- What is the urinary system and how does it work?
- What controls the process of urination?
- The urinary cycle
What is the urinary system and how does it work?
The urinary system is divided into upper and lower sections. The upper urinary system is made up of the kidneys and a tube called the ureter, which transports urine from the kidney to the bladder. There is one kidney for each side of the body and each kidney has its own ureter.
The lower urinary system consists of the bladder and another tube called the urethra, which transports urine from the bladder out of the body. The function of the urinary system is to remove waste products from the body, regulate water and salt balance, and to store and transport urine.
Upper urinary system
Kidneys
The kidneys are a pair of bean-shaped organs located near your back and just below the ribcage. The right kidney sits a little higher than the left because of the position of the liver. In an adult, the average kidney is 10 cm long, 6 cm wide and 3 cm thick, and weighs about 150 g.
The outer surface of the kidney is curved outwards, while the inner surface is curved inwards, just like a kidney bean. Several important structures enter and leave the kidney from its inner surface, including the ureter, blood vessels, nerves and lymphatic vessels.
The kidney is covered in three layers, including an inner layer, a fatty middle layer and a tough outer layer which protects the kidney from trauma. Under these layers lies the inside of the kidney, which is made up of inner and outer sections responsible for making urine. Blood flows into the kidney and is filtered through little units known as nephrons to make urine, which then passes via the ureter to the bladder.
The main roles of the kidneys are to remove waste substances from the blood, create a balance between water and salt in the body, and to produce hormones.
Ureter
The tubes that connect the kidneys to the bladder, known as the ureters, are approximately 30 cm long and 6 mm wide. They enter the bladder from behind and at an angle which creates a valve that stops urine from back-tracking up to the kidneys. The wall of the ureter is made up of three layers, including a layer of muscle which helps it to contract and propel urine from the kidney to the bladder.
 |
For more information on the upper urinary tract, see Anatomy of the Renal System. |
Lower urinary system
Bladder
The bladder is a hollow muscular organ that lies just behind the pubic bone. In males, the prostate gland sits behind the bladder, whereas in females, the vagina and uterus sit behind the bladder.
The bladder wall is made up of three layers. The innermost layer lines the bladder, the middle layer is made up the detrusor muscle, and the outermost layer surrounds the bladder. The detrusor muscle is made up of two different types of muscle which allow the bladder to contract and empty itself of urine.
At the bottom of the bladder is a triangular-shaped region known as the trigone. Urine enters the bladder from the ureters at the uppermost aspect of the trigone, and leaves the bladder via the urethra at the lowermost aspect of the trigone.
The bladder neck is a funnel-shaped extension at the bottom of the bladder that then connects with the urethra. It is 2–3 cm long and forms a muscular band around the urethra, known as the internal sphincter. This sphincter is normally closed tight to stop urine from leaking out of the bladder. When one decides to pass urine, the sphincter relaxes and urine can leave the bladder and pass into the urethra.
Male urethra
The urethra is a tube that runs from the bottom of the bladder to the opening where urine exits the body. In males, it is responsible for transporting both urine and sperm. The average male urethra is approximately 20 cm in length and is divided into four different parts along its course.
At the lower aspect of the urethra lies the external sphincter, which is formed by two groups of muscles which wrap around the urethra. The first component of this sphincter comes from the pelvic floor muscles, which form a sling around the urethra. This component only works to stop urine leaking when there is a sudden rise in pressure, for example, when one coughs, sneezes or lifts something heavy. The second component of the sphincter is formed by muscle from within the urethral wall itself. This component offers a more sustained level of tightening and is therefore the most important when it comes to stopping urine from leaking out of the bladder in males.
 |
For more information on the lower urinary tract in males, see Anatomy of the Male Urogenital System. |
Female urethra
The female urethra is much shorter than the male urethra and is only 4 cm long. Urine leaves the body via an opening in the urethra, which sits in front of the vagina. As with males, females also have an external sphincter which has two components. Contrary to males, the most important components to stop leakage of urine in females are the pelvic floor muscles which wrap around the urethra. Muscle in the wall of the urethra also contributes to the external sphincter mechanism in females.
 |
For more information on the lower urinary tract in females, see Anatomy of the Female Urogenital System. |
What controls the process of urination?
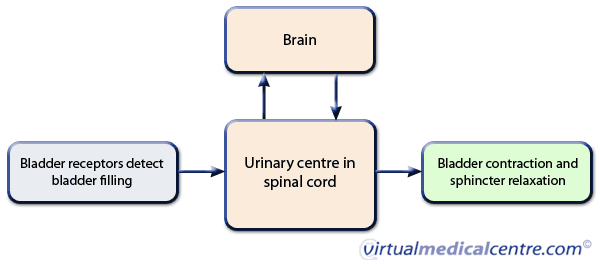
The process of urination is controlled by a complex circuit of nerves which relay messages between the bladder, the spinal cord and the brain.
Receptors within the bladder wall sense how full the bladder is and send this information to a urinary centre located at the bottom of the spinal cord. This region, known as the spinal micturition centre, co-ordinates signals going to and from the bladder as well as signals to and from the brain.
Until approximately 2–4 years of age, a simple circuit is involved in the process of urination. At this age, the central nervous system is immature and urination is therefore an involuntary process over which the child has no control. As the bladder fills, receptors in its wall send a message to the spinal micturition centre. The centre in turn sends a message to the detrusor muscle telling it to contract, and to the sphincters telling them to relax. This results in emptying of the bladder and urine being passed from the body.
As the brain matures with age, we develop the ability to control this process and choose an appropriate time and place to urinate. This conscious control over the process of urination is the result of a specialised area within the brain which communicates with the spinal micturition centre. This area in the brain blocks the signal that runs from the spinal cord to the bladder to initiate urination. When it is time to pass urine and an appropriate time and place are available, this region of the brain gives a ‘safe signal’, resulting in activation of the bladder, relaxation of the sphincters and the passage of urine.
Figure 1: Simplified illustration of connections between the bladder, spinal cord and brain.
Information on re-publishing of our images
The urinary cycle
Micturition, also referred to as urination or voiding, refers to the act of emptying the bladder of urine. It has two phases, known as the filling and voiding phases.
Filling phase
The bladder is very elastic and designed well for its role of urine storage. As the bladder fills, it expands and its muscular wall stretches and thins out, allowing for large amounts of urine to collect without a significant rise in pressure. During this filling phase, the brain blocks messages from the spinal cord to the bladder, which stops the bladder from emptying. When a bladder volume of about 200 mL is reached, receptors in the bladder wall send a signal to the spinal cord and up to the brain. If urination is not appropriate at this time, the brain blocks the signal from the spinal cord that would normally activate the bladder.
Voiding phase
Voiding requires the co-ordinated relaxation of the external sphincter and contraction of the detrusor muscle of the bladder. Signals from the spinal cord cause the muscle in the wall of the urethra to relax. After this, the pelvic floor muscles relax, causing the bladder neck to open. At the same time, a separate signal tells the detrusor muscle to tighten, which forces urine out of the bladder and causes the external sphincter to open and urine to pass from the body. As the bladder empties and the flow of urine stops, the brain sends a signal to close the external sphincter, stopping the passage of any further urine. Once the emptying cycle is finished, the brain re-activates its block on signals travelling from the spinal cord to the bladder and the filling cycle begins again.
References
- Fillingham S, Douglas J. Urological Nursing (3rd edition). Edinburgh: Baillière Tindall; 2004. [Book]
- Bullock N, Sibley G, Whitaker RH. Essential Urology. Edinburgh: Churchill Livingstone; 1989. [Book]
- Marieb EN, Hoehn KN. Anatomy and Physiology (3rd edition). San Francisco: Pearson Benjamin Cummings; 2008. [Book]
- Fowler CJ, Griffiths D, de Groat WC. The neural control of micturition. Nat Rev Neurosci. 2008;9(6):453-66. [Abstract | Full text]
- Blok BF. Central pathways controlling micturition and urinary continence. Urology. 2002;59(5 Suppl 1):13-7. [Abstract]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.