- Introduction to sweating
- Anatomy of sweat glands
- Innervation of the sweat glands
- Thermoregulatory sweating (body temperature control)
- Non-thermoregulatory sweating
Introduction to sweating
Sweat is a clear, odourless solution secreted by sweat glands, which are also known as sudoriferous glands. It is hypotonic, meaning that it has a lower concentration of electrolytes than the cells of the sweat glands. The body has millions of sweat glands which lie within the deep layers of the skin and connect via ducts to the epidermis (outer layer of skin) before opening out onto the skin surface.
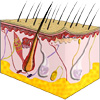 |
For more information, see Anatomy of the Skin. |
Sweating is the primary mechanism by which the human body regulates its temperature. It occurs during waking and sleeping. Sweat glands secrete sweat in response to nervous stimuli, primarily heat stimuli, but also emotional and gustatory (food) stimuli.
What is sweat?
Sweat consists primarily of water and electrolytes. The primary electrolytes contained in sweat are sodium and chloride. Potassium, urea, lactate, amino acids, bicarbonate and calcium are also found. Approximately 1% of the total volume of sweat consists of proteins, including immunoglobulins (proteins that function as antibodies) and glycoproteins (proteins joined to carbohydrates which perform a range of functions in the body). It is acidic, with a pH of 4–6.
Anatomy of sweat glands
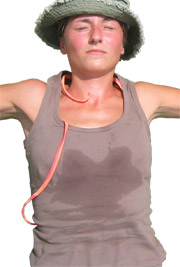
- Eccrine sweat glands: Constitute some 75% of all the body’s sweat glands (~3 million);
- Apocrine sweat glands: Comprise the other 25% (~1 million);
- Apoeccrine sweat glands: Mixed-type sweat glands known as apoeccrine glands are also found in humans.
Eccrine sweat glands
Eccrine sweat glands are tubular structures with long branches. They consist of:
- A tightly coiled tubular portion responsible for secreting sweat, located deep within the skin layers. The tubular portion is 60–80 µm in diameter and 2–5 mm in length; and
- A straight duct portion that transports the sweat to the skin surface. The duct portion fuses with the papillary layer of the dermis (the layer underlying the skin surface) and opens onto the skin surface. The duct portion is also 2–5 mm in length, but is slightly narrower in diameter compared to the tubular portion.
The eccrine glands consist of three cell types:
- Dark cells: Cover most of the surface of the cavities in the secretory or tubular portion of the eccrine sweat gland;
- Clear cells: Rest directly on the basement membrane (a thin, fibrous layer separating the inner and outer layers of skin) or on myoepithelial cells; and
- Myoepithelial cells: Spindle-shaped cells which lie between the secretory cells of the sweat glands and the basement membrane, close to the junction between the tubular and secretory portion of the eccrine sweat gland. These cells are also found in apocrine glands.
Eccrine sweat glands develop in utero (during foetal development) and are distributed over the entire body, with the exception of the lip margins, nail beds, nipples, the inner surface of the prepuce (foreskin), labia minora (outer folds of skin of the vulva/vagina), glans penis (head of the penis) and glans clitoris. The distribution of eccrine sweat glands at other body sites is uneven. Sites at which eccrine glands are heavily concentrated include:
- Soles of the feet: 620 ± 20 per cm2;
- Palms of the hands: 300 ± 80 per cm2;
- Armpits: 360 ± 60 per cm2;
- Forehead: 360 ± 60 per cm2; and
- Cheeks: 300 ± 80 per cm2.
Sites which have a low concentration of eccrine glands include:
- Trunk: 65 ± 20 per cm2; and
- Extremities (arms and legs): 120 ± 30 per cm2.
Apocrine sweat glands
Apocrine glands occur mainly in the arm pit, the areola of the nipples, and the perineum (region separating the anus from the genitals). They can also be found in the ear and eyelid. They are small and inactive before puberty. At puberty they increase in size, and in adults, apocrine glands are larger than eccrine glands.
Like the eccrine glands, they consist of secretory and ductal portions. In apocrine glands, the secretory portion is a tube consisting of a single layer of secretory cells arranged in a column and surrounded by myoepithelial cells. The ductal portion is short compared to the eccrine gland, and opens into the hair follicle, rather than to the skin surface.
Apoeccrine sweat glands
Apoeccrine glands are primarily found in the armpits and peri-anal region. They are larger than typical eccrine glands and smaller than apocrine glands. Like eccrine glands, the ductal portion of apoeccrine glands opens out to the skin surface. They are thought to arise from eccrine glands during puberty.
The secretory portion of apoeccrine glands consists of an irregularly wide section with a cell structure similar to apocrine glands and a narrower segment similar in structure to the eccrine gland. It secretes a thin watery sweat.
Innervation of the sweat glands
Nerve fibres which send signals to sweat glands arise in the sympathetic nervous system (a section of the nervous system that controls involuntary muscle movement). Nerves in different vertebrae of the thoracic (T) and lumbar (L) portions of the spinal cord supply sweat glands at different body sites:
- Upper limbs are supplied by nerves arising in vertebrae T2–8;
- Lower limbs are supplied by nerves arising in vertebrae T10–L2;
- Face and eyelids are supplied by nerves arising in vertebrae T1–4;
- Trunk is supplied by nerves arising in vertebrae T4–12.
Eccrine sweat glands
Eccrine sweat glands are innervated by (receive nerve signals from) the sympathetic nervous system via a chemical called acetylcholine, which is a neurotransmitter (a substance that transmits nerve signals from the brain). The sympathetic nerves which transmit signals to sweat glands in the arm are found in spinal cord segments T2–T6. Nerve fibres originating in spinal cord segments C5–T1 send signals to the sympathetic nerves in the T2-6 vertebrae.
Apocrine sweat glands
Apocrine glands are not situated close to nerve fibres and are thought to be regulated by androgens (hormones such as testosterone) rather than nerve stimuli.
Thermoregulatory sweating (body temperature control)
Eccrine sweat glands
Thermoregulatory stimuli (heat) stimulate the release of acetylcholine (the neurotransmitter) from nerve endings in the eccrine glands and catalyse sweat secretion. Sweat secretion plays an important role in thermoregulation. The amount of sweat produced differs under different environmental conditions and increases with increasing heat. Eccrine glands collectively have the capacity to produce up to 10 litres of sweat each day. Under normal conditions, only 5% of the glands are active at any given time and 0.5–1 L of sweat is produced per day. However, humans are typically able to produce 1.4 L/hour of sweat when exposed to heat or during exercise.
Increases in sweating occur due to an increase in the number of active sweat glands (in the initial phase of sweating) and an increase in the volume of sweat produced by each gland (in sustained sweating). Most of the sweat glands are activated within 8 minutes of exercise or passive exposure to heat. Subsequently, increases in the volume of sweat produced per gland occur gradually, until exercise or heat stress is withdrawn, or after 4–6 hours of prolonged heat stress when sweating reduces regardless of stimuli. The mechanisms that down-regulate sweating (decrease sweat production) during prolonged heat exposure or exercise are not well understood.
Eccrine glands consist of clear and dark cells, which have distinct functions. The clear cells secrete water and electrolytes, the main salts found in sweat. The dark cells secrete glycoproteins, the key proteins in sweat. Sweating is catalysed by acetylcholine, which binds to receptors thought to be located in the membrane of clear eccrine gland cells. When acetylcholine receptors are activated, a series of electrolyte exchanges between the cytoplasm (a gel-like substance that gives the cell its shape) and the fluid surrounding the cell are triggered.
In the first of the series of electrolyte exchanges, calcium electrolytes contained in the watery fluid secreted by a clear cell flood back into the clear cell’s cytoplasm. This in turn causes potassium chloride electrolytes to flood out of the cytoplasm, as the cell attempts to regulate its electrolyte and water concentration. The efflux (flooding out) of potassium chloride electrolytes in turn catalyses an influx (flooding in) of nitrogen, potassium and chloride electrolytes. At this point, there is an increase in the concentration of sodium electrolytes within the clear cell’s cytoplasm.
The increased concentration of sodium stimulates sodium pumps, which push sodium electrolytes out of the cell and draw in potassium electrolytes from the fluid surrounding the cells. At the same time, chloride ions move into the cell, assisted by sodium–potassium–chloride co-transporters, causing the membrane of the cell to attract sodium electrolytes. Chloride and sodium electrolytes then bind together to form sodium chloride, a key component of the primary solution from which sweat is produced. The primary solution, which is slightly acidic and isotonic (containing an equal concentration of electrolytes as the cell), is secreted from the tubular portion of the eccrine gland to the duct portion.
The tubular portion of the eccrine gland then reabsorbs sodium chloride in the solution to preserve electrolyte balance. Following reabsorption of sodium chloride from the primary solution, a hypotonic solution (sweat) remains and is secreted to the skin via the sweat gland duct.
Apocrine sweat glands
Apocrine glands increase in size and begin to function after puberty, a process that is regulated by androgens (male hormones). Following puberty, they secrete a solution that is thicker than sweat and contains fatty acids and proteins. It also smells. The odour of sweat occurs due to bacterial decomposition of sweat and the solution secreted from the apocrine glands, which contains lipids, cholesterol and steroids.
The apocrine glands are evolutionary remnants; they have no known function in humans, although in other mammals they function to produce odours that attract the opposite sex. Some hypothesise that apocrine secretions play a role in thermoregulation by emulsifying eccrine sweat and causing it to form a sweat layer over the skin.
Non-thermoregulatory sweating

Eccrine sweat glands
Eccrine sweat glands cover most of the body’s surface and are the source of excessive perspiration. In addition to heat stimuli, the eccrine glands also respond to emotional and gustatory (food) stimuli which can cause non-thermoregulatory, pathological sweating. Increased mental stress increases sympathetic nerve activity, which leads to increased sweating. Hyper-functioning of the hypothalamus during exercise is also thought to increase thermoregulatory sweating.
Excessive sweating is most likely to occur at the sites where eccrine glands are concentrated (armpits, palms, soles and face) in focal hyperhidrosis, a condition characterised by excessive sweating at distinct anatomical sites.
Apoeccrine sweat glands
The function of apoeccrine sweat glands in excessive sweat production is not well understood. However, in some focal hyperhidrosis patients, they are highly concentrated in the armpit region where they can comprise up to 45% of all sweat glands. This suggests they may have a role in non-thermoregulatory sweating.
References
- Marieb EN. Essentials of Human Anatomy and Physiology (7th edition). New York, NY: Prentice Hall; 2002. [Book]
- Kreyden OP, Scheidegger EP. Anatomy of the sweat glands, pharmacology of botulinum toxin, and distinctive syndromes associated with hyperhidrosis. Clin Dermatol. 2004;22(1):40-4. [Abstract]
- Eisenach JH, Atkinson JL, Fealey RD. Hyperhidrosis: Evolving therapies for a well-established phenomenon. Mayo Clin Proc. 2005;80(5):657-66. [Abstract | Full text]
- Haider A, Solish N. Focal hyperhidrosis: Diagnosis and management. CMAJ. 2005;172(1):69-75. [Abstract | Full text]
- Saga K. Histochemical and immunohistochemical markers for human eccrine and apocrine sweat glands: An aid for histopathologic differentiation of sweat gland tumors. J Investig Dermatol Symp Proc. 2001;6(1):49-53. [Abstract | Full text]
- Collin J, Whatling P. Treating hyperhidrosis: Surgery and botulinum toxin are treatments of choice in severe cases. BMJ. 2000;320(7244):1221-2. [Full text]
- Lindsay SL, Holmes S, Corbett AD, et al. Innervation and receptor profiles of the human apocrine (epitrichial) sweat gland: Routes for intervention in bromhidrosis. Br J Dermatol. 2008;159(3):653-60. [Abstract]
- Shibasaki M, Wilson TE, Crandall CG. Neural control and mechanisms of eccrine sweating during heat stress and exercise. J Appl Physiol. 2006;100(5):1692-701. [Abstract | Full text]
- Porter AM. Why do we have apocrine and sebaceous glands? J R Soc Med. 2001;94(5):236-7. [Abstract | Full text]
- Hyperhydrosis: Aetiology [online]. London: BMJ Best Practice; 1 December 2010 [cited 22 November 2011]. Available from: URL link
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.





