- What is Ulcerative Colitis (Inflammatory Bowel Disease)
- Statistics on Ulcerative Colitis (Inflammatory Bowel Disease)
- Risk Factors for Ulcerative Colitis (Inflammatory Bowel Disease)
- Progression of Ulcerative Colitis (Inflammatory Bowel Disease)
- Symptoms of Ulcerative Colitis (Inflammatory Bowel Disease)
- Clinical Examination of Ulcerative Colitis (Inflammatory Bowel Disease)
- How is Ulcerative Colitis (Inflammatory Bowel Disease) Diagnosed?
- Prognosis of Ulcerative Colitis (Inflammatory Bowel Disease)
- How is Ulcerative Colitis (Inflammatory Bowel Disease) Treated?
- Ulcerative Colitis (Inflammatory Bowel Disease) References
What is Ulcerative Colitis (Inflammatory Bowel Disease)
Ulcerative colitis (UC) is a form of inflammatory bowel disease characterised by chronic and widespread inflammation of the colorectal mucosa. Inflammation of the mucosa leads to the formation of ulcers.
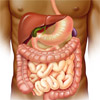 |
For more information on the bowel, see Anatomy of the Gastrointestinal System. |
UC is similar to another form of irritable bowel disease called Crohn’s disease in that both conditions are characterised by inflammation which is not caused by infection. Unlike Crohn’s disease, which can affect any part of the gastrointestinal tract (e.g. stomach, intestines), UC is confined to the large colon. It is often challenging for doctors to distinguish between the two conditions.
In UC, the inflammation extends from the rectum in a circumferential manner, typically affecting both sides of the colon in an uninterrupted pattern. Inflammation affects the rectum in over 95% of UC cases. Depending on the extent of the inflammation, UC can be further classified as:
- Proctitis: The least severe form of the disease, proctitis is characterised by inflammation of the rectal mucosa;
- Left-sided colitis: Characterised by limited inflammation of the colon;
- Extensive colitis: Characterised by extensive inflammation of the colon; or
- Pancolitis: Characterised by inflammation involving the entire colon.
UC may also be classified according to symptoms, as either:
- Mild: When the person passes < 4 stools daily (with or without blood) and no evidence of systemic toxicity;
- Moderate: When the person passes > 4 stools daily with minimal systemic toxicity;
- Severe: When the person passes > 6 bloody stools per day with signs of systemic toxicity, which may include fever, tachycardia (rapid heartbeat), and anaemia;
- Fulminant: When the person passes > 10 stools per day, continuous rectal bleeding needing blood transfusion, abdominal tenderness and distension, and systemic toxicity.
The image below shows the diffuse inflammatory changes of UC:
Statistics on Ulcerative Colitis (Inflammatory Bowel Disease)
Australia
While there are relatively few deaths caused by UC (only 26 deaths occured as a result of UC in 2008, accounting for 0.53% of all deaths caused by diseases of the digestive system), a considerable number of Australians are affected by the disease. Estimates of the number of people affected by UC in Australia vary significantly between studies; however, overall they suggest that between 16,000 and 33,000 people have ulcerative colitis at any given time, and over 800 new cases are diagnosed each year.
A recent population-based study reported an annual incidence (new cases of UC per year) of 11.2/100,000 people, one of the highest rates reported from a scientific study. As this was the first incidence study conducted in Australia and examined people living in only one city, it is not known whether incident cases have remained stable or if incidence of UC is the same in the wider Australian population.
Global
From a global perspective, studies have reported an annual incidence of UC ranging from 0.5 to 24.5 cases per 100,000 people. The condition affects a similar number of men and women. UC is more common in Northern Europe and North America, although the incidence of the disease has remained stable over the past 50 years in these countries. On the other hand, incidence has been rising in Asian and Southern European countries. In the United States, UC affects an estimated 500,000 people and is the cause of 250,000 doctor visits and 30,000 hospitalisations each year.
Children
UC also affects children, and cases have been recorded in babies as young as 6 months old. About 10% of UC cases are recorded in individuals < 18 years of age. One study reported an annual incidence in Danish children of 2.6 per 100,000 people in the 2002–2004 period, an increase from 1.8 per 100,000 people in the 1998–2000 period. A British study reported that incidence of the disease had increased five-fold between 1988–1998, at which time the annual incidence in children ≤ 16 years was 1.4 per 100,000 people. Between 2000 and 2004, the incidence of UC increased to 2.7 per 100,000 people, while the incidence of Crohn’s disease appeared to have stayed the same.
Risk Factors for Ulcerative Colitis (Inflammatory Bowel Disease)
Family history

While the aetiology of the disease is not yet fully understood, many genetic susceptibility factors (characteristics of the genes that increase an individual’s susceptibility to a health condition such as UC) have been identified for inflammatory bowel disease, of which 25 are shared between UC and Crohn’s disease in adults. Many of these genetic factors relate to genes that affect the part of the immune system that regulates the intestine. The development of UC in children appears to share many genetic susceptibility factors of the adult disease; however, research suggests there may also be some distinct pathways leading to the childhood condition.
Research has shown differences in risk depending on birth order and gender of the child. One study reported that the last-born daughters of women with UC and males who are the only child of a mother with UC have a significantly increased risk of developing the condition compared to others. One study reported that 41% of males who were the only child of a woman with UC also had the condition compared to 18% of those who were not, while 48% of last-born daughters of these women developed UC compared to 28% of those who were not last-born to a mother with UC.
Abnormal immune response
UC is characterised by an abnormal response of the immune system, in which the immune system tries to attack food and other substances in the intestine – normally, the immune system would only try to attack foreign bodies such as infective agents. This attack can also focus on the cells of the colon. The intestine responds to the immune attack by concentrating white blood cells in the intestinal lining. This movement of white blood cells causes inflammation and the symptoms of UC. This also occurs in Crohn’s disease.
Age
The risk of developing UC depends on a person’s age. The condition is most common in the 15–35-year-old age group. Individuals aged 50–75 years are also more likely to have UC compared to the general population (all age groups).Research from Norway reports one of the highest incidences of UC (21.5 per 100,000 people annually) to date in the 25–34-year-old age group.
Race and ethnicity
Individuals who are of Jewish or Eastern European origin have an increased risk of UC. Caucasians also have an increased risk compared to individuals of other ethnicities.
Personality type
Individuals who exhibit anxious or obsessive personality traits and/or are introverted or emotionally immature have a higher risk of UC than those who do not. One study reported that 84% of individuals with UC have these personality traits.
Urban living
The incidence of UC is higher in developed countries compared to developing countries. However, the extent of the difference between these countries is reducing as incidence increases in developing countries (with increasing urbanisation). This suggests that elements of an urban lifestyle may contribute to the aetiology of UC. Changes in diet, patterns of exposure to sunlight, pollution and industrial chemicals characteristic of a Western lifestyle are thought to play a role.
Diet
Although dietary habits do not cause UC, factors relating to a person’s diet may influence the development of the condition. High dietary intakes of total fats, polyunsaturated fatty acids, omega-6 fatty acids and meat seem to increase the risk of UC, while high vegetable intake may reduce the risk of UC.
Other factors
Factors that do not cause UC but may exacerbate its symptoms include:
- Stress;
- Oral contraceptive use;
- Infection as a baby or child;
- History of appendectomy (removal of the appendix); or
- History of infection with mycobacteria (e.g. bacteria that cause tuberculosis and leprosy).
Progression of Ulcerative Colitis (Inflammatory Bowel Disease)

UC is further classified depending on which area of the colon is affected. Early stage disease is characterised by inflammation of the rectum which has not yet spread to the colon. When the inflammation extends into the colon but is limited to the lower part of the colon, the condition is classified as left-sided colitis. Cases involving inflammation to the upper section of the colon or the entire colon are referred to as extensive and pancolitis respectively.
UC can also be classified as mild, moderate, severe or fulminant, depending on the severity of the symptoms experienced.
Symptoms of Ulcerative Colitis (Inflammatory Bowel Disease)
If a doctor suspects you have ulcerative colitis, they will ask about the symptoms you have been experiencing to help them diagnose your condition. The classical symptoms of UC are bloody diarrhoea and mucus discharge from the rectum. Lower abdominal cramping and faecal urgency and/or incontinence (inability to control bowel movement) are also common symptoms. The disease is usually long term with symptomatic periods and asymptomatic periods.
Systemic symptoms include malaise, tiredness, fever and weight loss. The specific nature of symptoms depends on the extent of disease.
Proctitis or mild UC
Proctitis or mild UC is the most common form of the disease in adults, and is the stage of disease at which about half of adults with UC first visit their doctor. This mild form of the disease is less common in children and accounts for only 25% of first doctor visits.
The main symptoms are rectal bleeding, mucus discharge, faecal urgency and increased frequency of defecation; symptoms such as abdominal pain and fever are rare. In rare and severe cases of proctitis, constipation characterised by the passing of stools 1–2 times per week and the passing several times daily of blood and/or mucus from the rectum may occur.
Left-sided colitis or moderate UC
30% of adults and 30% of children with UC will present for the first time with left-sided colitis (moderate UC) or inflammation confined to the lower area of the colon.
Extensive colitis or severe UC
Extensive colitis, or pancolitis, is seen in approximately 15% of cases.
Non-intestinal symptoms of UC
While UC is a condition that affects the colon, up to 40% of people with UC experience symptoms that affect other organs, called extra-intestinal symptoms. The doctor is likely to enquire about your experience of extra-intestinal symptoms. The following extra-intestinal symptoms are associated with UC:
- Eye disorders, including uveitis (inflammation of the uvea, the middle layer of the eye which contains many blood vessels) and episcleritis (inflammation of the sclera, the membrane that covers the eye). These are sight-threatening conditions and you may need to see a specialist urgently if you have symptoms suggestive of an eye disorder;
- Arthropathy (painful joints) affecting small and large joints;
- Skin conditions, including alopecia (hair loss), erythema nodosum (a condition characterised by painful red skin lumps, usually affecting the shins) and pyoderma gangrenosum (a condition characterised by the death of skin tissue and the formation of ulcers, usually affecting the legs);
- Liver abnormalities;
- Venous thrombosis (formation of a blood clot in a vein); or
- Anaemia.
Systemic health
The doctor may also enquire about your general health and provide routine health interventions. For example, the doctor may assess whether you need any vaccinations or, if you are female, offer a pap smear test if you have not had one in the last two years.
Clinical Examination of Ulcerative Colitis (Inflammatory Bowel Disease)

UC shares symptoms with a number of other gastrointestinal conditions, and the doctor may need to conduct tests to determine whether your symptoms are caused by UC or another condition. These include:
- Crohn’s disease, another form of irritable bowel disease characterised by inflammation. It causes similar symptoms to UC. Distinguishing between these two conditions is often challenging and sometimes it is not possible for the doctor to definitively diagnose one or the other for several years after you begin experiencing symptoms. However, unless surgery is being considered, treatment of both conditions is similar;
- Anal fissure (a tear in the mucous membrane that lines the rectum and anus);
- Infectious colitis (colitis caused by an infection);
- Pseudomembranous colitis (colitis caused by infection following antibiotic use);
- Food-sensitive colitis (a short-term form of colitis caused by food intolerance, affecting young children);
- Ischaemic colitis (caused by inadequate blood flow to the colon, affecting adults only);
- Diverticulitis (an infected pouch in the colon, affecting adults only); and
- Colonic tumours (adults only).
How is Ulcerative Colitis (Inflammatory Bowel Disease) Diagnosed?
If the doctor suspects you have UC after asking about your symptoms and conducting an examination, tests may be performed to enable a definitive diagnosis to be made and/or other causes of the symptoms to be excluded. These tests include:
- Blood test;
- Urine test;
- Liver function test;
- Gut test;
- Stool sample.
If UC is still suspected after these routine tests have been conducted, further tests may be performed, including a biopsy and/or colonoscopy.
Biopsy
A biopsy is a procedure in which tissue or cells are removed from the body for further examination, for example under a microscope. In cases of suspected UC, the doctor may take a biopsy of the mucous membrane lining the rectum.
Sigmoidoscopy and colonoscopy
Sigmoidoscopy and colonoscopy are both techniques that allow the doctor to view the inside of your rectum. A special instrument (a sigmoidoscope or colonoscope), with a light and camera on one end, is inserted into the rectum. The doctor can examine the internal colon and identify features characteristic of UC using these methods.
Imaging techniques
Ultrasound (US), magnetic resonance imaging (MRI), CT (CT) scanning and x-ray may also be used to help in the diagnosis of UC. Each of these techniques allows the doctor to view your internal organs.
Prognosis of Ulcerative Colitis (Inflammatory Bowel Disease)

Overall, 66% of people with UC are able to relieve their symptoms with medications, and of those 80% who take their medicine correctly, as prescribed by the doctor, remain symptom free.
People with more severe forms of colitis may require other treatments to control symptoms, including colectomy, a surgical procedure in which part (partial colectomy) or all (total colectomy) of the colon is removed. Up to one third of patients will require such surgery after 20 years of UC.
The life expectancy of people with UC is not unlike that of the general population, although there is a significant risk of colorectal cancer that increases with the severity and duration of the disease.
The following risk factors have been identified for the development of colorectal cancer in individuals with UC:
- Having colitis for > 8 years;
- Having a more severe form of UC;
- Having a liver disease called sclerosing cholangitis; or
- Family history of colorectal cancer.
Onset of disease in childhood or adolescence may also increase the risk of cancer.
How is Ulcerative Colitis (Inflammatory Bowel Disease) Treated?
Treatment of UC is targeted at relieving symptoms and ensuring the symptoms do not return. This can improve the person’s quality of life.
Medical treatment
Medicines called aminosalicylates (a type of anti-inflammatory medicine) are most commonly used to treat UC. These medicines typically relieve symptoms and prevent symptoms recurring. However, these medicines can cause poisoning in individuals who have problems with their kidneys. They may also cause side effects such as headache, nausea, gastrointestinal pain, diarrhoea, oligospermia (low sperm production) in men and, rarely, more serious side effects.
There are many different aminosalicylate preparations, including tablets and rectal suppositories. The most appropriate preparation for you depends on the extent of your disease. Oral administration of aminosalicylate is complicated by digestion of the active components of the medicine before it reaches the part of the intestine affected by ulcerative colitis. Attempts have been made to prevent release of the aminosalicylate until it reaches the target area by binding it to carrier substances (called prodrugs) or coating the active drug with an acid resistant layer.
Mild cases

Topical aminosalicylates such as enemas or suppositories are the best treatment for proctitis, in which the inflammation is limited to the rectum. These preparations are inserted into the anus. If you feel uncomfortable or unsure about how to properly place the medicines in your anus, talk to your doctor for advice. Topical agents are usually sufficient for mild cases. However, if your proctitis is resistant to the treatment, the doctor may also prescribe oral medications.
Moderate to severe cases
For moderate to severe disease, it is common to use a topical aminosalycilate agent in combination with an oral medication. Individuals who do not improve or who are unable to tolerate oral aminosalicylates (about 10% of patients) may be prescribed oral corticosteroids (another type of anti-inflammatory medicine) instead of oral aminosalicylates. However, these medications are usually only prescribed for short-term use. Medicines that suppress the immune system may also be prescribed.
Severe cases
Individuals with severe UC require admission to hospital for aggressive treatment with intravenous steroids. They may also require:
- Intravenous fluids;
- A blood transfusion if they have experienced significant rectal bleeding;
- Feeding via a tube if they are experiencing malnutrition;
- Antibiotics; or
- Treatment for anaemia.
People with severe UC are monitored closely while in hospital. If symptoms such as fever persist, different medications may be used or surgery may be performed.
Surgery
Colectomy surgery to remove all or part of the colon may be needed in acute severe cases (fulminant colitis) and in chronic severe cases that cannot be treated with medication. Individuals with a high risk of colorectal cancer may also need surgery.
Maintenance therapy

Medication compliance
Medication compliance refers to the extent to which a person complies with their medication schedule – that is, the extent to which they take their medicine when they are supposed to. Patients who take the medication when they are supposed to at least 80% of the time are five times less likely to experience symptoms, compared to those who take their medicine correctly less than 80% of the time. Correct use of medicines for maintenance therapy also reduces the risk of colorectal cancer by as much as 75%.
However, medication compliance can be difficult, even with medications taken for short periods of time. Treatment for UC is life-long and many people fail to take their medications correctly. One study reported that only 40% of people adhered to their maintenance therapy medication schedule. Reasons for non-compliance included that they forgot to take the medicine, did not experience symptoms, found taking the medication inconvenient or had too many pills to take each day. There are many reasons why you might find it difficult to take your medications correctly. If you do, make sure you talk to your doctor or pharmacist for advice to help you adhere to your medication schedule.
New preparations of aminosalicylates which only need to be taken once a day are now available. Research has demonstrated that these medicines are as effective as those needing to be taken more than once a day. Taking medicines only once a day may reduce the challenges associated with medication compliance for individuals with UC.
Psychosocial intervention
UC can significantly affect quality of life, and individuals with UC are more likely to have psychological conditions such as depression. Such conditions may occur, for example, because of concerns regarding limitations the disease may place on lifestyle, personal relationships and financial stresses. They may also make medication compliance more difficult. If you feel like you are having difficulty coping emotionally with UC, talk to your doctor, who may provide you with a referral for further care such as support or evaluation by a specialist.
Nutritional intervention
Individuals with UC should maintain good nutritional habits. If you have trouble maintaining a healthy diet, talk to your doctor or ask about a referral to a nutritionist.
Complementary therapies
As yet, no complementary therapies have been demonstrated to be effective in the treatment of UC.
Screening for colorectal cancer
People with UC (with the exception of the mild form proctitis) have an increased risk of colorectal cancer. After 8–10 years of disease, some 2% develop cancer, increasing to 18% after 30 years. People with UC should therefore undergo periodic screening for colorectal cancer by colonoscopy, according to the following schedule:
- Moderate UC/left-sided proctitis: Every 5 years;
- Extensive colitis causing mild inflammation: Every 3 years; and
- Extensive proctitis causing moderate to severe inflammation: Annually.
More information
 |
For more information on inflammatory bowel disease, including how the digestive system works, types of IBD and useful videos, see Inflammatory Bowel Disease (IBD). |
Ulcerative Colitis (Inflammatory Bowel Disease) References
- Ghosh S, Shand A, Fergusson A. Ulcerative colitis. BMJ. 2000;320(7242):1119-23. Abstract | Full text
- Kornbluth A, Sachar DB. Ulcerative colitis practice guidelines in adults: American College Of Gastroenterology, Practice Parameters Committee. Am J Gastroenterol. 2010;105(3):501-23. Abstract | Full text
- Inflammatory bowel disease (IBD) [online]. Atlanta, GA: Centres for Disease Control and Prevention; 11 January 2011 [cited 26 April 2011]. Available from: URL link
- Moum B, Vatn MH, Ekbom A, et al. Incidence of ulcerative colitis and indeterminate colitis in four counties of southeastern Norway, 1990-93. A prospective population-based study. The Inflammatory Bowel South-Eastern Norway (IBSEN) Study Group of Gastroenterologists. Scand J Gastroenterol. 1996;31(4):362-6. Abstract
- Ulcerative colitis: Risk factors [online]. Baltimore, MD: University of Maryland Medical Center; 1 December 2008 [cited 30 March 2011]. Available from: URL link
- Jakobsen C, Wewera V, Ume F, et al. Incidence of ulcerative colitis and Crohn’s disease in Danish children: Still rising or levelling out? J Crohns Colitis. 2008;2(2):152-7. Abstract
- Efthymiou M, Taylor ACF, Kamm MA. Cancer surveillance strategies in ulcerative colitis: The need for modernization. Inflamm Bowel Dis. 2010; [Epub ahead of print]. Abstract
- Devadson D, Hussein H, Spray C, Sandhu B. The incidence of ulcerative colitis has doubled since 1999. J Pediatr Gastroenterol Nutr. 2005;40(5):643. Full text
- O’Conner, MB, O’Donavan N, Phelan MJ, Regan MJ. Inflammatory bowel disease such as ulcerative colitis is a risk factor for recurrent thromboembolic events: A case report. Cases J. 2009;2:173. Abstract | Full text
- Wilson J, Hair C, Knight R, et al. High incidence of inflammatory bowel disease in Australia: A prospective population-based Australian incidence study. Inflamm Bowel Dis. 2010;16(9):1550-6. Abstract
- Monsén U, Broström O, Nordenvall B, et al. Prevalence of inflammatory bowel disease among relatives of patients with ulcerative colitis. Scand J Gastroenterol. 1987;22(2):214-8. Abstract
- Kumar P, Clark M (eds). Clinical Medicine (5th edition). Edinburgh: WB Saunders Company; 2002. Book
- Genetics of inflammatory bowel disease in children [online]. Bethesda, MD: National Institute of Diabetes and Digestive and Kidney Diseases; 30 November 2010 [cited 30 March 2011]. Available from: URL link
- Tocchi AM, Lepre L, Liotta G, et al. Familial and psychological risk factors of ulcerative colitis. Ital J Gastroenterol Hepatol. 1997;29(5):295-8 Abstract
- Langan RC, Gotsch PB, Krafczyk MA, Skillinge DD. Ulcerative colitis: Diagnosis and treatment. Am Fam Physician. 2007;76(9):1323-30. Abstract | Full Text
- Loftus EV Jr. Clinical epidemiology of inflammatory bowel disease: Incidence, prevalence and environmental influences. Gastroenterology. 2004;126(6):1504-17. Abstract
- Williams D. Inflammatory bowel disease. Aust Doctor. 10 September 2004:31-8. Full text
- Tanaka M, Saito H, Kusumi T, et al. Spatial distribution and histogenesis of colorectal Paneth cell metaplasia in idiopathic inflammatory disease. J Gastroenterol Hepatol. 2001;16(12):1353-9. Abstract
- Causes of death, Australia, 2008: Diseases of the digestive system [online]. Belconnen, ACT: Australian Bureau of Statistics; 2 May 2011 [cited 20 April 2011]. Available from: URL link
- Access Economics. The economic cost of Crohn’s disease and ulcerative colitis [online]. Hawthorn, VIC: Crohn’s and Colitis Australia; 9 June 2007 [cited 20 April 2011]. Available from: URL link
- Umeno J, Asano K, Matsushita T, et al. Meta-analysis of published studies identified eight additional common susceptibility loci for Crohn’s disease and ulcerative colitis. Inflamm Bowel Dis. 2011; [Epub ahead of print]. Abstract
- Hou JK, Abraham B, El-Serag H. Dietary intake and risk of developing inflammatory bowel disease: A systematic review of the literature. Am J Gastroenterol. 2011;106(4):563-73. Abstract
- Mowat C, Cole A, Windsor A, et al. Guidelines for the management of inflammatory bowel disease in adults. Gut. 2011;60(5):571-607. Abstract
- Buckton S, Seltenreich H, Radford-Smith G, Kateley D. Gastroenterology nurse practitioner health management protocol for the management of inflammatory bowel disease in adults > 14 years of age [online]. Brisbane, QLD: Queensland Health; 2008 [cited 23 April 2011]. Available from: URL link
- Infliximab for subacute manifestations of ulcerative colitis: NICE technology appraisal guidance 140 [online]. London: National Institute for Health and Clinical Excellence; April 2008 [cited 23 April 2011]. Available from: URL link
- Infliximab for acute exacerbations of ulcerative colitis. NICE technology appraisal guidance 163 [online]. London: National Institute for Health and Clinical Excellence; December 2008 [cited 23 April 2011]. Available from: URL link
- Kane S, Huo D, Aikens J, Hanauer S. Medication nonadherence and the outcomes of patients with quiescent ulcerative colitis. Am J Med. 2003;114(1):39-43. Abstract
- Kamm MA, Lichtenstein GR, Sandborn WJ, et al. Randomised trial of once- or twice-daily MMX mesalazine for maintenance of remission in ulcerative colitis. Gut. 2008;57(7):893-902. Abstract | Full text
- Harris MS, Lichtenstein GR. Review article: Delivery and efficacy of topical 5-aminosalicylic acid (mesalazine) therapy in the treatment of ulcerative colitis. Aliment Pharmacol Ther. 2011;33(9):996-1009. Abstract | Full text
- Kane S. Does treatment schedule matter? Once daily versus divided doses of 5-ASAs. Dig Dis. 2010;28(3):478-82. Abstract
- Sandborn WJ, Kamm MA, Lichtenstein GR, et al. MMX Multi Matrix System(R) mesalazine for the induction of remission in patients with mild-to-moderate ulcerative colitis: a combined analysis of two randomized, double-blind, placebo-controlled trials. Aliment Pharmacol Ther. 2007;26(2):205-15. Abstract | Full text
- Brereton N, Bodger K, Kamm MA, et al. A cost-effectiveness analysis of MMX mesalazine compared with mesalazine in the treatment of mild-to-moderate ulcerative colitis from a UK perspective. J Med Econ. 2010;13(1):148-61. Abstract
- Prantera C, Rizzi M. 5-ASA in ulcerative colitis: Improving treatment compliance. World J Gastroenterol. 2009;15(35):4353-55. Abstract | Full text
Symptoms of Ulcerative Colitis:
Treatments Used in Ulcerative Colitis:
Drugs/Products Used in the Treatment of Ulcerative Colitis:
- Mezavant Gastro-Resistant Prolonged-Release Tablets (Mesalazine)
- Azapin (Azathioprine)
- Colazide (Balsalazide sodium)
- Dipentum (Olsalazine sodium)
- Salofalk Enemas (Mesalazine)
- Salofalk Foam Enemas (Mesalazine)
- Salofalk Granules (Mesalazine)
- Salofalk Tablets (Mesalazine)
- Thioprine (Azathioprine)
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







