- What is Diabetes Mellitus Type 2?
- Statistics
- Risk Factors
- Progression
- Symptoms
- Clinical Examination
- How is it Diagnosed
- Prognosis
- Treatment
- References
What is Diabetes Mellitus Type 2?
Type 2 Diabetes Mellitus is a condition in which the body fails to metabolise glucose (sugar) correctly. This causes levels of sugar in the blood to increase, a state known as hyperglycaemia.
When a person does not have diabetes, a gland called the pancreas produces and secretes a hormone called insulin. The hormone is used by the body’s tissues to metabolise glucose. Usually the amount of insulin secreted increases in relation to the amount of carbohydrate (sugar) a person consumes. In people with type 2 diabetes, insulin secretion from the pancreas often decreases. This is referred to as reduced insulin secretion.
In addition the body tissues do not respond adequately to the insulin which is produced. Normally the insulin would be used by the body to draw glucose into the cells, where it could be stored as energy which could be used by the body later (e.g. when exercising or any of the other activities which involve energy expenditure). In type 2 diabetes, the glucose is not taken into the cells. This is referred to as insulin resistance. It causes glucose to stay in the blood stream and hyperglycaemia is the result.
Type 2 diabetes mellitus was previously called non-insulin dependent diabetes mellitus (NIDDM) and late onset diabetes mellitus. These names are no longer used because they are inaccurate. Insulin is often used in the management of type 2 diabetes. The condition is increasingly diagnosed in young people.
Statistics
Almost one in 20 Australians, or one million people, were diagnosed with type 2 diabetes mellitus in 2008. The actual proportion of Australians with the condition may be higher as many people are not diagnosed until they develop complications, for example diabetic retinopathy.
Of those who have been diagnosed with type 2 diabetes, 56% are men and 92% are over 45 years of age. The condition is most common in the Northern Territory where 7.7% of people have been diagnosed with diabetes and least common in the Australian Capital Territory where only 2.4% of people have been diagnosed.
It is by far the most common form of diabetes, accounting for 87% of all diabetes mellitus in Australia. Other types of diabetes include type 1 diabetes and gestational diabetes.
The proportion of Australians with type 2 diabetes has increased rapidly in the past decade. Estimates suggest that if the increase continues three million Australians will be living with diabetes by 2025.
Children
An increasing number of children and adolescents are being diagnosed with type 2 diabetes. Each year, 3 children in every 100,000 aged 10-14 years and 8 in every 100,000 aged 15-19 year are diagnosed with type 2 diabetes.
Risk Factors
Type 2 diabetes is partly a genetic disease and partly a lifestyle disease. People whose parents had diabetes have a genetic predisposition, meaning they are more likely to get type 2 diabetes themselves. However characteristics of a person’s lifestyle, especially what they eat and how much exercise they do, also influence the risk of type 2 diabetes. People with a genetic predisposition may not develop the condition if they lead a healthy lifestyle.
While there is no single cause for developing Type 2 diabetes, there are well-known risk factors. Some of these can be changed (avoidable) and some cannot (unavoidable).
Unavoidable risk factors
- Family history of diabetes – people with close relatives that have type 2 diabetes are more likely to get the condition themselves. One in ten of those with a sibling that has type 2 diabetes will develop the condition, as will half of those with an identical twin who is affected by type 2 diabetes.
- Age – the risk increases as a person gets older.
- Ethnic background – people from Aboriginal or Torres Strait Islanders, Pacific Islanders, Indian and Chinese ethnic background are more likely to develop type 2 diabetes mellitus.
- Having Polycystic Ovarian Syndrome or a history of gestational diabetes during pregnancy.
- Low birth weight is thought to predispose to diabetes due to poor beta-cell development and function.
Avoidable risk factors
- Obesity and overweight
- Physical inactivity
- High blood pressure
- Diet
- Impaired glucose metabolism
Progression
Type 2 diabetes mellitus may have an onset over several months, or be asymptomatic and be detected on a routine blood test. It is generally not recognised and diagnosed until the patient seeks health care for another problem.
Some common presenting symptoms of type 2 diabetes mellitus include:
- Excessive thirst.
- Increased urine output (polyuria).
- Hunger.
- Weight loss or gain.
- Slow healing or frequent infections.
- Blurred vision.
- Dry eyes
- Headaches.
- Numbness, tingling or burning of the feet (peripheral neuropathy).
Without treatment patients may develop acute complications due to dehydration (HONKC, see below) and long-term complications will develop much more rapidly.
The main acute complication is hyperosmolar nonketotic coma (HONKC), sometimes also known as hyperosmolar hyperglycaemic nonketotic coma (HHNC). This is a condition that develops over several days in poorly controlled diabetes involving high blood glucose and potentially lethal secondary dehydration and electrolyte disturbances.
Long-term complications include:
- Microvascular disease:
- Diabetic retinopathy (eye disease).
- Diabetic nephropathy (kidney disease).
- Peripheral neuropathy and autonomic neuropathy (nerve disease).
- Impotence (difficulty maintaining an erection).
- Macrovascular disease – i.e. atherosclerosis (hardening of the arteries) causing:
- Coronary artery disease or heart attack.
- Cerebrovascular disease (stroke).
- Peripheral vascular disease – potentially causing gangrene and leading to need for leg or toe amputation.
Men are particularly susceptible to diabetic complications and often have higher rates of mortality than females.
Symptoms
Diabetes can be easily diagnosed if you present with the classic symptoms of:
- Thirst.
- Polyuria- Passing urine often or waking at night several times to pass urine (nocturia).
- Fatigue.
- Hunger.
- Weight loss.
However, many patients with diabetes remain assymptomatic for many years but are still subject to the damaging effects of high blood sugars. Unlike type 1 diabetes which tends to present acutely, type 2 diabetes presents gradually over several years.
At the time of diagnosis of type 2 diabetes, you may already have several complications of the disease, such as heart or eye problems. You may have noticed blurring of your vision, pins and needles in the feet (due to damage to the nerves) and recurrent infections.
Diabetes or impaired glucose tolerance may be detected on routine blood tests as part of a general health check-up or investigation for other symptoms or diseases. If you are obese, suffer from high blood pressure, have a family history of diabetes, have high cholesterol or come from a high risk population (e.g. Aboriginal background) it is important that you get tested for diabetes.
Clinical Examination
Your doctor will perform a careful examination mainly looking for the various complications of diabetes. This will include cardiovascular, neurological and retinal (eye) examinations. In the early stages of disease your examination may be completely normal, however as the duration and severity of disease progressed it is likely you will have some end-organ damage.
Your doctor will use a special device (called an opthalmoscope) to look at the back of your eye (retina). Here the doctor may see various degrees of diabetic retinopathy which basically represents damage to and leaking from the small vessels at the back of your eyes. Often cataracts (white opacities) may also be found in the lens. These develop because the excess sugar upsets the normal consistency of the lens. You may also have dry eyes.
Cardiovascular exam may reveal signs of heart failure due to ischaemic heart disease. You may have an abnormal heart rhythm or crackles at the base of your lungs from accumulated fluid. In addition, your blood pressure will be checked and your doctor may perform an ECG to detect any obvious ischaemic changes.
Leg examination may reveal diabetic ulcers (on pressure points in the feet) and peripheral vascular disease (poor peripheral pulses and circualtion), diabetic foot disease and trophic skin changes and skin infections. Your doctor will also test the nerves in your legs. You may have the classic ‘glove and stocking’ neuropathy which refers to reduced sensation in the distal portions of your limbs (i.e. where gloves and stockings are usually positioned). The neuropathy starts distally and progresses further up the limb as the condition worsens.
Your sensations of vibration (tested with a tuning fork placed on the bone) and propioception (recognition of joint space position, tested by wiggling your toe or finger with your eyes closed) tend to be affected first. In advanced cases you may have severe pain and impaired motor function.
Finally your doctor may request a urine sample to measure the amount of protein present. This reflects your kidney function as damaged kidneys tend to leak protein.
How is it Diagnosed
Type 2 diabetes mellitus is diagnosed when any of the following criteria are reached:
- Symptoms of diabetes are present (increased urination, increased thirst or weight loss) with a random plasma glucose (RPG) level of >11.0mmol/L
- Fasting plasma glucose (FPG) >7.0mmol/L
- Oral glucose tolerance test (OGTT) 2 hour plasma glucose >11.1mmol/L
Patients who do not reach these criteria may still be classified as having impaired fasting glucose (IFG) or impaired glucose tolerance (IGT) on the basis of fasting blood glucose or oral glucose tolerance test results. These patients are at increased risk of developing type 2 diabetes mellitus.
Other tests which may be ordered include:
- Glycosylated haemoglobin (HbA1c): this test is not used as a diagnostic or screening test for diabetes but may be used in the ongoing monitoring of diabetes. HbA1c reflects blood glucose levels over the past 2-3 months. Results >7% suggest poor blood glucose control and correlate with poor clinical outcomes.
When a diagnosis of diabetes mellitus is first made, several tests are often ordered to check for organ function and exclude complications of diabetes. These may include:
- Full blood count.
- Urea and electrolytes (potentially showing kidney impairment).
- Urinalysis to check for infection or protein loss through the kidneys.
- Liver function tests.
- Chest x-ray.
- ECG.
- Blood lipids (including cholesterol).
Prognosis
Diabetes is associated with a significant long-term risk of early mortality and morbidity. Heart disease (heart attacks 3-5 times more likely), peripheral vascular disease (amputation 50 times more likely), and stroke (twice as likely) are the major causes of death in patients over the age of 50. In addition, diabetic eye disease and renal failure due to diabetic nephropathy are important causes of morbidity. In addition, renal failure is potentially fatal. However, several large trials have proven that the risks of long-term complications from diabetes can be reduced with good blood glucose (sugar) control.
The acute complication of hyperosmolar non-ketotic coma has a mortality approaching 50% due to the fact that it affects elderly patients with extensive medical problems. Hypoglycaemia due to inappropriate use of insulin or as a side-effect of medications is also potentially fatal.
Treatment
The first goals of treatment are to eliminate symptoms of hyperglycemia (high blood sugar), stabilise blood glucose, and restore normal body weight. The ongoing goals of treatment are to prevent or reduce long-term complications, and to allow the patient to live as normal a life as possible.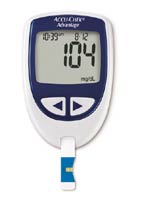
A team approach is usually used in the management of diabetes mellitus. Team members may include a GP, diabetic specialist, diabetic educator, ophthalmologist, podiatrist, dietician and the patient themselves. These health professionals can help to monitor all aspects of the disease. Diabetic educators in particular are invaluable, providing you with information about nutrition, exercise, the management of diabetes during illness, and medication. They may also teach you skills such as home monitoring of blood sugar levels (BSLs).
BSL monitoring is now a simple and quick task, which can be accomplished by the use of a blood sugar monitor (pictured right). BSL monitors assess levels by analysing a drop of blood that has usually been obtained by a very quick finger prick and take only moment to give a result.
Monitoring of glucose control and regular follow-up is extremely important. Tests include glycosylated Hb (also known as HbA1c, a reflection of long-term blood glucose control), blood pressure, weight, plasma lipids, proteinuria (protein in the urine), kidney function, condition of feet and cardiovascular exam.
Regular education and counselling is also extremely important.
Lifestyle changes
Diet and exercise are key in the management of type 2 diabetes. In fact, most patients will notice an improvement in symptoms after just one month of lifestyle changes. Dietary changes focus on the ideas of weight loss and blood sugar regulation (that is, keeping the blood sugar levels relatively stable throughout the day, avoiding big peaks or troughs).
Some simple ideas include:
- Eat healthy food, regularly spaced throughout the day – don’t skip meals;
- Reduce the amount of fat in your diet;
- Avoid refined carbohydrates and sugars, replacing them with complex carbohydrates (such as wholemeal bread);
- Eat plenty of fruit and vegetables; and
- Reduce or eliminating alcohol from the diet.
It is recommended that you consume foods that have a low Glycaemic Index (GI) as these raise your blood sugar by much lower amounts.
Exercise is also extremely important in managing diabetes. 30 minutes of moderate activity on most days of the week is recommended. If you are not used to exercise, always take care when beginning a new exercise program, and see your health professional before you begin.
If you are significantly overweight or obese you may require additional treatments to help you lose weight. A variety of obesity treatments are now available including meal replacement programs, lifestyle changes, weight loss drugs and surgery (for the morbidly obese). You should discuss with your doctor whether any of these treatments are suitable for you.
Medications
If lifestyle modifications are inadequate to control diabetes, tablets are usually the next step. Metformin is usually the first line agent if you are overweight as it does not have the side effect of weight gain. Sulfonylureas (e.g. glibenclamide and gliclazide) are the tablets of choice in thin patients. Care must be taken in the latter case to avoid hypoglycaemia (low blood sugar).
You should be aware of warning signs of a hypoglycaemic attack including weakness, pallor, hunger, sweating, shaking, confusion, loss of concentration and blurred vision, and carry suitable sugar remedies. Metformin can have a serious side effect called lactic acidosis if you have impaired renal, liver or cardiac function. Your doctor will decide whether this medication is suitable for you and explain situations where metformin treatment may be dangerous.
Another oral hypoglycaemic agent is often added later on. Acarbose and newer drugs (rosiglitazone and pioglitazone) can also be used. Insulin may eventually be needed in poorly controlled diabetes, or when other treatments fail.
References
- Braunwald, Fauci, Kasper, Hauser, Longo, Jameson. Harrison’s Principles of Internal Medicine. 16th Edition. McGraw-Hill. 2005
- Cotran, Kumar, Collins 6th edition. Robbins Pathologic Basis of Disease. WB Saunders Company. 1999.
- Dunstan, Zimmet, Welborn, Sicree, Armstrong, Atkins, Cameron, Shaw, Chadban on behalf of the AusDiab Steering Committee, Diabesity & Associated Disorders in Australia- 2000. The Accelerating Epidemic, International Diabetes Institute, 2001.
- Hurst JW (Editor-in-chief). Medicine for the practicing physician. 4th edition Appleton and Lange 1996.
- Isley W, Oki J. ‘Diabetes Mellitus, Type 2.’ eMedicine, Web MD, 2006. Available at: [URL Link] (Last accessed 12/12/06).
- Kumar P, Clark M. Clinical Medicine. WB Saunders 2002 Pg 427-430.
- Longmore M, Wilkinson I, Torok E. Oxford Handbook of Clinical Medicine. Oxford University Press. 2001.
- Murtagh J. General Practice. 3rd edition. McGraw-Hill. 2003.
- Talley NJ, O’Connor S. Examination medicine. 5th edition. Churchill Livingstone. 2006.
- Coyne KS, Margolis MK, Kennedy-Martin T, et al. The impact of diabetic retinopathy: perspectives from patient focus-groups. 2004. Fam Prac; 21(4): 447-53. Available from: [Abstract]
- Watkins PJ. Retinopathy. BMJ. 2003; 326: 924-6. Available from: [Full Text]
- International Council of Ophthalmology. Diabetic Retinopathy (Initial and Follow up evaluation). 2010. Available from: [URL Link]
- American Diabetes Association. Physical Activity/Exercise and Diabetes. Diabetes Care. 2004; 27(s1): s58-s62. Available from: [Full Text]
- Huang ES, Brown SES, Ewigman BG, Patients perceptions of Quality of life with diabetes related complications and treatments. Diabetes care. 2007; 30(10): 2478-2483. Available from: [Abstract | Full Text]
- Diabetes Australia. Diabetes: the silent pandemic and its impact on Australia. 2012. [cited 30 April 2015. Available from: [URL Link]
- Australian Institute of Health and Welfare. What is Diabetes? Undated. [cited 30 April 2015]. Available from: [URL Link]
- Australian Institute of Health and Welfare. Diabetes prevalence in Australia: detailed estimates for 2007-08. 2011. [cited 30 April 2015]. Available from: [URL Link]
- Australian Institute of Health and Welfare. Type 2 diabetes in Australia’s children and young people: a working paper. 2014. [cited 30 April 2015] Available from: [URL Link]
- International Diabetes Federation. Diabetes risk factors. 2014. [cited 30 April 2014] Available from: [URL Link]
- National Health and Medical Research Council. Diabetes. Genetics in Family Medicine- The Australian Handbook for General Practitioners. 2007. [cited 30 April 2015]. Available from: [URL Link]
- Diabetes Australia. Type 2 Diabetes. 2013. [cited 30 April 2014]. Available from: [URL Link]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







