
- Since oral thrush can be asymptomatic, having regular dental check-ups is vital, especially for people who are immunocompromised;
- A healthy balanced diet and daily exercise can help maintain a good immune system and thus reduce the occurrence of oral thrush;
- Sufficient fluid intake should be taken to keep the mouth moist; and
- Reducing sugar consumption and avoiding smoking and alcohol are measures that can be taken to maintain a strong immune system.
References
- Roseff SA, Sugar AM. Oral and esophageal candidiasis. In: Bodey GP (ed). Candidiasis: Pathogenesis, diagnosis and treatment. New York: Raven Press; 1993. [Book]
- Manning DJ, Coughlin RP, Poskitt EM. Candida in mouth or on dummy? Arch Dis Child. 1985;60(4):381-2. [Abstract | Full text]
- Berdicevsky I, Ben-Aryeh H, Szargel R, Gutman D. Oral Candida in children. Oral Surg Oral Med Oral Pathol. 1984;57(1):37-40. [Abstract]
- Lucas VS. Association of psychotropic drugs, prevalence of denture-related stomatitis and oral candidosis. Community Dent Oral Epidemiol. 1993;21(5):313-6. [Abstract]
- Arendorf TM, Walker DM. The prevalence and intra-oral distribution of Candida albicans in man. Arch Oral Biol. 1980;25(1):1-10.[Abstract]
- Aldred MJ, Addy M, Bagg J, Finlay I. Oral health in the terminally ill: A cross-sectional pilot survey. Spec Care Dentist. 1991;11(2):59-62. [Abstract]
- Cumming CG, Wight C, Blackwell CL, Wray D. Denture stomatitis in the elderly. Oral Microbiol Immunol. 1990;5(2):82-5. [Abstract]
- Holbrook WP, Hjorleifsdottir DV. Occurrence of oral Candida albicans and other yeast-like fungi in edentulous patients in geriatric units in Iceland. Gerodontics. 1986;2(5):153-6. [Abstract]
- Rodu B, Carpenter JT, Jones MR. The pathogenesis and clinical significance of cytologically detectable oral Candida in acute leukemia. Cancer. 1988;62(9):2042-6. [Abstract | Full text]
- Dupont B, Graybill JR, Armstrong D, et al. Fungal infections in AIDS patients. J Med Vet Mycol. 1992;30(Suppl 1):19-28. [Abstract]
- Odds FC. Candida and Candidosis: A review and bibliography. London: Baillière Tindall; 1988. [Book]
- Oksala E. Factors predisposing to oral yeast infections. Acta Odontol Scand. 1990;48(1):71-4. [Abstract]
- Budtz-Jörgensen E. Etiology, pathogenesis, therapy, and prophylaxis of oral yeast infections. Acta Odontol Scand. 1990;48(1):61-9. [Abstract]
- Holt JM. Candida infection of the oesophagus. Gut. 1968;9(2):227-31. [Abstract | Full text]
- Kodsi BE, Wickremesinghe C, Kozinn PJ, et al. Candida esophagitis: A prospective study of 27 cases. Gastroenterology. 1976;71(5):715-9. [Abstract]
- Sehhat S, Hazeghi K, Bajoghli M, Touri S. Oesophageal moniliasis causing fistula formation and lung abscess. Thorax. 1976;31(3):361-4. [Abstract | Full text]
- Kaloyannides TM. Oral monoliasis in the newborn. J Can Dent Assoc (Tor). 1968;34(9):496-7. [Abstract]
- Fisher BM, Lamey PJ, Samaranayake LP, et al. Carriage of Candida species in the oral cavity in diabetic patients: Relationship to glycaemic control. J Oral Pathol. 1987;16(5):282-4. [Abstract]
- Manfredi M, McCullough MJ, Al-Karaawi ZM, et al. The isolation, identification and molecular analysis of Candida spp. isolated from the oral cavities of patients with diabetes mellitus. Oral Microbiol Immunol. 2002;17(3):181-5. [Abstract]
- Belazi M, Velegraki A, Fleva A, et al. Candidal overgrowth in diabetic patients: Potential predisposing factors. Mycoses. 2005;48(3):192-6. [Abstract]
- Rayfield EJ, Ault MJ, Keusch GT, et al. Infection and diabetes: The case for glucose control. Am J Med. 1982;72(3):439-50. [Abstract]
- Darwazeh AM, MacFarlane TW, McCuish A, Lamey PJ. Mixed salivary glucose levels and candidal carriage in patients with diabetes mellitus. J Oral Pathol Med. 1991;20(6):280-3. [Abstract]
- Clarkson JE, Worthington HV, Eden OB. Interventions for preventing oral candidiasis for patients with cancer receiving treatment. Cochrane Database Syst Rev. 2007;(1):CD003807. [Abstract | Full text]
- Glasmacher A, Cornely O, Ullmann AJ, et al. An open-label randomized trial comparing itraconazole oral solution with fluconazole oral solution for primary prophylaxis of fungal infections in patients with haematological malignancy and profound neutropenia. J Antimicrob Chemother. 2006;57(2):317-25. [Abstract | Full text]
- Chaushu G, Bercovici M, Dori S, et al. Salivary flow and its relation with oral symptoms in terminally ill patients. Cancer. 2000;88(5):984-7. [Abstract | Full text]
- Davies AN, Brailsford SR, Beighton D. Oral candidosis in patients with advanced cancer. Oral Oncol. 2006;42(7):698-702. [Abstract]
- Belazi M, Velegraki A, Koussidou-Eremondi T, et al. Oral Candida isolates in patients undergoing radiotherapy for head and neck cancer: Prevalence, azole susceptibility profiles and response to antifungal treatment. Oral Microbiol Immunol. 2004;19(6):347-51. [Abstract]
- De Pauw B. Practical modalities for prevention of fungal infections in cancer patients. Eur J Clin Microbiol Infect Dis. 1997;16(1):32-41. [Abstract | Full text]
- Leung KC, McMillan AS, Cheung BP, Leung WK. Sjögren’s syndrome sufferers have increased oral yeast levels despite regular dental care. Oral Dis. 2008;14(2):163-73. [Abstract]
- Figueiral MH, Azul A, Pinto E, et al. Denture-related stomatitis: Identification of aetiological and predisposing factors – a large cohort. J Oral Rehabil. 2007;34(6):448-55. [Abstract]
- Farah CS, Ashman RB, Challacombe SJ. Oral candidosis. Clin Dermatol. 2000;18(5):553-62. [Abstract]
- Palmer GD, Robinson PG, Challacombe SJ, et al. Aetiological factors for oral manifestations of HIV. Oral Dis. 1996;2(3):193-7. [Abstract]
- McCarthy GM, Mackie ID, Koval J, et al. Factors associated with increased frequency of HIV-related oral candidiasis. J Oral Pathol Med. 1991;20(7):332-6. [Abstract]
- Umadevi KMR, Ranganathan K, Pavithra S, et al. Oral lesions among persons with HIV disease with and without highly active antiretroviral therapy in southern India. J Oral Pathol Med. 2007;36(3):136-41. [Abstract]
- Sherman RG, Prusinski L, Ravenel MC, Joralmon RA. Oral candidosis. Quintessence Int. 2002;33(7):521-32. [Abstract]
- Clift RA. Candidiasis in the transplant patient. Am J Med. 1984;77(4D):34-8. [Abstract]
- Silverman S Jr, Luangjarmekorn L, Greenspan D. Occurrence of oral Candida in irradiated head and neck cancer patients. J Oral Med. 1984;39(4):194-6. [Abstract]
- Sivapathasundharam B, Gururaj N. Mycotic infections of the oral cavity: Candidiasis. In: Rajendran R, Sivapathasundharam B (eds). Shafer’s Textbook of Oral Pathology (6th edition). Delhi: Elsevier; 2009: 363-7. [Book]
- Akpan A, Morgan R. Oral candidiasis. Postgrad Med J. 2002;78(922):455-9. [Abstract | Full text]
- Fichtenbaum CJ, Aberg JA. Candidiasis and HIV [online]. San Francisco, CA: University of California San Francisco; February 2006 [cited 28 January 2011]. Available from: URL link
- Oral candidiasis and HIV disease: Preventing and treating fungal infections of the mouth and throat [online]. San Francisco, CA: Project Inform; November 2005 [cited 28 January 2011]. Available from: URL link
- Holmstrup P, Axéll T. Classification and clinical manifestations of oral yeast infections. Acta Odontol Scand. 1990;48(1):57-9. [Abstract]
- Reichart PA, Samaranayake LP, Philipsen HP. Pathology and clinical correlates in oral candidiasis and its variants: A review. Oral Dis. 2000;6(2):85-91. [Abstract]
- McCullough MJ, Savage NW. Oral candidosis and the therapeutic use of antifungal agents in dentistry. Aust Dent J. 2005;50(4 Suppl 2):S36-9. [Abstract | Full text]
- Soysa NS, Samaranayake LP, Ellepola AN. Antimicrobials as a contributory factor in oral candidosis: A brief overview. Oral Dis. 2008;14(2):138-43. [Abstract]
- Ellepola AN, Samaranayake LP. Inhalational and topical steroids, and oral candidosis: A mini review. Oral Dis. 2001;7(4):211-6. [Abstract]
- Ramirez-Amador V, Esquivel-Pedraza L, Sierra-Madero J, et al. Oral manifestations of HIV infection by gender and transmission category in Mexico City. J Oral Pathol Med. 1998;27(3):135-40. [Abstract]
- Ellepola AN, Samaranayake LP. Oral candidal infections and antimycotics. Crit Rev Oral Biol Med. 2000;11(2):172-98. [Abstract | Full text]
- Nelson BL, Thompson L. Median rhomboid glossitis. Ear Nose Throat J. 2007;86(10):600-1. [Abstract]
- Lombardi T, Budtz-Jörgensen E. Treatment of denture-induced stomatitis: A review. Eur J Prosthodont Restor Dent. 1993;2(1):17-22. [Abstract]
- Farah CS, Lynch N, McCullough MJ. Oral fungal infections: An update for the general practitioner. Aust Dent J. 2010;55(Suppl 1):48-54. [Abstract]
- Grimoud AM, Lodter JP, Marty N, et al. Improved oral hygiene and Candida species colonization level in geriatric patients. Oral Dis. 2005;11(3):163-9. [Abstract]
- Kulak-Ozkan Y, Kazazoglu E, Arikan A. Oral hygiene habits, denture cleanliness, presence of yeasts and stomatitis in elderly people. J Oral Rehabil. 2002;29(3):300-4. [Abstract]
- Liu X, Hua H. Oral manifestation of chronic mucocutaneous candidiasis: Seven case reports. J Oral Pathol Med. 2007;36(9):528-32. [Abstract]
- Williams DW, Lewis MA. Isolation and identification of Candida from the oral cavity. Oral Dis. 2000;6(1):3-11. [Abstract]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







