- What is sleep?
- What drives sleep?
- Why do we need sleep?
- How much sleep is normal and how much is needed?
- Oversleeping is detrimental
- Sleep patterns as we age
- Morning people versus evening people
- Napping
What is sleep?
Sleep is a state of reduced awareness and responsiveness. In humans, sleep is also associated with reduced movement.
Sleep consists of two different phases:
- Rapid eye movement (REM) sleep; and
- Non-REM sleep or slow wave sleep.
REM sleep

The brain is extremely active during REM sleep. The electroencephalogram shows patterns of brain wave activity similar to those that occur during the waking hours. Due to this feature of REM sleep, it is often also referred to as paradoxical sleep as it is a paradox that one can be asleep and yet the brain is incredibly active.
Non-REM sleep
In contrast, non-REM sleep is characterised by deep sleep. The duration of REM sleep episodes is longer earlier in the night when one is most tired. As one becomes more rested during the night, the duration of REM sleep episodes decreases.
During non-REM sleep the blood pressure, breathing and metabolic rate are all depressed significantly. Bodily movements do not occur during non-REM sleep.
Non-REM sleep is also referred to as slow wave sleep as during this period the brain waves are very strong and of a very low frequency (i.e. slow).
While non-REM sleep is sometimes referred to as dreamless sleep, dreams and even nightmares can occur during non-REM sleep. These are not associated with movement and are not remembered as they are not consolidated to memory during this sleep phase.
Sleep cycles
REM sleep occurs at about 90 minute intervals. There are usually 4 to 6 cycles of REM and non-REM sleep each night. Later into the night, the REM episodes become longer and non-REM sleep becomes shorter and lighter.
Non-REM sleep can be defined as stage 1, 2, 3 or 4. Stages 1 and 2 are often referred to as light sleep and stages 3 and 4 as deep sleep, slow wave sleep or delta sleep.
Brain wave activity (EEG) during wakefulness and sleep
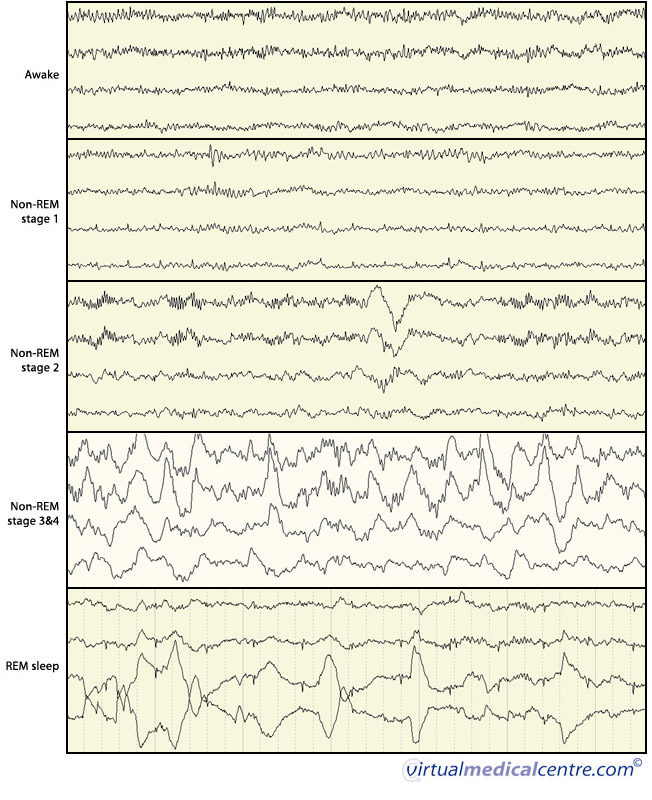
What drives sleep?
Homeostatic drive

Adaptive drive
This includes a number of mechanisms which effect but are independent of the duration of wakefulness and the circadian rhythm.
Mental stimulation prior to bedtime can make falling asleep difficult, particularly if there are worries or anxieties that cannot be resolved. The ability to relax the body (mentally and physically) affects whether one is able to initiate sleep.
The level or lack of sensory inputs also influences our ability to fall asleep. A number of these sensory inputs include:
- Pain and discomfort: Awakening during the night is more common in individuals with chronic disease such as rheumatoid arthritis or multiple sclerosis. Pain is also associated with increased tossing and turnings that also result with increased awakenings during the night;
- Temperature: An ambient temperature of 18 °C is ideal for falling asleep and staying asleep. Increased and decreased temperatures result in disrupted sleep;
- Physical activity: Exercise promotes wakefulness during the activity and also for 3 hours after the activity. Exercise close to the time of going to bed can delay and decrease melatonin secretion. This is important as melatonin is a hormone produced by the pineal gland which promotes sleep;
- Sexual activity: Unlike other forms of activity, sexual intercourse usually promotes falling asleep;
- Noise: A noisy environment can impair sleep and increase arousal from sleep. The noise level that causes an individual to wake varies between people and also changes with age. A person is also more likely to wake up if the noise is significant to the person, the crying of an infant to its parents;
- Hunger: Hunger is associated with wakefulness. Carbohydrates and milky drinks that contain tryptophan, a compound which is broken down in the body to produce melatonin, are excellent at promoting sleep. Bananas, peanuts and figs are also rich sources of tryptophans. High protein foods are rich in tyrosine (a hormone which promotes wakefulness) and can lead to wakefulness. Large meals can cause reflux and heartburn and also drive wakefulness; and
- Light exposure: Seasonal changes in the duration of daylight affect the sleep-wakefulness cycle. During sleep, 5-10% of light reaches the retina and light exposure can result in arousal from non-REM sleep. Light exposure during the day also increases alertness, motor function and mood, elevates body temperature and heart rate.
A separate effect of light is on the circadian rhythm. This effect is mediated at a specific region in the brain called the suprachiasmatic nuclei (SCN) and suppresses melatonin levels.
Circadian rhythm

The circadian rhythm is generated by a “biological clock” whose activity is modulated by various external stimuli. These external cues ensure that the internal clock is in sync with the external environment.
Special cells within the retina of the eye provide the input to the SCN. The SCN in turn influences melatonin secretion from the pineal gland. Melatonin is synthesised from tryptophan. Melatonin production can be increased by an increased oral intake of tryptophan and vitamin B6 (a co-enzyme in tryptophan metabolism) such as by consuming carbohydrates, milk, bananas, figs and peanuts, so consuming these can help an individual to fall asleep. Melatonin secretion is increased by selective serotonin reuptake inhibitors (anti-depressants) and antipsychotics. Melatonin release is inhibited by caffeine, beta-blockers, benzodiazepines and non-steroidal anti-inflammatories, and their consumption can make it more difficult to sleep.
Regimented times for going to bed, going to sleep, waking and getting up are important for reinforcing circadian rhythm. The most important of these is the time of waking because it helps to ensure that the homeostatic drive to sleep is strong.
Why do we need sleep?

Biochemical
Different hormones are secreted depending upon whether an individual is asleep or awake. For example growth hormone is secreted during sleep while cortisol is secreted during wakefulness.
Metabolic rate falls during non-REM sleep, energy is conserved and body temperature drops. During this period protein synthesis and the production of complex molecules within the body is increased.
When we are awake our brain cells use a considerable amount of glucose to function and the intracellular glycogen stores become depleted. During sleep this process is reversed so that glucose is available during the next bout of wakefulness.
Physiological
Sleep has been considered a restorative or a recovery phase that prepares the body for the next episode of wakefulness. Cell division is more rapid during non-REM sleep and sleep has an important function on the immune system.
Neurological
Sleep may have some role in development of brain cells and connections between brain cells during development. The ability to form new neurons (neurogenesis) slows early in life and it is the development of new neuronal networks that is responsible for new behaviours.
Synchronisation of cortical activity during non-REM sleep may in some way coordinate cortical connections. The prefrontal cortex is inactive during all phases of sleep (this may also confer some benefit). During REM sleep the cerebral cortex is open to sensory inputs and forms loose associations that cannot be formed during wakefulness.
Psychological
Both phases of sleep are involved in memory consolidation. Very little new information is gained during sleep, but consolidation and maintenance of memory from experiences of the previous day is considerable. It is known that learning of visual information is improved during the first night of sleep and that sleep deprivation impairs recall of the information. Different types of sleep have a different effect on memory consolidation and retention of information. Retention is best if stage 3 and 4 non-REM sleep occurs in the first 2 hours of sleep and if the last 25% of sleep is REM sleep.
The type of sleep also affects the type of information which is consolidated by the brain. Learning of movement sequences is best if stage 2 non-REM sleep occurs late in the night, while learning of cognitive sequences occurs best if there is a cycle of REM and non-REM sleep.
Dreams are a manifestation of underlying brain activity and reflect the loose associative connections made during REM sleep. These loose associations are likely to result in increased creative mental activity and problem-solving abilities.
How much sleep is normal and how much do I need?

The daily sleep requirements decline steadily as we age, from 16 hours a day in infants to 7.5-8,5 hours in young adults. It then levels off before decreasing further in the elderly.
Less than 5-6 hours of sleep in a night is usually associated with symptoms of sleep deprivation.
For more information on good sleep practices, see Sleep Hygiene.
Oversleeping is detrimental
People who sleep for more than 8 hours per night have been shown to have a higher mortality. There are no benefits of oversleeping, and like overeating, it can cause problems. As the duration of a sleeping episode increases, the length and depth of non-REM sleep increases.
Sleep inertia is a mixed wake-sleep state and is the feeling of drowsiness upon waking. Oversleeping can make it become more prominent and drawn out. Sleep inertia can last between 30 and 120 minutes after waking. Sleep the following night may become fragmented as a result of the oversleeping.
Sleep patterns as we age
Adults tend to sleep once (monophasic sleep) during a 24-hour period. In contrast, children have polyphasic sleep. Infants around 6 months of age tend to sleep for 3-5 hours during the day and children of 2 years of age, sleep for around 2 hours during the day. In newborns the cycles of sleep and wakefulness are almost random, until their circadian rhythm matures between 3 and 6 months of age. Once their circadian rhythm is operating, infants usually sleep more at night time than during the day. Elderly individuals often revert back to a polyphasic sleep pattern.
REM sleep usually occurs half of the sleeping time in infants and then declines until the age of about 10 years, where it stabilises at approximately 25 % of total sleep time.
Children sleep through noise more than adults. However, the elderly are more easily aroused from sleep by noise (unless they are deaf). The threshold for arousal increases from stage 1 sleep through to stage 4 non-REM sleep. Arousal is therefore more likely later in the night after the initial bouts of stage 3 and stage 4 non-REM sleep have occurred.
Morning people versus evening people

Morning people:
- Have a shorter duration to entering stage 3 and 4 non-REM sleep;
- Are unable to sleep late in the mornings;
- Often complain of poor sleep quality with more frequent night time awakenings;
- Earlier melatonin peak and temperature low;
- Shorter circadian cycle;
- Longer delay between temperature low and waking, waking occurs later in the circadian cycle and as a result they are more alert soon after waking;
- Intolerant to nightshift work; and
- Sleep longer by going to bed earlier.
Evening people:
- Sleep is more closely associated with light;
- Later melatonin peak and temperature low;
- Longer circadian cycle;
- Wake closer to minimum temperature;
- Can tolerate nightshift work;
- Cope better with changing timezones; and
- Sleep longer by waking later.
Napping
Daytime naps are normal in young children and the elderly, and are taken especially between 2 pm and 4 pm when the circadian rhythm favours sleep. They are often taken to compensate for sleep debt accrued at night and daytime tiredness.
Stages 3 and 4 of non-REM sleep are more likely if the nap occurs after being awake for a long period, i.e. in the afternoon. These sleep stages are also more likely if the naps lasts for more than about 60 minutes and is unlikely if the nap is less than 20 minutes.
More information
 |
For more information about sleep, including how much is good for you, tips for getting more sleep, and sleep disorders, as well as some useful videos, see Sleep. |
References
- Shneerson JM. Sleep Medicine: A guide to sleep and its disorders (2nd edition). Oxford: Blackwell Publishing; 2005. [Book]
- Guyton AC, Hall JE. Textbook of Medical Physiology (11th edition). Philadelphia: Elsevier Saunders; 2005. [Book]
- Lee-Chiong TL. Sleep Medicine: Essentials and review. Oxford: Oxford University Press; 2008. [Book]
- Marieb EN, Hoehn KN. Anatomy and Physiology (3rd edition). San Francisco: Pearson Benjamin Cummings; 2008: 413-5. [Book]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







