- What is Irritable Bowel Syndrome (IBS)
- Statistics on Irritable Bowel Syndrome (IBS)
- Risk Factors for Irritable Bowel Syndrome (IBS)
- Progression of Irritable Bowel Syndrome (IBS)
- Symptoms of Irritable Bowel Syndrome (IBS)
- Clinical Examination of Irritable Bowel Syndrome (IBS)
- How is Irritable Bowel Syndrome (IBS) Diagnosed?
- Prognosis of Irritable Bowel Syndrome (IBS)
- How is Irritable Bowel Syndrome (IBS) Treated?
- Irritable Bowel Syndrome (IBS) References
What is Irritable Bowel Syndrome (IBS)
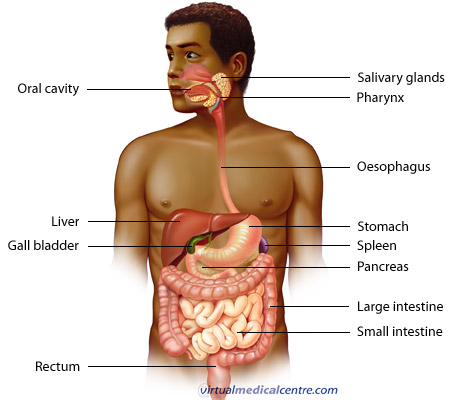
Irritable bowel syndrome or IBS is a chronic disorder of function of the gastrointestinal tract, particularly the large intestine (colon). The gastrointestinal tract (pictured below) consists of the mouth (oral cavity), oesophagus, stomach, pancreas, liver, gallbladder, and the small and large intestines.The colon, which is about 5 feet long, connects the small intestine with the rectum and anus. The major function of the colon is to absorb water, nutrients, and salts from the partially digested food that enters from the small intestine.
Statistics on Irritable Bowel Syndrome (IBS)
One in six to ten Americans has IBS, making it one of the most common disorders diagnosed by doctors. It occurs more often in women than in men, and it typically occurs between the ages of 20 and 40 years.
Risk Factors for Irritable Bowel Syndrome (IBS)
Symptoms of IBS cannot be traced to a single organic cause. Research suggests that people with IBS seem to have a colon that is more sensitive and reactive than usual to a variety of things, including certain foods and stress. Some evidence indicates that the immune system, which fights infection, is also involved.
IBS symptoms can result from the following:
- The normal motility of the colon may not work properly. It can be spasmodic or can even stop temporarily. Spasms are sudden strong muscle contractions that come and go;
- The lining of the colon (epithelium), which is affected by the immune and nervous systems, regulates the passage of fluids in and out of the colon. In IBS, the epithelium appears to work properly. However, fast movement of the colon’s contents can overcome the absorptive capacity of the colon. The result is too much fluid in the stool. In other patients, colonic movement is too slow, too much fluid is absorbed, and constipation develops;
- The colon responds strongly to stimuli (for example, foods or stress) that would not bother most people.
Progression of Irritable Bowel Syndrome (IBS)
The natural history of IBS is unclear, and generally consists of repeated episodes of intestinal symptoms, which makes initiation of treatment plans difficult.
Symptoms of Irritable Bowel Syndrome (IBS)
Irritable bowel syndrome affects each person differently.The hallmark of IBS is abdominal discomfort or pain, however, symptoms vary from person to person. The following symptoms are also common:
- Abdominal cramping and pain that are relieved after bowel movements;
- Alternating periods of diarrhoea and constipation;
- Change in the stool frequency or consistency;
- Gassiness (flatulence);
- Passing mucus from the rectum;
- Bloating;
- Abdominal distension.
Bleeding, fever, weight loss, and persistent severe pain are not symptoms of IBS and may indicate other problems such as inflammation, and a doctor should be consulted.
Clinical Examination of Irritable Bowel Syndrome (IBS)
If you think you have IBS, seeing your doctor is the first step. IBS is generally diagnosed on the basis of a complete medical history that includes a careful description of symptoms and a physical examination, focusing on the abdomen. Relevant investigations are then carried out to exclude any other causes.
These tests may include stool or blood tests, x-rays, or endoscopy (viewing the colon through a flexible tube inserted through the anus). If these tests are all negative, the doctor may diagnose IBS based on your symptoms: that is, how often you have had abdominal pain or discomfort during the past year, when the pain starts and stops in relation to bowel function, and how your bowel frequency and stool consistency are altered.
How is Irritable Bowel Syndrome (IBS) Diagnosed?
Clinical judgement is necessary to decide which investigations are necessary before an accurate diagnosis of IBS can be made. Because many of the symptoms are non specific, your doctor will decide after consultation whether there is a risk of more serious problems.
IBS is a diagnosis after exclusion of other conditions such as bowel cancer, inflammatory bowel disease, infections and food allergies. Therefore, your doctor may want to perform a number of diagnostic tests to exclude any other causes of your abdominal discomfort.
Prognosis of Irritable Bowel Syndrome (IBS)
Because irritable bowel syndrome is a chronic (long-term) disease, symptoms usually return from time to time. This may be influenced by factors such as stress, diet, or other environmental causes. No known treatment cures IBS. Multiple factors may play a role in aggravating IBS, so it may be difficult to predict which may make IBS worse for a particular person. Establishing a good relationship with a doctor may help alleviate concerns over symptoms and allow rapid recognition of changing or worsening symptoms.
How is Irritable Bowel Syndrome (IBS) Treated?
Treatment of IBS is comprehensive and based on individual symptoms. Treatment methods employed include dietary changes, medications and reduction of stressors.
Diet
Many people have already modified their diets before seeing a doctor. Temporarily avoiding dairy products may help assess whether symptoms of lactose intolerance are mimicking those of irritable bowel syndrome. Persons who avoid dairy products should exercise and consider taking calcium supplements. Certain foods, such as cruciferous vegetables (cauliflower, broccoli, cabbage, brussels sprouts) and legumes (beans) may worsen bloating and gassiness. Increasing fibre content may aid to relieve constipation.
Medications
Medications are an important part of relieving symptoms. Your doctor may suggest fibre supplements or occasional laxatives for constipation, as well as medicines to decrease diarrhoea, tranquilisers to calm you, or drugs that control colon muscle spasms to reduce abdominal pain. Antidepressants may also relieve some symptoms. It is also important to note that medications affect people differently and that no one medication or combination of medications will work for everyone with IBS. You need to work with your doctor to find the best combination of medicine, diet, counseling, and support to control your symptoms.
Irritable Bowel Syndrome (IBS) References
- Connell AM, Hilton C, Irvine G, et al. Variation of bowel habit in two population samples. Br Med J. 1965;2(5470):1095-9. [Abstract | Full text]
- Wald A. Treatment of irritable bowel syndrome [online]. Waltham, MA: UpToDate; 13 February 2005 [cited 2 June 2005]. Available from: URL link
- Drossman DA, Thompson WG. The irritable bowel syndrome: Review and a graduated multicomponent treatment approach. Ann Intern Med. 1992;116(12 Pt 1):1009-16. [Abstract]
- Hammer J, Talley NJ. Diagnostic criteria for the irritable bowel syndrome. Am J Med. 1999;107(5A):5-11S. [Abstract]
- Kumar P, Clark M (eds). Clinical Medicine (5th edition). Edinburgh: WB Saunders Company; 2002. [Book]
- Lehrer JK, Lichtenstein GR. Irritable bowel syndrome [online]. Omaha, NE: eMedicine; 2004 [cited 2 June 2005]. Available from: URL link
- Levy RL, Jones KR, Whitehead WE, et al. Irritable bowel syndrome in twins: Heredity and social learning both contribute to etiology. Gastroenterology. 2001;121(4):799-804. [Abstract]
- Lynn RB, Friedman LS. Irritable bowel syndrome. N Engl J Med. 1993;329(26):1940-5. [Abstract]
- Murtagh J. Murtagh’s General Practice (3rd edition). North Ryde, NSW: McGraw Hill Australia; 2001. [Book]
- Longmore M, Wilkinson I, Torok E. Oxford Handbook of Clinical Medicine (5th edition). Oxford: Oxford University Press; 2001. [Book]
- Talley NJ, Zinsmeister AR, Van Dyke C, Melton LJ 3rd. Epidemiology of colonic symptoms and the irritable bowel syndrome. Gastroenterology. 1991;101(4):927-34. [Abstract]
- Irritable bowel syndrome [online]. Bethesda, MD: National Digestive Diseases Information Clearinghouse; 2004 [cited 2 June 2005]. Available from: URL link
- Whorwell PJ, McCallum M, Creed FH, Roberts CT. Non-colonic features of irritable bowel syndrome. Gut. 1986;27(1):37-40. [Abstract | Full text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







