- What is Chronic Bronchitis
- Statistics on Chronic Bronchitis
- Risk Factors for Chronic Bronchitis
- Progression of Chronic Bronchitis
- Symptoms of Chronic Bronchitis
- Clinical Examination of Chronic Bronchitis
- How is Chronic Bronchitis Diagnosed?
- Prognosis of Chronic Bronchitis
- How is Chronic Bronchitis Treated?
- Chronic Bronchitis References
What is Chronic Bronchitis
Chronic bronchitis is a disease of the lung. The lungs consist of a series of folded membranes (the alveoli) which are located at the ends of very fine branching air passages (bronchioles).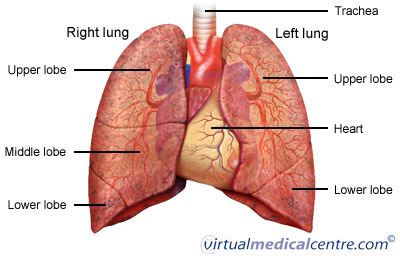
Chronic bronchitis is a persisting infection and inflammation of the larger airways of the lungs – the bronchi. There are two main bronchi in the lungs (the right and left) which divide from the trachea, as seen in the figure to the right. Chronic bronchitis occurs as part of the disease complex known as chronic obstructive pulmonary disease (COPD) which also includes emphysema and small airways disease. Chronic bronchitis specifically refers to chronic cough and daily mucus production for at least three months of two or more consecutive years. Other causes of chronic cough must be excluded before making the diagnosis.
Statistics on Chronic Bronchitis
COPD (which includes chronic bronchitis and emphysema) is a common disease in Australia and a major cause of disability, hospital admissions, and mortality. It is considered to be ranked third in the overall burden of disease after heart disease and stroke. More than half a million Australians are estimated to suffer from moderate to severe disease, and COPD ranks fourth among the common causes of death in Australian men, and sixth in women. Rates are even significantly higher in the Australian Aboriginal population.
Chronic bronchitis is common among smokers. In Western countries it is estimated that chronic bronchitis occurs in approximately 18% of male and 14% of female smokers compared to 7% and 6% of non-smokers, respectively.
Risk Factors for Chronic Bronchitis
Chronic bronchitis can affect both males and females of all ages but it tends to be most common in middle-aged males. The following predisposing factors have been identified:
- Cigarette smoke– This is by far the most important factor in the development of chronic bronchitis. The disease is 4 to 10 times more common in heavy smokers regardless of age, sex, occupation, and place of dwelling. There is a direct relationship between intensity of smoking and reductions in lung function and mortality from disease. Those who smoke 30 cigarettes per day are 20 times more likely to die from chronic bronchitis and COPD than non-smokers.
- Pollution- Non-smokers exposed to heavy atmospheric pollution may occasionally develop chronic bronchitis. This results due to irritation of the airways from inhalation of toxins and fumes.
- Family history- There is some role of family history in the development of COPD and chronic bronchitis.
- Airway infections- Although infection is not considered responsible for the initiation of chronic bronchitis, it is important factor in maintaining disease and causing exacerbations.
Progression of Chronic Bronchitis
Early on in chronic bronchitis you usually will have symptoms of cough productive of significant amounts of sputum without any significant breathlessness. The excess mucus production is caused by enlargement of mucous glands and increased numbers of mucus-secreting goblet cells in the airways. The small airways themselves then become inflamed but at this stage the disease is considered largely reversible. Cessation of smoking will resolve the airway inflammation.
As the disease progresses there is progressive abnormal cell growth (called squamous metaplasia) and fibrosis (hardening) of the bronchial walls. This causes airflow limitation and symptoms of shortness of breath. Symptoms of breathlessness are usually present on exertion. You may develop other signs of COPD such as cyanosis (bluish discolouration of the lips and skin). Emphysema may also be present at this stage, causing more severe shortness of breath and chest tightness.
If your chronic bronchitis remains severe some other complications can develop including:
- Secondary polycythaemia– This is an increase in the number of red blood cells in the blood to try to compensate for reduced oxygen levels. The blood subsequently becomes ‘thicker’ with sluggish flow which can lead to clotting.
- Right heart failure.
- Pneumothorax (punctured lung).
- Respiratory failure– This is often caused by acute infective exacerbations. Death can sometimes occur from severe declines in respiratory function.
Symptoms of Chronic Bronchitis
Chronic bronchitis is defined clinically as cough productive of sputum for at least 3 months a year over 2 consecutive years. If airway limitation is also present you may experience symptoms of wheezing, chest tightness and breathlessness. Your doctor will ask you lots of questions about your symptoms including when they started, their duration and any triggering factors.
Symptoms may be worsened by factors such as cold, foggy weather and atmospheric pollution. In addition your doctor will take a detailed medical history and family history to exclude other causes of cough and sputum production. Smoking history is essential as this is the major cause of chronic bronchitis.
It can be difficult to distinguish symptoms of chronic bronchitis from emphysema and both conditions commonly occur together. Therefore if you have cough and breathlessness your doctor may diagnose COPD, rather than chronic bronchitis alone.
Clinical Examination of Chronic Bronchitis
Your doctor will perform a detailed examination of your respiratory system. This will include undressing your top, inspecting your chest, measuring your chest expansion and listening to your breath sounds. Important signs your doctor will be looking for include:
- Productive cough.
- Cyanosis (bluish discolouration).
- Tachypnoea- An increased respiratory rate.
- Use of accessory muscles.
- Hyper-expansion of the chest- In advanced disease the chest wall can become barrel shaped.
- Reduced chest expansion.
- Reduced breath sounds, wheeze and crackles.
- Signs of heart failure such as peripheral oedema (swelling) may be present in advanced disease.
Patients with chronic bronchitis are classically described as “blue bloaters” due to the presence of cyanosis and oedema. They have reduced levels of ventilation and are not very breathless. There are low levels of oxygen in the blood and high levels of carbon dioxide which can cause other signs such as bounding pulse, asterixis (flapping of the hands), and in severe cases, confusion and progressive drowsiness.
Patients with predominantly emphysema on the other hand are described as “pink puffers” as they are very breathless and hyperventilating (with pursed lips) but have near normal levels of oxygen and carbon dioxide in the blood. However, these clinical signs aren’t always reliable and do not always correlate with pathology.
How is Chronic Bronchitis Diagnosed?
Your doctor may perform number of tests to confirm the diagnosis of chronic bronchitis and to detect the associated airway limitation. Tests may include:
- Blood tests- Specifically looking at the concentration of red blood cells which may be increased due to the chronic lack of oxygen in the body.
- Chest x-ray– This helps to show hyper-expansion of the lungs associated with chronic bronchitis and COPD. The lung fields will look enlarged and empty and may flatted out the diaphragm.
- ECG– This can detect signs of right heart failure (a complication of chronic bronchitis and COPD).
- Pulmonary/Lung Function tests– Spirometry is the best test to detect airflow limitation and obstruction. Unlike asthma, the airflow limitation is not reversible.
- Blood gases- These may also be normal but in the later stages of disease you may have low oxygen and high carbon dioxide levels.
- High resolution CT– This is sometimes used in patients with COPD. It is best for detecting emphysema and bullae (big dilated air spaces).
Prognosis of Chronic Bronchitis
Chronic bronchitis itself does not cause an increase in mortality unless there is an associated decline in lung function. Your overall prognosis therefore depends on:
- Whether you continue to smoke- Stopping smoking will improve symptoms in 90% of patients. Even if you have severe disease, studies have shown that stopping smoking increases survival.
- Your current lung function.
- Presence of other complications such as heart failure and respiratory failure.
- Frequency of exacerbations.
Chronic bronchitis with severe breathlessness carries a poor prognosis with approximately 50% of patients dying by 5 years. Death is usually caused by a decline in lung function from infective exacerbations.
How is Chronic Bronchitis Treated?
Chronic bronchitis should be treated if airway limitation is present. Treatment follows the same general principals as treatment of COPD. The majority of treatments only control and improve symptoms.
Only smoking cessation and oxygen therapy (in those with advanced disease) actually alter the course of disease. Stopping smoking is the best thing you can do as quitting smoking, regardless of the stage and severity of disease, will slow down the rate of progression and prolong life. Other treatments are outlined below.
Drug therapy
Drugs can be used for long-term suppression of symptoms or for treatment of acute exacerbations. Bronchodilators (such as Ventolin, Seretide and Atrovent via puffer or nebuliser) and corticosteroids are used for symptom control. Your doctor will usually give you a trial of oral steroids to see if you respond before using long-term inhaled steroids. Antibiotics are taken for short-term exacerbations of disease. Your doctor may also prescribe agents to reduce the thickness of your sputum (called mucolytics, for example acetylcysteine). Studies have shown these agents may reduce the frequency of exacerbations.
Pulmonary rehabilitation
Chest physiotherapy has been shown to help remove secretions in the airways. Various techniques are available which assist sputum removal and improve your ventilation for patients. Your doctor will also enter you into exercise or pulmonary rehabilitation programs which have been shown to increase exercise tolerance, relieve symptoms and improve quality of life.
Oxygen therapy
If you have severe airflow limitation you may require home oxygen therapy, sometimes for up to 19 hours per day. Oxygen ca be administered via nasal prongs or mask. This treatment has been shown to prolong life in patients with severe COPD who have stopped smoking.
Other
- Vaccinations- It is important that you have your yearly influenza vaccination, and pneumococcal vaccine. This will help reduce effective exacerbations from these agents.
- Diuretics– If your chronic bronchitis is complicated by right heart failure, you may be treated with tablets to remove the excess fluid.
For more health information on chronic bronchitis and appropriate treatment for yourself, please consult your local doctor.
Chronic Bronchitis References
- Cotran R, Kumar V, Collins T. Robbins Pathological Basis of Disease Sixth Ed. WB Saunders Company 1999.
- Ekberg-Jansson A, Larsson S, Löfdahl C. Preventing exacerbations of chronic bronchitis and COPD: Two recent Cochrane reviews report effective regimens, BMJ 2001;322:1259-1261
- Kerstijens H. Stable chronic obstructive pulmonary disease, BMJ 1999;319:495-500.
- Kumar, Clark. Clinical Medicine. 5th Edition. Saunders. 2002.
- Longmore, Wilkinson, Rajagopalan. Oxford Handbook of Clinical Medicine. 6th Edition. Oxford University Press. 2004.
- McKenzie D, Frith P, Burdon J, Town G. The COPDX Plan: Australian and New Zealand Guidelines for the management of Chronic Obstructive Pulmonary Disease 2003, MJA 2003; 178: S1-S40. Available [online] at URL: http://www.mja.com.au/public/issues/178_06_170303/tho10508_all.html
- Murtagh J. General Practice, 3rd Edition, McGraw-Hill, Sydney, 2003.
- Reilly J, Silverman E, Shapiro S. ‘Chronic Obstructive Pulmonary Disease,’ in Kasper et al. Harrison’s Principle of Internal Medicine, 16th Edition (Chapter 242), McGraw-Hill, 2006.
- Talley NJ, O’Connor S. Clinical examination- A Systematic Guide to Physical Diagnosis, 4th Edition. MacClennan & Petty, Sydney 2001.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







