- Human Respiratory System
- The Upper Airway and Trachea
- Human Lungs
- The Work of Breathing
- The Respiratory System Through the Ages
Human Respiratory System
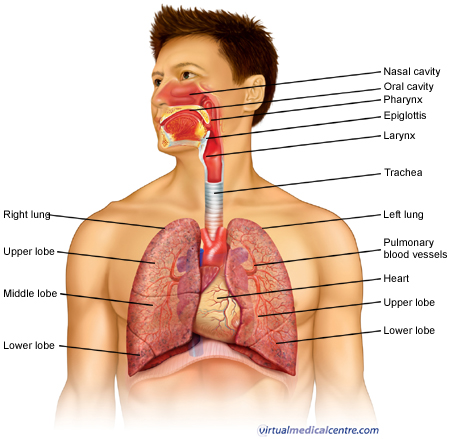
The respiratory system consists of all the organs involved in breathing. These include the nose, pharynx, larynx, trachea, bronchi and lungs. The respiratory system does two very important things: it brings oxygen into our bodies, which we need for our cells to live and function properly; and it helps us get rid of carbon dioxide, which is a waste product of cellular function. The nose, pharynx, larynx, trachea and bronchi all work like a system of pipes through which the air is funnelled down into our lungs. There, in very small air sacs called alveoli, oxygen is brought into the bloodstream and carbon dioxide is pushed from the blood out into the air. When something goes wrong with part of the respiratory system, such as an infection like pneumonia, it makes it harder for us to get the oxygen we need and to get rid of the waste product carbon dioxide. Common respiratory symptoms include breathlessness, cough, and chest pain.
The Upper Airway and Trachea
When you breathe in, air enters your body through your nose or mouth. From there, it travels down your throat through the larynx (or voicebox) and into the trachea (or windpipe) before entering your lungs. All these structures act to funnel fresh air down from the outside world into your body. The upper airway is important because it must always stay open for you to be able to breathe. It also helps to moisten and warm the air before it reaches your lungs.
The Lungs
Structure
The lungs are paired, cone-shaped organs which take up most of the space in our chests, along with the heart. Their role is to take oxygen into the body, which we need for our cells to live and function properly, and to help us get rid of carbon dioxide, which is a waste product. We each have two lungs, a left lung and a right lung. These are divided up into ‘lobes’, or big sections of tissue separated by ‘fissures’ or dividers. The right lung has three lobes but the left lung has only two, because the heart takes up some of the space in the left side of our chest. The lungs can also be divided up into even smaller portions, called ‘bronchopulmonary segments’.
These are pyramidal-shaped areas which are also separated from each other by membranes. There are about 10 of them in each lung. Each segment receives its own blood supply and air supply.
How they work
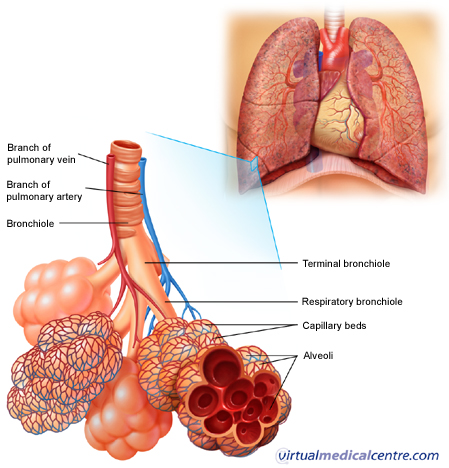
Air enters your lungs through a system of pipes called the bronchi. These pipes start from the bottom of the trachea as the left and right bronchi and branch many times throughout the lungs, until they eventually form little thin-walled air sacs or bubbles, known as the alveoli. The alveoli are where the important work of gas exchange takes place between the air and your blood. Covering each alveolus is a whole network of little blood vessel called capillaries, which are very small branches of the pulmonary arteries. It is important that the air in the alveoli and the blood in the capillaries are very close together, so that oxygen and carbon dioxide can move (or diffuse) between them. So, when you breathe in, air comes down the trachea and through the bronchi into the alveoli. This fresh air has lots of oxygen in it, and some of this oxygen will travel across the walls of the alveoli into your bloodstream. Travelling in the opposite direction is carbon dioxide, which crosses from the blood in the capillaries into the air in the alveoli and is then breathed out. In this way, you bring in to your body the oxygen that you need to live, and get rid of the waste product carbon dioxide.
Blood Supply
The lungs are very vascular organs, meaning they receive a very large blood supply. This is because the pulmonary arteries, which supply the lungs, come directly from the right side of your heart. They carry blood which is low in oxygen and high in carbon dioxide into your lungs so that the carbon dioxide can be blown off, and more oxygen can be absorbed into the bloodstream. The newly oxygen-rich blood then travels back through the paired pulmonary veins into the left side of your heart. From there, it is pumped all around your body to supply oxygen to cells and organs.
Book your health appointments online
Find and instantly book your next health appointment with Healthengine
The Work of Breathing
The Pleurae
The lungs are covered by smooth membranes that we call pleurae. The pleurae have two layers, a ‘visceral’ layer which sticks closely to the outside surface of your lungs, and a ‘parietal’ layer which lines the inside of your chest wall (ribcage). The pleurae are important because they help you breathe in and out smoothly, without any friction. They also make sure that when your ribcage expands on breathing in, your lungs expand as well to fill the extra space.
The Diaphragm and Intercostal Muscles
When you breathe in (inspiration), your muscles need to work to fill your lungs with air. The diaphragm, a large, sheet-like muscle which stretches across your chest under the ribcage, does much of this work. At rest, it is shaped like a dome curving up into your chest. When you breathe in, the diaphragm contracts and flattens out, expanding the space in your chest and drawing air into your lungs. Other muscles, including the muscles between your ribs (the intercostal muscles) also help by moving your ribcage in and out. Breathing out (expiration) does not normally require your muscles to work. This is because your lungs are very elastic, and when your muscles relax at the end of inspiration your lungs simply recoil back into their resting position, pushing the air out as they go.
The Respiratory System Through the Ages
Breathing for the Premature Baby
When a baby is born, it must convert from getting all of its oxygen through the placenta to absorbing oxygen through its lungs. This is a complicated process, involving many changes in both air and blood pressures in the baby’s lungs. For a baby born preterm (before 37 weeks gestation), the change is even harder. This is because the baby’s lungs may not yet be mature enough to cope with the transition. The major problem with a preterm baby’s lungs is a lack of something called ‘surfactant’. This is a substance produced by cells in the lungs which helps keep the air sacs, or alveoli, open. Without surfactant, the pressures in the lungs change and the smaller alveoli collapse.
This reduces the area across which oxygen and carbon dioxide can be exchanged, and not enough oxygen will be taken in. Normally, a foetus will begin producing surfactant from around 28-32 weeks gestation. When a baby is born before or around this age, it may not have enough surfactant to keep its lungs open. The baby may develop something called ‘Neonatal Respiratory Distress Syndrome’, or NRDS. Signs of NRDS include tachypnoea (very fast breathing), grunting, and cyanosis (blueness of the lips and tongue). Sometimes NRDS can be treated by giving the baby artifically made surfactant by a tube down into the baby’s lungs.
The Respiratory System and Ageing
The normal process of ageing is associated with a number of changes in both the structure and function of the respiratory system. These include:
- Enlargement of the alveoli. The air spaces get bigger and lose their elasticity, meaning that there is less area for gases to be exchanged across. This change is sometimes referred to as ‘senile emphysema’.
- The compliance (or springiness) of the chest wall decreases, so that it takes more effort to breathe in and out.
- The strength of the respiratory muscles (the diaphragm and intercostal muscles) decreases. This change is closely connected to the general health of the person.
All of these changes mean that an older person might have more difficulty coping with increased stress on their respiratory system, such as with an infection like pneumonia, than a younger person would.
More information
 |
For everything you need to know about Asthma, including the symptoms, risk factors, treatments and other useful resources, visit Asthma. |
References
- Ganong, W.F. Review of Medical Physiology (seventeenth edition). New Jersey, Prentice-Hall, 1995.
- Jannsens, JP, Pache JC, Nicod LP. ‘Physiological changes in respiratory function associated with ageing,’ European Respiratory Journal. 1999, 13(1):197-205
- Johnson, L.R. Essential Medical Physiology (second edition). Philadelphia, Lippincott Williams & Wilkins, 1998.
- Last, L.J. Aids to Anatomy (twelfth edition). London, Balliere, Tindall & Cassell, 1962.
- Moore, K.L., Dalley, A.F. Clinically Oriented Anatomy (fourth edition). Baltimore, Lippincott Williams & Wilkins, 1999.
- Robinson, M.J., Roberton, D.M. Practical Paediatrics (fifth edition). Sydney: Churchill Livingstone, 2003.
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.