- What is dialysis?
- Kidneys
- Types of dialysis
- Nutrition during dialysis
- Nutritional management
- Nutrient supplementation
- Nutritional status monitoring in dialysis
- Important dietary tips for dialysis patients
What is dialysis?
Dialysis is a treatment which removes waste products normally filtered by the kidney from the blood. It is used for people who have kidney or renal failure. Proper nutrition is even more important for these people as they must ensure that unnecessary waste products are not added to their system through their diet.
Kidneys
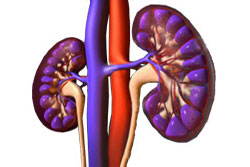
The rate at which the nephrons filter waste from the blood is measured as the Glomerular Filtration Rate (GFR). A GFR score in the range of 90-120 ml/min is usually an indication of a normal kidney function. A GFR of 4-5 ml/min warrants dialysis.
Types of dialysis
Dialysis is a process by which waste products are removed from the blood in the event of kidney failure. There are two main forms of dialysis – haemodialysis and peritoneal dialysis. In haemodialysis, the blood is cleaned outside the body via a machine, and in the process of peritoneal dialysis the blood is filtered through the peritoneal membrane located in the abdomen. The common feature of both types of dialysis is the removal of wastes and excess fluids from the body.
Either type of dialysis may be referred to as maintenance dialysis when it is provided on an ongoing basis in an outpatient setting (e.g. the person’s home or any time other than during hospital admission). Maintenance dialysis is provided to those people with kidney failure who have received initial treatment and had their condition stabilised.
Nutrition during dialysis

Nutritional management
Because the kidneys of people on dialysis are unable to cope with excess fluid and other metabolic wastes, it is vital that the nutrient content of foods consumed by these people is carefully balanced. Individuals using dialysis often consume inadequate quantities of macronutrients (energy measures as calories or kilojoules), fluids (water) and/or important micronutrients (vitamins, minerals and trace elements). Evidence suggests that the build up of toxins that can occur with renal failure can also suppress the appetite. As a result, people being treated with dialysis often reduce the amount of food they consume.
Nutritional imbalances in individuals treated with dialysis
Protein-energy malnutrition
Malnutrition is common in people being treated with dialysis and close to 40% suffer from varying degrees of protein-energy malnutrition. Protein energy malnutrition is a form of malnutrition in which the individual does not consume enough of their macronutrients (calories) in the form of proteins like meat and legumes; they consume too much of their macronutrients in the form of carbohydrates. Protein energy malnutrition occurs in people eating less than the recommended amount of protein which is 1.2 g/kg body weight. It may occur even when a person’s overall macronutrient (energy) intake is adequate, meaning they are consuming 35 kcal/kg body weight if they are <60 years or 30 kcal/kg body weight if they are >60 years.
The causes of protein-energy malnutrition in people being treated with maintenance dialysis are varied including decrease in dietary protein and overall energy intake. Protein intake may be restricted because higher intake of protein requires higher doses of dialysis. Note lower intake of protein with sufficient energy intake requires lower doses of dialysis.
People on dialysis may not be aware of the recommended energy and protein intake unless they receive nutritional counselling from a health professional. It is important for people who are on dialysis to access nutritional counselling so they understand the importance of different foods and the types of nutrients they add to the diet, rather than simply follow a diet which restricts intake of certain foods.
Micronutrient deficiencies
Apart from protein-energy malnutrition, dialysis patients are also vulnerable to micronutrients deficiencies because dialysis can cause loss of water soluble vitamins such as vitamins B and C.
Micronutrient excesses

Vitamin A
Vitamin A is a fat soluble vitamin which unlike water soluble vitamins (e.g. vitamin C) is not removed from the body through dialysis. The kidneys play a major role in removing vitamin A and its by-products (especially retinol) from the body. In people with kidney failure concentrations of Vitamin A in the blood stream typically increase. However the vitamin A in the blood stream is less likely to be taken up by the body’s tissues and cells, where it is used for repair and maintenance.
There is a need for further research to properly understand the role of Vitamin A in dialysis and whether or not people on dialysis treatment should receive vitamin A supplements. On the one hand there are concerns that giving people on dialysis vitamin A supplements may lead to excessive concentrations in the blood stream and have toxic effects. On the other hand there is evidence that low vitamin A levels in dialysis are associated with an increased risk of death from heart problems.
Phosphorus
Foods rich in phosphorus (e.g. dairy products, nuts, beans, lentils, cola drinks, beer, and cocoa drinks) increase the phosphorus level in the blood. Unfortunately, dialysis is unlikely to remove accumulated levels of phosphorus in the blood and this can cause excessive amount of phosphorous to accumulate in the blood, which in turn cause the release of calcium from the bones. The continuous removal of calcium from the bones may eventually make them weak. It is also known that high accumulation of phosphorus in the blood results in the formation of what is called calcium-phosphorus crystals in the joints, muscle, blood and heart. The calcium-phosphorus crystals may pose problems such as bone pain, poor blood circulation and even damage to the heart.
Potassium
Persons undertaking haemodialysis may have to limit the intake of foods rich in potassium. Potassium is a mineral of importance to dialysis patients because impaired kidney function can lead to a rise in the level of potassium in the blood. Foods high in potassium include bananas, melons, oranges, potatoes, tomatoes, milk, poultry, and fish.
Sodium

- Swelling of the lower joints of the feet and hands;
- Increased weight associated with accumulated body fluids;
- Increase in blood pressure;
- Shortness of breath and
- Increased activity of the heart.
Fluid excesses
Factors that can lead to increased intake of fluids must be watched and avoided. Fluids include any food or beverage that remains liquid at room temperature, for example gravy, soups, ice cream, tea, coffee, juices, water, fizzy drinks.
Nutrient supplementation
Some supplements especially fat soluble micronutrients (e.g. vitamin A) may be harmful for people treated with dialysis as these can accumulate in the body. They should be avoided.
Nutritional status monitoring in dialysis
In order to prevent and treat malnutrition it is important that people being treated with dialysis have their nutritional status assessed by a health professional (e.g. dietician or/doctor). Nutritional assessment allows those individuals who are not yet malnourished but at risk of becoming malnourished to be identified.
Nutritional assessment is performed by examining nutritional indicators including:
- Fat and muscle mass: A clinical assessment of subcutaneous fat mass (FM) and muscle mass and a history of weight loss should constitute important parts of the routine nutritional assessment of protein energy malnutrition in people on dialysis. Loss in fat deposits and muscle mass gives an indication of under nutrition. Body mass index (BMI) is also an important indicator for the assessment of malnutrition especially that of obesity. Most dialysis patients with malnutrition also have accompanying diseases, in particular cardiovascular disease and inflammation, and so their assessment is an integral part of the nutritional assessment of dialysis patients.
- Serum creatinine: Creatinine is a waste product that emanates from normal metabolism of the body. It is removed from the body by the kidney. Therefore, creatinine levels may rise with increasing inability of the kidney to function. The normal blood creatinine level for males is usually less than 120 µmol/L and 90 µmol/L for females. Low creatinine levels may thus reflect normal kidney function or diet patterns.
- Serum albumin: Low levels may reflect inadequate intake of protein or calories.
Important dietary tips for dialysis patients
- Consume fresh or plain frozen vegetables which often contain no added salt.
- Choose canned fruits which usually contain less potassium than fresh fruits.
- Use non-dairy creamers that contain low phosphorus instead of milk.
- Read labels on food packages to guide in choosing foods with only permissible ingredients.
- Help reduce the salt content of your diet by using herbs and spices instead of common table salt.
More information
 |
For more information on nutrition, including information on types and composition of food, nutrition and people, conditions related to nutrition, and diets and recipes, as well as some useful videos and tools, see Nutrition. |
References
- Savica VSD, Ciolino F, Mallamace A, Calvani M, Savica R, Bellinghieri G. Nutritional therapy in chronic kidney disease. Nutr Clin Care 2005;8 (2):70-76.
- Michelle M Romano. Renal conditions. In: Lucinda K Lysen, ed. Quick Reference to Clinical Dietetics. Maryland: Aspen Publishers, Inc., 1997.
- Nakao T, Niwa T, Kaysen GA, et al. Nutritional management of dialysis patients: balancing among nutrient intake, dialysis dose, and nutritional status. American Journal of Kidney Diseases 2003;41 (No. 3, Supplement 1):S133-S136.
- Devine WCJ. Current Nutrition Management of Patients with Renal Diease. Top Clin Nutr 1992;7 (4):21-33.
- Acchiardo ML, Latour PA. Malnutrition as the main factor in morbidity and mortality of hemodialysis patients. Kidney Int. 1983;24 (16):199-203.
- National Kidney Foundation. Nutrition and hemodialysis guide. New York: National Kidney Foundation 2006: 1-16.
- Hoover H. Compliance in hemodialysis patients: a review of the literature. J Am Diet Assoc 1989;89 (7):957-959.
- Sherie Sourial. Barriers to nutritional supplement use in dialysis patients in Auckland district health board and counties manukau district health board Retrieved from: [URL Link] 2003.
- Stenvinkel P, Heimbürger O, Lindholm B, Kaysen GA, Bergström J. Are there two types of malnutrition in chronic renal failure? . Nephrol Dial Transplant 2000;15:953-960.
- Kidney Health Australia. Chronic Kidney disease. Australia: Kidney Health Australia: [URL Link] 2006.
- Massachusetts Government. Chronic Maintenance Dialysis Treatments and Home Dialysis Supplies. 2012. [cited 12 January 2015]. Available from: [URL Link]
- Ahmed S. Himmelfarb J. The ABCs of Micronutrients in Dialysis patients. Am J Kidney Dis. 2010; 56 (3): 431-33. [Full Text]
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







