- What is Deep Vein Thrombosis (DVT)
- Statistics on Deep Vein Thrombosis (DVT)
- Risk Factors for Deep Vein Thrombosis (DVT)
- Progression of Deep Vein Thrombosis (DVT)
- Symptoms of Deep Vein Thrombosis (DVT)
- Clinical Examination of Deep Vein Thrombosis (DVT)
- How is Deep Vein Thrombosis (DVT) Diagnosed?
- Prognosis of Deep Vein Thrombosis (DVT)
- How is Deep Vein Thrombosis (DVT) Treated?
- Deep Vein Thrombosis (DVT) References
What is Deep Vein Thrombosis (DVT)
Deep Vein Thrombosis is the formation of a blood clot in one of the deep veins of the body. DVT clots usually occur in those deep veins within the leg, particularly within the calf muscles. The veins in the arm, eye or brain may also rarely be affected. Deep vein thrombosis is quite rare, affecting approximately one or two people in every thousand, mainly older people.
Statistics on Deep Vein Thrombosis (DVT)
The true incidence of deep vein thrombosis is not entirely known as many studies have not been accurate nor conclusive to date. However, overall it is thought approximately 80 cases of deep vein thrombosis occur per 100,000 persons occur annually. The incidence of deep vein thrombosis in the hospitals is much higher, especially in surgical patients. This is thought to be related to long periods of immobilisation which encourage the blood the clot.
Risk Factors for Deep Vein Thrombosis (DVT)
Unlike arterial emboli, DVTs often occur in structurally normal vessels. They frequently develop due to stasis of blood (for example cardiac failure) or hypercoaguable states.4 Previous history of venous thromboembolic disease is a key risk factor for DVT. Other important risk factors are listed below:
- Increasing age.
- Family history.
- Drugs- Synthetic oestrogens in the oral contraceptive pill, Tamoxifen or hormone replacement therapy increase patient’s risks of DVT.
- Pregnancy and the puerperium.
- Recent surgery or trauma- Pelvic and orthopaedic surgeries (e.g. hip) are particularly high risk.5
- Clotting disorders– Thrombophilia, Protein C or S deficiency, Anti-thrombin deficiency and Antiphospholipid syndromes have all been associated with increased rates of DVT.4
- Malignancy.
- Obesity.
- Smoking.
- Varicose veins.
- Periods of immobility- This includes long air travel.6 Reduced physical activity reduces the muscular mechanisms that aid venous return to the heart.
The single most important risk factor for deep vein thrombosis is a prior history of DVT or pulmonary embolism (PE). However, if any of your first-degree relatives (parents or siblings) has had a clot, you are also at higher risk. The reason for this is that an inherited blood factor imbalance that causes increased susceptibility to clotting. Deep vein thrombosis post-surgery patients continue to be at risk for several months after surgery, as do women after delivery of their baby. One study also found that people with varicose veins and older people were at greater risk of deep vein thrombosis. The more risk factors you have, the greater your chances of clotting.
Additional risk factors:
- Recent surgery.
- Smoking.
- A malignancy.
- Taking synthetic hormone replacement therapy or oral contraceptives.
- Being obese or pregnant.
Progression of Deep Vein Thrombosis (DVT)
Deep vein thrombi usually develop when there is a reduction in the amount of blood flow (called stasis) or there is an increased clotting tendency (either inherited or acquired). The thrombi can grow by clumping more red blood cells and fibrin together. Occasionally the thrombus can obstruct the vessel involved or parts can break off ans spread to the rest of the vasculature.
Symptoms of Deep Vein Thrombosis (DVT)
DVT often presents as a painful or aching calf. You may also notice some redness, swelling or warmth over the area. These deep vein thrombosis symptoms are serious so you should always obtain medical advice as dislodgement of a clot to elsewhere in the body can be life-threatening. Your doctor will ask you several questions about the pain and possible risk factors for DVT such as travel, surgery and drug use.
Clinical Examination of Deep Vein Thrombosis (DVT)
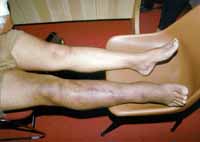
- Leg pain in one leg only- Felt as an ache or tightness in the calf.
- Leg tenderness in one leg only.
- Acute diffuse swelling (oedema) of only one leg.
- Changes in skin color of one leg, eg. redness.
- Increase in the warmth of one leg.
- Mild fever.
- Increased pain or resistance on dorsiflexion of the foot (Homan’s sign)- This is not a reliable sign and generally should not be performed due to risks of dislodging the thrombus.5,6
Your doctor will carefully examine your leg looking for:
- Tenderness or pain within the calf.
- Swelling of the limb.
- Redness.
- Warmth.
They may check if bending your foot up is painful (a sign of DVT) but there are risks of dislodging the clot associated with this manoeuvre.
How is Deep Vein Thrombosis (DVT) Diagnosed?
Investigations for deep vein thrombosis inculde:
- Blood tests– A particular test called a D-Dimer is performed which measures a breakdown product of clots. If this test is negative it can rule out DVT. However, a positive test result is not always reliable because other things like infection, pregnancy and cancers can also cause it to rise. Therefore if the test is positive more specific investigations are needed such as:
- Venography– This is probably the most reliable test for detecting clots in the veins. For this procedure a radiologist will inject contrast material into a vein on the top of the foot. This spreads through the veins and shows up on an x-ray. The clot area will be seen as a defect in the contrast. The venography is reasonably accurate, but it is also a costly and painful procedure. Moreover, the irritation of the vein by the contrast material may in itself contribute to the formation of new clots.
- Ultrasonography is a less invasive test that is also quite reliable detecting clots. Ultrasound works by emitting sound waves that can determine the flow of blood within the vessels. The clogged veins are easily distinguished on color pictures produced by this method. This method is painless, no foreign material is injected, and no radiation is required. The method is also cheaper than venography, but it is less accurate at detecting thrombi in smaller veins within the calf.
- CT or Magnetic Resonance Imaging may also occasionally be used.
The doctor may do additional tests to determine if you have a clotting disorder. This involves a series of blood tests looking for abnormal levels of some proteins in the blood. This is particularly important for patients with recurrent deep vein thrombosis family history of DVT or cases where there is no obvious cause (such as recent surgery or immobilisation) for the clot forming.
Prognosis of Deep Vein Thrombosis (DVT)
The majority of deep vein thrombosis will disappear without any complications, however there is a significant risk for recurrence. Pulmonary embolus is uncommon when deep vein thrombosis are treated properly but they can occur and can be life threatening.
Complications:
- If left untreated, deep vein thrombosis can cause a lot of pain and discomfort.
- DVT can also lead to varicose veins and certain other irreversible changes in the skin and the tissue.
- If the thrombus gets detached from the site it can lead to pulmonary embolism.
- Deep vein thrombosis can lead to non-healing venous ulcers.
How is Deep Vein Thrombosis (DVT) Treated?
Treatment of deep vein thrombosis largely aims to prevent the development of a pulmonary embolus (a clot in the lung) as this can be a life-threatening condition. To do this doctors will aim to reduce the size of the clot using anticoagulant (blood thinning) medications.
The first main deep vein thrombosis treatment is called heparin which can be given through a vein in the arm. This results in almost immediate anticoagulation and treatment of the clot. For this treatment you need to stay in hospital so your APTT can be measured in the blood. This basically is a measure for how well your blood clots which indicates if the drug is working or not.
Heparin is also available as an injection under the skin and this can be given on an out-patient basis. This type of heparin is called low-molecular- weight heparin (such as enoxaparin) and has the advantage of more predictable actions. A standard dose can be given based on your weight and monitoring is not needed.
Along with heparin an oral medication called warfarin is given. Because warfarin usually takes several days to reach effectiveness (until it reaches a therapeutic level), the heparin is continued until the warfarin is able to be effective. The effect of warfarin is also monitored using another blood test called the INR. When this reaches approximately 2.5 for two days in a row, the heparin can be stopped. Heparin needs to be given for at least five days. Warfarin is continued for around 3-6 months to prevent further clot formation. INR needs to be continually monitored because there is a risk of bleeding when the dose gets too high.
Other treatments for DVT included pressure stockings and early mobilisation. These help prevent pooling of blood within the legs. In some patients who have pulmonary emboli or that can’t take anticoagulant medications, a filter may be need to be inserted into the inferior vena cava. This is the main vein returning blood from the lower part of the body to the heart and lungs. The filter traps blood clots before they can enter the lungs. All patients who are at risk for DVT (e.g. pregnant, elderly, clotting disorder) will require special preventative methods during hospital visits or surgery. This includes wearing the pressure stockings, physiotherapy, early ambulation and calf compressors during surgery. Around the time of surgery patients will also be given regular heparin to prevent clot formation.
Deep Vein Thrombosis (DVT) References
- Anderson DR. Wells PS. Stiell I. MacLeod B. Simms M. Gray L. Robinson KS. Bormanis J. Mitchell M. Lewandowski B. Flowerdew G. Management of patients with suspected deep vein thrombosis in the emergency department: combining use of a clinical diagnosis model with D-dimer testing. Journal of Emergency Medicine 2000; 19(3):225-30.
- Gallus A, Baker R, Chong B, Ockelford P, Street A. on behalf of the Australasian Society of Thrombosis and Haemostasis. Consensus guidelines for warfarin therapy. MJA 2000; 172: 600-605.
- Hirsh J. Warkentin TE. Shaughnessy SG. Anand SS. Halperin JL. Raschke R. Granger C. Ohman EM. Dalen JE. Heparin and low-molecular-weight heparin: mechanisms of action, pharmacokinetics, dosing, monitoring, efficacy, and safety. Chest 2001; 119: 64S-94S.
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
- Murtagh J. General Practice. 3rd Edition. McGraw-Hill Australia. 2003.
- Tovey C, Wyatt S. Diagnosis, investigation, and management of deep vein thrombosis. BMJ 2003; 326: 1180-1184.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







