- What is Lymphoma of the Stomach (Gastric Lymphoma)
- Statistics on Lymphoma of the Stomach (Gastric Lymphoma)
- Risk Factors for Lymphoma of the Stomach (Gastric Lymphoma)
- Progression of Lymphoma of the Stomach (Gastric Lymphoma)
- Symptoms of Lymphoma of the Stomach (Gastric Lymphoma)
- Clinical Examination of Lymphoma of the Stomach (Gastric Lymphoma)
- How is Lymphoma of the Stomach (Gastric Lymphoma) Diagnosed?
- Prognosis of Lymphoma of the Stomach (Gastric Lymphoma)
- How is Lymphoma of the Stomach (Gastric Lymphoma) Treated?
- Lymphoma of the Stomach (Gastric Lymphoma) References
What is Lymphoma of the Stomach (Gastric Lymphoma)
Cancer is a condition in which the normal cells of the body undergo change and exhibit abnormal cell growth. This can manifest differently depending on the tissues/organs involved and the characteristics of the cancer itself.
Lymphoma is a cancer of the lymphatic cells/lymphoid tissue that forms part of the immune system. Normally these cells help protect our bodies against infection. The cells/tissues affected may be located within lymph nodes or in lymphoid tissue located in other sites of the body (not within lymph nodes) such as the central nervous system, gastrointestinal tract and skin. Approximately 25-50% of lymphomas occur in sites other than lymph nodes (extra-nodal sites).
For those lymphomas affecting the gastrointestinal tract, the stomach is the most commonly affected site (50-60%), followed by the small and large intestines (30% and 10% respectively).
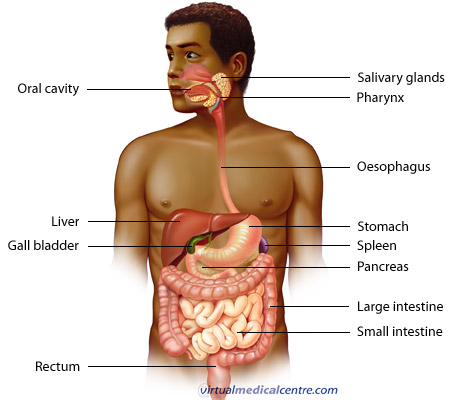
Approximately 5% of the cancers found in the stomach can be attributed to lymphomas. They are the second most common cancer affecting the stomach following adenocarcinoma.
Statistics on Lymphoma of the Stomach (Gastric Lymphoma)
The precise incidence of lymphomas in the gastrointestinal tract over the past twenty years is largely uncertain. There are large differences depending on the country in which you live (geographical) and between children and adults. Also there are many different forms of lymphoma and their prevalence varies depending on the location within the gastrointestinal tract.
In general most cases of gastric lymphoma occur in those aged 50 years or more (median 60-65 years) although cases occurring in the second decade of life have also been reported. The incidence of gastric lymphoma in individuals affected by HIV and/or AIDS is increasing and these individuals are becoming increasingly affected at younger ages.
Males are at a 2-3 times greater risk of developing gastric lymphoma.
Risk Factors for Lymphoma of the Stomach (Gastric Lymphoma)

- Age – Median age for diagnosis of gastric lymphoma is age 60-65 years;
- Sex – Males are affected 2-3 times more commonly than females;
- Chronic Helicobacter pylori infection – this is a bacteria that can grow and live within the gastrointestinal tract. Its presence has been associated with a number of pathologies including gastric ulcers and gastric lymphoma. However, given that H. pylori infects over 50% of the world’s population and the majority of these do not develop gastric lymphoma, other factors are believed to be involved.
- Other chronic infections – including hepatitis C, and human immunodeficiency virus (HIV);
- Autoimmune disorder of the thyroid or salivary glands;
- Coeliac disease.
Symptoms of Lymphoma of the Stomach (Gastric Lymphoma)
Early in the course of the disease individuals may not have symptoms at all, or otherwise the symptoms may be unspecific.
Common symptoms include:
- Upper abdominal pain;
- Upset stomach or indigestion;
- Change of bowel habits;
- Nausea and vomiting;
- Loss of appetite;
- Weight loss.
Vomiting of blood (haematemesis) or blood loss in the faeces (melena) occur at the outset in 20-30% of people.
You should seek medical attention if you develop any of these symptoms and/or you are concerned about your health.
Clinical Examination of Lymphoma of the Stomach (Gastric Lymphoma)
In patients affected by gastric lymphoma, a clinical examination performed by an experienced doctor is normal in 55-60% of cases.
It is for this reason that investigations, such as endoscopy (see below), are required if the diagnosis is suspected.
How is Lymphoma of the Stomach (Gastric Lymphoma) Diagnosed?
To diagnose gastric lymphoma and/or to differentiate it from other conditions which may present in a similar way such as gastritis or a gastric ulcer, several investigations will need to be performed including:
Blood tests
Blood tests will be used to determine your overall health and the levels of other markers that may be increased in infection or cancer.
Breath test
This is a simple non-invasive test in which your breath, following ingestion of urea, is used to determine the presence of H. pylori in the gastrointestinal system. This is often used as a first line test to determine your risk of H. pylori associated disease. It is important to assess the presence or absence of H. pylori as this may impact on treatment options available. The presence of H. pylori can be confirmed or excluded with the use of endoscopy and biopsy, which are important for an accurate diagnosis.
Endoscopy
Endoscopy involves feeding a small camera through the mouth and/or rectum to visualise the lumen (interior) of the gastrointestinal tract. This is used to look for the presence of normal or abnormal tissue. Abnormal findings may include changes to the lining of the stomach, the presence of a mass or other lesions, and/or an ulcer. Biopsies are generally taken as part of an endoscopic investigation and these play an important role in diagnosis of lymphoma.
Biopsy
A biopsy is a small sample of tissue taken for further investigation. If lymphoma or other gastrointestinal cancer is suspected a biopsy may be taken during endoscopy. The tissue sample obtained is then sent to the pathologist who can report on the submitted tissue.
Staging

- Computerised tomography (CT): CT is an imaging study in which X-rays are used to create a 3-dimensional image of the region of interest. In lymphoma a CT of the neck, chest, abdomen and pelvis may be performed to exclude spread to these regions of the body.
- Endoscopic ultrasound: Similar to endoscopy, this involves the use of a small ultrasound probe to visualise any abnormal areas previously identified on endoscopy. This provides useful information in terms of the depth of any lesions, and local spread.
- Positron emission tomography (PET): PET is an imaging study that highlights areas of activity within the body. As cancer cells are typically rapidly dividing, this can be used as part of the staging system to locate other areas of spread or alternatively to it can be used to monitor response to therapy.
- Bone marrow biopsy: Bone marrow biopsy involves removing a small sample of the bone marrow to determine if it has been involved in the disease process. While bone marrow involvement is rare with gastric lymphomas it occurs frequently in lymphomas occurring in other sites of the body.
- Spinal tap: If an individual with lymphoma has aggressive disease or symptoms suggesting that the central nervous system is involved, a sample of the fluid surrounding the spinal cord (spinal tap) may be taken for analysis.
From these investigations, the lymphoma is staged according to a staging system. The most appropriate staging system for gastric lymphoma is controversial. Several staging systems are available including the Lugano staging system for gastrointestinal lymphomas, The Ann Arbor stage, Tumour extension and a TNM staging system adapted for gastric lymphoma as described below. Each takes into account whether the cancer occurs solely in the gastrointestinal system, if it penetrates through the wall of the gastrointestinal tract, the involvement of lymph nodes and any spread to other sites within the body.
In the TNM staging system a score is given for each of the three areas of interest:
- Tumour (T) – the characteristics of the tumour
- Node (N) – the involvement of any lymph nodes
- Metastasis (M) – spread to distant sites in the body
The TNM staging system scores are given as outlined below. Involvement of the bone marrow (B) may also be included.
Paris staging system for primary gastrointestinal lymphomas
| Tx | Lymphoma extent not specified |
| T0 | No evidence of lymphoma |
| T1 | Lymphoma confined to the mucosa/submucosa |
| T1m | Lymphoma confined to the mucosa |
| T1sm | Lymphoma confined to the submucosa |
| T2 | Lymphoma has spread through the muscular layers |
| T3 | Lymphoma penetrates the outer surface of the gastrointestinal tract without invasion of adjacent structures |
| T4 | Lymphoma invades adjacent structures or organs |
| Nx | Involvement of lymph nodes not assessed |
| N0 | No evidence of lymph node involvement |
| N1c | Involvement of regional lymph nodes |
| N2 | Involvement of intra-abdominal lymph nodes beyond the regional area |
| N3 | Spread to extra-abdominal lymph nodes |
| Mx | Dissemination not assessed |
| M0 | No evidence of extranodal dissemination |
| M1 | Non-continuous involvement of separate sites in gastrointestinal tract (e.g. stomach and rectum) |
| M2 | Non-continuous involvement of other tissues (e.g. peritoneum, pleura) or organs (tonsils, parotid gland, ocular adnexa, lung, liver, spleen, kidney, breast, etc) |
| Bx | Involvement of bone marrow not assessed |
| B0 | No evidence of bone marrow involvement |
| B1 | Lymphomatous infiltration of the bone marrow |
Depending on the T, N, and M scores the tumour is then designated a stage:
| TNM stage I | T1 N0 M0 T2 N0 M0 T3 N0 M0 |
| TNM stage II | T1-3 N1 M0 T1-3 N2 M0 |
| TNM stage IIE | T4 N0 M0 |
| TNM stage IV | T1-4 N3 M0 T1-4 N0-3 M1 |
For example, if a tumour was confined to the inner layer of the gastrointestinal wall (T1) and there was no evidence of spread to lymph nodes (N0) or distant organs (M0), this would be a stage I tumour. In comparison, a tumour invading nearby structures (T4), and spread to lymph nodes located outside of the abdomen (N3) would be considered stage IV whether there was distant spread to other organs or not (M).
This information is important when considering suitable treatment options.
Prognosis of Lymphoma of the Stomach (Gastric Lymphoma)

- Low grade disease;
- Age <65;
- Clear surgical margins where resection has been performed; and
- Initial complete remission (following treatment of the primary cancer, there was no remaining evidence of cancer)
If you have H. pylori positive disease (you have tested positive for H. pylori and have a diagnosis of gastric lymphoma) certain chromosomal changes are associated with no response to treatment with antibiotics. These chromosomal changes can be tested for on tissue obtained from biopsy.
Five year survival rates are as high as 91% in low grade disease, but are reduced to 56% for high grade primary tumours.
How is Lymphoma of the Stomach (Gastric Lymphoma) Treated?

Treatment of gastric lymphoma has changed dramatically over the past two decades. We have seen a shift away from surgical techniques towards more conservative treatments such as chemotherapy and H. pylori eradication therapies.
Surgery
Historically, surgical techniques have been the primary treatment option for gastric lymphomas followed by the use of radiotherapy and/or chemotherapy. However in the late 1980s this began to be challenged and in practice today the role of surgery in the treatment of gastric lymphoma is limited.
The abandonment of surgery in the treatment of gastric lymphoma came from effective treatment with medical managements including chemotherapy and antibiotics. These conservative treatments offer a greater quality of life with no adverse impact on survival rates.
Antibiotic therapy
For gastric lymphomas associated with H. pylori infection, treatment is focused around H. pylori eradication using a combination of proton pump inhibitors and antibiotics. Between 60-100% of individuals achieve long term remission with this therapy.
In those individuals who respond to antibiotic therapy, there is no justification for additional treatment with chemotherapeutic agents. However, these individuals will need to be followed up as directed by their treating physician.
More information on H.pylori eradication
Chemotherapy
Chemotherapy refers to the use of drugs that are toxic to cells in an attempt to destroy cancer cells. Chemotherapy targets rapidly dividing cells, one of the main properties of cancer cells.
Treatment of early stage disease typically consists of:
- 3 cycles of chemotherapy with the drugs: cyclophosphamide, doxorubicin, vincristine and prednisolone (CHOP) +/-rituximab followed by radiotherapy; or alternatively
- 6-8 cycles of CHOP-rituximab.
Radiotherapy
The main role of radiotherapy for gastric lymphoma lies in the treatment of lymphoma confined to the gastrointestinal tract (no spread) that has failed to improve despite antibiotic eradication therapy or for those that are H. pylori negative. Radiotherapy can achieve 4-5 year disease free survival in 85-100% of people.
Side effects are largely dependant upon several factors including how big the target (cancer) is, the technique used, the total dose used and how this is delivered. Acute side effects typically include anorexia, nausea and vomiting, but these can usually be adequately prevented in the majority of cases with the use of drugs to prevent nausea and vomiting (anti-emetics). Diarrhoea and bone marrow suppression may also occur depending on the radiotherapy being performed.
Late side effects are expected to be minimal but may include kidney damage and secondary hypertension, or a slightly increased risk of second cancers.
Radiotherapy can also be used as an add-on therapy to chemotherapy in aggressive cases. However, two studies comparing chemotherapy and chemotherapy plus radiation in the treatment of aggressive gastric lymphoma have shown at least equal outcomes with the sole use of chemotherapy. This has led to speculation that we may be over treating some individuals with combined chemotherapy and radiotherapy.
Your doctor will advise on best treatment for you as this depends on several factors including whether you are H. pylori positive or negative, the form of lymphoma and how far advanced it is.
More information
 |
For more information on gastric cancer, including different types of gastric cancer, see Gastric Cancer. |
Lymphoma of the Stomach (Gastric Lymphoma) References
- Ferrucci PF, Zucca E. Primary gastric lymphoma pathogenesis and treatment: what has changed over the past 10 years? British Journal of Haematology 2006; 136: 521-38.
- Boot H. Diagnosis and staging in gastrointestinal lymphoma. Best Practice & Research Clinical Gastroenterolgy 2010; 24: 3-12.
- Ruskone-Fourmestraux A, Dragosics B, Morgner A, Wotherspoon A, De Jong D. Paris staging system for primary gastrointestinal lymphomas. Gut 2003; 52: 912-3.
- Montalban C, Santon A, Boixeda D, Bellas C. Regression of gastric high grade mucosa associated lymphoid tissue (MALT) lymphoma after Helicobacter pylori eradication. Gut 2001; 49: 584-7.
- Morgner A, Miehlke S, Fischbach W, Schmitt W, Muller-Hermelink H, Greiner A, Thiede C, Schetelig J, Neubauer A, Stolte M, Ehninger G, Bayerdorffer E Complete remission of primary high-grade B-cell gastric lymphoma after cure of Helicobacter pylori infection. Journal of Clinical Oncology 2001; 19: 2041- 8.
- Chen LT, Lin JT, Tai JJ, Chen GH, Yeh HZ, Yang SS, Wang HP, Kuo SH, Sheu BS, Jan CM, Wang WM, Wang TE, Wu CW, Chen CL, Su IJ, Whang-Peng J, Cheng AL. Long-term results of anti-Helicobacter pylori therapy in early-stage gastric high-grade transformed MALT lymphoma. Journal of the National Cancer Institute 2005; 97: 1345-53.
- Raderer M, de Boer J P. Role of chemotherapy in gastric MALT lymphoma, diffuse large B-cell lymphoma and other lymphomas. Best Practice & Research Clinical Gastroenterolgy 2010; 24: 19-26.
- Raderer M, Chott A, Drach J, Montalban C, Dragosics B, Jager U, et al. Chemotherapy for management of localised highgrade gastric B-cell lymphoma: how much is necessary? Ann Oncol 2002; 13: 1094-8.
- Aleman BMP, Haas RLM, van der Maazen RWM. Role of radiotherapy in the treatment of lymphomas of the gastrointestinal tract. Best Practice & Research Clinical Gastroenterolgy 2010; 24: 27-34.
- DeJong D, Boot H, van Heerde P, Hart GAM, Taal BG. Histological grading in gastric lymphoma: pretreatment criteria and clinical relevance. Gastroenterology 1997; 112: 1466-74.
- Jaffe ES, Harris NL, Stein H, Vardiman JW, eds (2001) World Health Organization Classification of Tumours. Pathology and Genetics of Tumours of Haematopoietic and Lymphoid Tissues. IARC Press, Lyon, France.
- Al-Akwaa AM, Siddiqui N, Al-Mofleh IA. Primary gastric lymphoma. World J Gastroenterol 2004; 10: 5-11.
- National Health & Medical Research Council. Clinical practice guidelines, Chapter 17, Gastric Lymphoma. Available from URL: http://nrv.gov.au/_files_nhmrc/file/publications/synopses/cp107/chapter17cp107.pdf [9th May 2010].
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







