- What is Crohn’s Disease (Inflammatory Bowel Disease)
- Statistics on Crohn’s Disease (Inflammatory Bowel Disease)
- Risk Factors for Crohn’s Disease (Inflammatory Bowel Disease)
- Progression of Crohn’s Disease (Inflammatory Bowel Disease)
- Symptoms of Crohn’s Disease (Inflammatory Bowel Disease)
- Clinical Examination of Crohn’s Disease (Inflammatory Bowel Disease)
- How is Crohn’s Disease (Inflammatory Bowel Disease) Diagnosed?
- Prognosis of Crohn’s Disease (Inflammatory Bowel Disease)
- How is Crohn’s Disease (Inflammatory Bowel Disease) Treated?
- Crohn’s Disease (Inflammatory Bowel Disease) Prevention
- Crohn’s Disease (Inflammatory Bowel Disease) References
What is Crohn’s Disease (Inflammatory Bowel Disease)
Crohn’s disease is a form of inflammatory bowel disease characterised by chronic inflammation of the gastrointestinal tract, which occurs in a discontinuous pattern (there are sections of healthy and diseased tissue). The inflammation is transmural, meaning it affects all layers of mucous membrane forming the gastrointestinal wall. Other types of inflammatory bowel disease such as ulcerative colitis cause superficial inflammation, meaning that they affect only the outer layer of the gastrointestinal wall.
In Crohn’s disease, inflammation can affect any of the gastrointestinal organs, from the mouth to the anus. However, it typically occurs in the terminal ileum (last section of the small intestine), in which case it is also referred to as terminal ileitis. The ileum (small intestine), colon (bowel or large intestine) and perianal region (the anus and surrounding area) are also commonly involved.
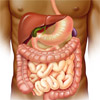 |
For more information on the anatomy of the gastrointestinal system, see Gastrointestinal System. |
When inflammation is limited to the colon, the disease is known as ulcerative colitis, another form of inflammatory bowel disease, thought to have similar causes. If both the small and large intestine are affected, the disease is known as ileocolitis. When other gastrointestinal organs (e.g. stomach, mouth) are affected, the condition is called Crohn’s disease.
Crohn’s disease can be further categorised depending on the extent and severity of symptoms as:
- Mild: Describes a person with limited complications. Weight loss is minimal (< 10%) and the person can tolerate swallowing oral medication;
- Moderate–severe: Describes mild Crohn’s disease which does not improve with an initial course of medicine, or mild disease accompanied by complications such as fever, abdominal pain or tenderness, significant weight loss, nausea and vomiting or anaemia;
- Severe–fulminant: Describes a person with Crohn’s disease being treated with steroid medication who experiences persistent symptoms, or one with severe complications including persistent vomiting, high fever, bowel obstruction or abscess, cachexia (severe weakness or muscle wasting) or rebound tenderness (pain when the abdomen is touched);
- Remission: Refers to Crohn’s disease which is asymptomatic or does not produce inflammation of the gastrointestinal tract, including cases that have responded to treatment with medicine or surgery.
Statistics on Crohn’s Disease (Inflammatory Bowel Disease)

Evidence shows that females are slightly more likely than males to develop Crohn’s disease.
Disease onset typically occurs in adolescence or early adulthood (between the ages of 15 and 30 years). The condition is rare in children aged less than 5 years. A review of studies from the United States reported the average age at Crohn’s diagnosis to be 33–39 years of age.
The age distribution of Crohn’s is often described as bi-modal, meaning that there are two age groups in which diagnosis of the disease peaks (a large peak in the 20–30 year age group and a smaller peak in the 60–70 year age group). But many studies have also reported unimodal distribution (a single peak) with incidence peaking in the 20–30 year age group and declining thereafter.
Risk Factors for Crohn’s Disease (Inflammatory Bowel Disease)
The cause of Crohn’s disease is unknown, but various immunological, genetic and environmental factors are thought to have a role.
Immunological factors
Although the causes of Crohn’s disease are poorly understood, the disorder is thought to be due, at least in part, to irregularities in the components of the immune system that regulate the mucous membranes of the gut. According to this hypothesis, disordered activities of T cells (blood cells that participate in the body’s immune responses) underpin the immune system irregularities.
Infectious factors
Infectious causes of Crohn’s disease are also suspected. Many infectious agents have been investigated in the past; however, a particular organism that causes Crohn’s disease has not been identified and theories which explain Crohn’s disease as an infectious condition remain controversial. Research examining the role of Mycobacterium paratuberculosis as an infectious cause of Crohn’s disease is currently underway in Australia.
Genetic factors
Many potential genes that might be involved in causing Crohn’s disease have been identified. Mutations in the NOD2/CARD15 gene on chromosome 16, which plays an important role in defence of the mucous membranes because it recognises bacteria, have been implicated in causing Crohn’s disease and are particularly likely to be associated with Crohn’s disease affecting the ileum (small intestine). However, only 30% of individuals with Crohn’s disease have such mutations, and some 20% of those who do not have Crohn’s also have such mutations.
Crohn’s disease is more prevalent amongst Caucasians compared to other ethnic populations. However, there is also evidence that this association may be caused by environmental rather than genetic factors, as environmental factors differ considerably between the geographic locations of various ethnic groups.
Environmental and lifestyle factors
Smoking is a well-established risk factor for Crohn’s disease. It is associated with a 3–4 times increased risk of developing the condition. Smokers also experience more severe disease when they have Crohn’s; they have more frequent relapses, are more likely to be admitted to hospital, and spend more time in hospital than non-smokers with Crohn’s disease. Quitting smoking reverses this disease course and is an important component of therapy for smokers.
Other environmental and lifestyle factors that may trigger disease include:
- Dietary factors, particularly a high sugar content in the diet;
- Variations in the balance of beneficial and harmful bacteria in the gut;
- Living in a Western society (although the condition is becoming more prevalent in less-developed countries with increasing industrialisation);
- Being from a low socio-economic background: Children from families of low socio-economic status are three times more likely to develop Crohn’s disease;
- Perinatal illness (illness immediately before or after childbirth) affecting either mother or baby is associated with a four-fold increased risk of Crohn’s disease for the child.
Progression of Crohn’s Disease (Inflammatory Bowel Disease)

Crohn’s disease usually manifests between 15 and 30 years of age, and typically follows a chronic and recurrent course (the disease goes through symptomatic and asymptomatic stages for the remainder of the person’s life). An individual with Crohn’s disease is likely to be affected for the rest of their life and experience periods of active, symptomatic disease, followed by periods of medical or surgical remission (periods when the disease becomes asymptomatic following surgical or medical treatments) and relapse to active disease. The majority of time with disease is spent in remission.
One study reported that a typical individual with Crohn’s disease will spend 24% of their lifetime with the disease in a state of medical remission, and 27% of the time experiencing mild disease. Typically, a small proportion of the time with disease is characterised by severe manifestations, which may either: heal after treatment with medicines (1%), require ongoing treatment with medicine to relieve symptoms (4%), or be untreatable with medicines and require surgical treatment (1%). A typical person spends 41% of their time with Crohn’s disease in post-surgical remission (with asymptomatic disease following surgery).
The disease course varies considerably between individuals. A minority of people (~10%) achieve lengthy remission periods. Most (73%) experience chronic recurring disease, and a considerable proportion (13%) experience unremitting disease (continuous symptoms). Existing data are insufficient to determine which people with Crohn’s disease are likely to achieve prolonged remission and which are not.
In the first year after a diagnosis of Crohn’s, 80% of affected individuals experience high disease activity and only 5% achieve remission, compared to 30% with high activity and 55% in remission more than 1 year after Crohn’s diagnosis. 25% of individuals with Crohn’s will experience active disease every year. A significant proportion (38%) require surgery within 1 year of starting to take medicine to treat Crohn’s disease.The disease course is influenced by smoking, with smokers having more frequent and severe recurrence of the disease.
Individuals with Crohn’s disease may experience the following complications during the course of their disease:
- Adhesions: Inflammatory adhesions between diseased and healthy sections of bowel may form – that is, diseased sections of the bowel may attach to healthy sections of the bowel. This complication is particularly likely in individuals with:
- Transmural ulceration: Inflammation affecting several layers of the bowel walls, as opposed to superficial inflammation which affects only the outer layer of the bowel wall; and/or
- Bowel obstruction; or
- A bout of toxic colitis (toxic megacolon), a potentially life-threatening complication in which the bowel widens rapidly. Surgical treatment is usually required;
- Bowel obstruction: Arising from stricturing (abnormal narrowing of the bowel), which may be chronic (long-term) or acute (short-term). Surgical treatment is usually required in these cases;
- Abscess formation: Abscesses may form and cause cavities in the mucosa (outer layer of the bowel wall) or submucosa (underlying layers of the bowel wall). The abscesses may rupture, causing bleeding. Rupture of a cavity in the mucosa can cause severe bleeding requiring urgent surgical treatment;
- Fistulae: Abnormal passages between two organs, or an organ and the body’s surface, may form as a result of Crohn’s disease. Fistulae typically involve the vagina, rectum, anus, vessels and skin. They are rarely responsive to treatment with medicines and surgery is usually required. Fistulae occur at some point in the course of disease for 20–40% of individuals with Crohn’s. Recurrence rates after treatment to close fistulae are as high as 82%;
- Perforation and bleeding: Perforation occurs rarely, typically in response to rapid deterioration causing severe symptoms. Perforation may cause severe bleeding requiring emergency surgery.
In children, Crohn’s disease causes similar symptoms and complications, and may also lead to marked growth retardation (slow growth) and delayed puberty. 15–40% of children with the disease experience growth retardation.
Symptoms of Crohn’s Disease (Inflammatory Bowel Disease)

Some symptoms are typical of Crohn’s disease and prompt the doctor to conduct further tests which enable them to confirm or exclude Crohn’s disease. These symptoms include:
- Chronic diarrhoea;
- Abdominal pain, which may progress from intermittent to chronic over the course of the disease;
- Bowel obstruction;
- Weight loss;
- Unexplained fever; and
- Night sweats.
The following symptoms may also occur as a result of Crohn’s disease:
- Diarrhoea (affects 85% of Crohn’s patient4 and is often chronic or nocturnal);
- Abdominal pain;
- Weight lossor anorexia;
- Blood or mucus in stools (faeces);
- Rectal bleeding;
- Perineal pain (pain in the area between the anus and the genitals);
- Nausea;
- Malaise (feeling unwell);
- Arthralgia (joint pain);
- Discharge; and
- Irritation associated with perianal fistulae (abnormal passages that form between the anus other body structures).
The doctor will probably ask whether or not you have experienced these symptoms. You will likely be asked about your history of smoking and your family history of inflammatory bowel disease. This information helps the doctor to correctly diagnose your condition.
A large proportion (14–76%) of individuals with Crohn’s disease have anal and/or perianal disease, meaning that the inflammation affects the anus and surrounding tissues. The doctor is therefore likely to examine the perianal region for signs of disease. Symptoms that affect the entire body are also common, including malaise, lethargy, and fever.
Other symptoms may be present as a result of complications (as alluded to above):
- Malabsorption syndromes, in which the body does not absorb nutrients from food properly. These may result in conditions such as anaemia;
- Fistulas and abscesses;
- Intestinal obstruction from strictures (narrowing of the intestines); and
- Rectal bleeding.

- Eyes: About 5% of individuals with Crohn’s disease have symptoms affecting their eyes. These may cause conditions such as:
- Uveitis (inflammation of the uvea, which is the middle part of the eye);
- Episcleritis (inflammation of the tissues covering the sclera, the white of the eyeball); and
- Recurrent conjunctivitis (inflammation of the outermost layer of the eyeball);
- Joints: About 25% of individuals with Crohn’s disease experience symptoms of the joints, including:
- Arthralgia (joint pain); and
- Arthritis (painful inflammation of the joints);
- Skin: About 15% of individuals with Crohn’s disease experience symptoms affecting the skin, including:
- Erythema nodosum (inflammation of fat cells under the skin)
- Pyoderma gangrenosum (characterised by skin ulcers); and
- Ulcers of the mucous membranes of the The corium and submucosa;
- Liver disorders may also occur in individuals with Crohn’s disease, and include:
- Sclerosing cholangitis (inflammation of the bile ducts connecting to the liver); and
- Fatty liver or the excessive build-up of fat in liver cells, which may lead to further liver disorders such as chronic hepatitis (inflammation of the liver) and liver failure;
- Urogenital complications, including:
- Nephrolithiasis, commonly referred to as kidney stones, characterised by the build up of small deposits (stones) in the kidneys; and
- Other kidney diseases;
- Blood vessel disorders, including:
- Deep vein thrombosis (a blood clot in the deep veins, usually the legs); and
- Pulmonary embolism (a blood clot in the lungs).
Onset is typically gradual and the symptoms are usually mild, though occasionally severe symptoms may occur rapidly. When severe symptoms occur rapidly, they may be similar to the symptoms of acute appendicitis. The doctor may need to conduct tests to distinguish between acute Crohn’s disease and acute appendicitis.
Throughout the course of the disease, an individual with Crohn’s may experience serious complications that require emergency treatment. These include:
- Perforation of the bowel wall, which affects 1–3% of individuals with Crohn’s at some stage of the disease. Perforation causes acute abdominal symptoms (e.g. severe abdominal pain). Emergency surgery is required to correct this complication;
- Toxic megacolon, which affects 4.4–6.3% of individuals with Crohn’s disease at some stage. It is characterised by rapid widening of the bowel, which may lead to bowel perforation and possible death if not treated surgically.
Differential diagnoses

- Ulcerative colitis;
- Acute appendicitis;
- Small bowel obstruction;
- Irritable bowel syndrome;
- Malabsorption syndromes (failure of the body to properly absorb nutrients from food);
- Infectious or ischaemic colitis (inflammation of the colon due to infection or lack of blood flow);
- Neoplasia (tumours);
- Haemorrhoids (swellings in the lining of the anus, commonly called piles); and
- Diverticular disease (formation of small out-pouchings in the colon).
Children
Diagnosis of Crohn’s disease may be slightly more difficult in children. In general the disease has similar symptoms, with the following additional symptoms characteristic of Crohn’s disease in childhood:
- Growth failure or delayed growth, the extent of which correlates to the severity of gastrointestinal symptoms of the disease. Children with more severe symptoms have greater delays or impairments in growth compared to children with mild symptoms;
- Delayed puberty and development of secondary sex characteristics (non-genital characteristics of men and women); and
- Psychological symptoms including increased rates of depression and anxiety.
Clinical Examination of Crohn’s Disease (Inflammatory Bowel Disease)
There are few physical signs of Crohn’s disease other than weight loss and general ill health, in particular pallor (pale skin) or cachexia (muscle wasting). There may also be perianal fissures, fistula or abscesses (e.g. small lumps around the anus); the doctor may examine the anus to check for these. There may be signs of extra-gastrointestinal involvement affecting the eyes, skin or joints. The doctor may also wish to examine a stool sample to check for blood.
How is Crohn’s Disease (Inflammatory Bowel Disease) Diagnosed?

- Full blood count: A test that analyses the makeup of the blood, including the proportion of red and white blood cells, and the amount of haemoglobin (responsible for transporting oxygen in the blood);
- Tests to assess markers of inflammation;
- Liver tests if the liver is thought to be affected;
- Blood cultures if sepsis (infection) is suspected;
- Stool cultures may be needed if you are experiencing diarrhoea, to exclude infectious causes; or
- Electrolyte tests: Electrolyte levels may be disturbed due to dehydration from diarrhoea.
Imaging and other tests may also be used in the diagnosis of Crohn’s disease. These include:
- X-rays;
- Biopsy: The removal of small sections of tissue for microscopic evaluation. In Crohn’s disease, an endoscope is used to guide the removal of tissue from the ileum (small intestine);
- Endoscopy: The use of a long, flexible tube with a camera on the end to view hollow internal cavities. Endoscopy is often used in the diagnosis of Crohn’s disease. Colonoscopy (use of an endoscope to view the colon) is the most commonly used technique, though the ileum and upper gastrointestinal tract (e.g. oesophagus) may also be viewed with endoscopy. Colonoscopy helps the doctor distinguish between Crohn’s disease and ulcerative colitis, and is typically used in conjunction with biopsy;
- Capsule endoscopy: Endoscopic capsules are swallowed and move through the gastrointestinal tract. Any part of the gastrointestinal tract can be viewed with capsule endoscopy, but the capsules cannot be used to assist biopsy (removal of tissues); and
- CT: X-rays are used to produce computer-generated images of the body’s internal structures. This technique allows the doctor to assess all layers of the bowel wall, unlike endoscopic techniques which only enable visualisation of the outer layer of the bowel wall.
Prognosis of Crohn’s Disease (Inflammatory Bowel Disease)
Crohn’s disease is a lifelong condition. Despite being characterised by periods of active symptomatic disease and asymptomatic remission, individuals with Crohn’s disease typically experience severe debilitation as a result of the condition. For example, in the first year after diagnosis, 25% of individuals with Crohn’s require time off work, and after 5–10 years of disease, 15% are unable to work.
Many individuals achieve periods of remission with treatment, though a significant proportion require surgical treatment; 50% will undergo surgery to induce remission in the first 10 years of disease, and 70–80% will require surgery in their lifetime.
Individuals with Crohn’s disease have an increased risk of colorectal and small bowel cancer. There is also evidence of an increased risk of mortality in individuals with Crohn’s disease.
How is Crohn’s Disease (Inflammatory Bowel Disease) Treated?

Medicine
Taking medicine alongside lifestyle modifications is the mainstay of treatment for Crohn’s disease. Surgery tends to be reserved for those individuals with chronic obstructive complications (e.g. stricturing). The primary aims of treatment are to treat acute flare-ups when they occur, and induce and maintain remission of symptoms following a flare-up.
Treatment varies according to the severity and anatomical site of disease (e.g. whether the stomach or colon is affected). Similar medications are used as in the treatment of ulcerative colitis (the other major form of inflammatory bowel disease), namely:
- Oral corticosteroids: Medicines used to treat a range of inflammatory conditions, including severe inflammation. They are typically used to treat active flare ups and may also be used in ongoing maintenance therapy;
- Aminosalicylate preparations: Medicines used to treat inflammatory bowel disease in mild-to-moderate cases. They are typically used for ongoing maintenance therapy, rather than to induce remission.
Appropriate treatments differ for adults and children because of the need to attain appropriate growth and pubertal development in children (corticosteroid use in children is associated with delayed growth and puberty). However, there is a general lack of evidence regarding the effectiveness of different treatment options in children.
Aminosalicylates
Aminosalicylates may be used to induce remission of a flare up of Crohn’s disease, though evidence suggests that they not as effective as corticosteroids for inducing remission. In addition, many people do not tolerate aminosalicylate medications due to side effects. But if aminosalicylates have effectively treated your condition in the past and you were able to tolerate the side effects, your doctor may prescribe them for treatment of an acute flare up.
Aminosalicylates may also be used for maintenance therapy, particularly following surgery to induce remission. For individuals who have a high risk of relapse (experiencing an acute flare up in the future), including those who have had surgery more than once in the past, immunosuppressive medications may be more effective for maintenance therapy. However, evidence suggests that maintenance therapy with aminosalicylates reduces the risk of colorectal cancer, and for this reason aminosalicylates may be preferred.
Aminosalicylates are not used to treat Crohn’s disease in childhood.
Corticosteroids
Corticosteroid medications are the most effective and most commonly used treatment for inducing remission of an active flare up of Crohn’s disease. In severe cases complicated by fistulae, corticosteroids are rarely effective; however, they may be taken to reduce inflammation prior to surgery, which is usually required to close fistulae.
The choice of medicine depends on the severity and site of disease. Budesonide, prednisolone or methylprednisolone are the corticosteroids most commonly used in the treatment of Crohn’s disease. Budesonide is slightly less effective than either prednisolone or methylprednisolone, but is associated with fewer side effects. It is recommended for achieving remission of mild-to-moderate cases of Crohn’s disease confined to the colon and ileum (small and large intestine). The prescribing doctor will determine the best dose and frequency for you. Always take the medicines as prescribed by the doctor.
If your Crohn’s disease is severe or affects a more extensive area of the gastrointestinal system (structures above the colon and ileum, for example the stomach of oesophagus) prednisolone or methylprednisolone will probably be prescribed to induce remission. While more effective than budesonide, prednisolone or methylprednisolone are more likely to induce side effects such as bleeding and infection. The doctor will consider the risk of side effects in relation to the expected benefits of you taking the medicine before prescribing prednisolone or methylprednisolone, and will determine the best dose and frequency of taking the medication for you. Always take the medicines as prescribed by the doctor.
Corticosteroids are not usually prescribed for maintenance therapy if remission is achieved using medicines (as opposed to surgery).
In children, corticosteroids are not generally used as they are less effective in inducing remission compared to enteral feeding (feeding through a tube inserted in the throat).
Antibiotics

Antibiotics are not used to treat Crohn’s disease in children.
Immunosuppressive agents
Immunosuppressive medications called azathioprine and mercaptopurine are effective for inducing remission of Crohn’s disease, but are associated with many, often serious, side effects. Treatment for at least 17 weeks is necessary for maximum effectiveness.
Azathioprine may be used as maintenance therapy once remission is achieved using an immunosuppressive agent. It is usually only prescribed to individuals who cannot use corticosteroids to treat their Crohn’s disease (either because corticosteroids are ineffective or because they produce intolerable side effects), because azathioprine is associated with serious adverse events including myelodysplastic syndrome, a blood disorder that can be fatal. If you take azathioprine for maintenance therapy, you will need to have your blood tested regularly to check for signs of myelodysplastic syndrome developing.
Mercaptopurine may be used for maintenance therapy following surgical remission, but is only recommended for individuals with a high risk of recurrence, including those who have undergone > 1 surgical procedure.
Immunosuppressive agents are not used to treat children with Crohn’s disease
Methotrexate
Methotrexate, a medicine administered by injection and often used in cancer treatment, is a further option for inducing remission of an acute flare up in adults with Crohn’s disease which does not heal after treatment with aminosalicylates, corticosteroids or immunosuppressive agents. The medicine is only used when other medicines fail to treat Crohn’s disease, as methotrexate is associated with serious side effects, including liver disorders. If you are prescribed this medicine, you will need to have your liver function tested regularly to ensure the medicine is not damaging your liver.
Methotrexate may be used for maintenance therapy, but will only be prescribed when other medicines cannot be used (either due to side effects or because they fail to treat Crohn’s disease effectively).
Note that if you are pregnant or wish to conceive (men and women), you should not take methotrexate. Tell your doctor if you become pregnant or wish to conceive while taking methotrexate.
Methotrexate is not used to treat children with Crohn’s disease.
Tumour necrosis factor alpha inhibitors (TNF-α inhibitors)
Infliximab, which belongs to a group of medicines called tumour necrosis factor alpha (TNF-α) inhibitors, is a new medicine now used in Australia as a treatment for severe Crohn’s disease that does not respond to other medicines (aminosalicylates, corticosteroids, immunosuppressive agents). Infliximab is administered via infusion (via a drip inserted into a vein), and evidence shows that a single infusion of the medicine is effective in inducing remission in approximately two thirds of individuals who receive the infliximab to treat an acute flare up.
Infliximab is used in maintenance therapy, and 60% of individuals who achieve remission using infliximab will maintain remission if treated with 8-weekly infusions of the medicine.
In the short term, infliximab is not associated with adverse side effects; however, more evidence is needed to determine the safety of this medicine when used for long-term maintenance therapy. Repeated use for maintenance therapy may be limited in many individuals because they have adverse reactions to the infusion. These include pruritis (itching), nausea and flushing.
Infliximab suppresses the immune system, which makes it unsuitable for treating patients with septicaemia. Because of its immunosuppressive effect, infliximab predisposes individuals taking the medicine to infectious complications such as tuberculosis. Individuals treated with infliximab have a 4–5 times greater risk of tuberculosis, and must be screened for tuberculosis before commencing infliximab treatment. Infliximab should be used with caution by individuals with congestive heart failure, so it is important to tell your doctor if you have heart problems.
Note that infliximab is not subsidised under the Pharmaceutical Benefits Scheme (PBS), so cost may limit its use.
The effects of TNF-α inhibitors in children have not yet been studied.
Lifestyle measures
Education and support

Smoking cessation
Non-smokers with Crohn’s disease experience greater periods of remission, and quitting smoking is associated with lower relapse rates and reduced use of medicine to maintain remission. If you smoke, it is important to quit as this will help improve your Crohn’s disease. However, be aware that the nicotine contained in cigarettes is addictive and many people require counselling or other forms of support to help them quit smoking. You are more likely to quit smoking if you have such support, so talk to your doctor about strategies that can help you quit and places where you can access support.
Nutritional interventions
Nutritional interventions (treatments that modify the diet), are used in Crohn’s disease therapy to both induce and maintain remission. Nutritional interventions may also be used to restore nutritional deficiencies arising because of the disease. These deficiencies may be macronutrient (e.g. anorexia, cachexia) or micronutrient (e.g. anaemia) deficiencies, or both.
Providing macronutrient support (support to consume more energy/calories) may improve growth in children. Micronutrient deficiencies should be identified and corrected through supplementation (e.g. vitamin tablets) with the aim of improving conditions caused by nutritional deficiency such as anaemia. Folate supplements may also be given to individuals with Crohn’s disease, as evidence indicates that taking folate supplements reduces the risk of developing colon cancer.
In addition, elemental diets (consuming easily digestible foods only) and enteral nutrition (tube feeding) have an established role in the treatment of inflammatory symptoms of Crohn’s disease in children. Elemental diets are also an option for inducing and maintaining remission in adult patients. While they are less effective than corticosteroid treatment for adults, they are associated with fewer side effects. There is no evidence that other nutritional interventions are effective in treating Crohn’s disease.
Individuals who may be prescribed enteral nutrition to induce remission include those:
- With partial obstruction of the small bowel;
- With severe Crohn’s disease involving the perianal region and causing pain;
- Who fail to achieve remission with corticosteroid therapy;
- With borderline intestinal failure; or
- Children with active Crohn’s disease causing growth failure.
Fish oil supplementation
There is promising evidence for fish oil capsules as maintenance therapy for Crohn’s disease. However, further studies are needed to confirm the effectiveness of fish oil therapy and it is not currently recommended for routine use.
Monitoring for colorectal cancer
As mentioned previously, long-standing Crohn’s disease is associated with an increased risk of colorectal cancer, although there are a lack of guidelines regarding monitoring for colorectal cancer in individuals with Crohn’s disease. In general, frequent monitoring by colonoscopy is recommended from 10 years after the onset of disease. The appropriate monitoring interval varies depending on the extent and severity of disease. Your doctor will advise you how often you should undergo monitoring for colorectal cancer.
Surgical treatment

- Elective:
- Fistulae, with or without abscess;
- Obstruction of the gastrointestinal tract;
- When treatment with medicines fails;
- Cancerous tumours; or
- Growth retardation in children;
- Urgent:
- Perforation of the bowel or other gastrointestinal structure;
- Bleeding; or
- Toxic colitis or megacolon (rapid widening of the colon due to inflammation).
Elective reasons are the most common for surgery. While these procedures are considered elective, there is evidence suggesting that early surgery (elective as opposed to urgent) is associated with significantly reduced complications of Crohn’s disease in adults. In children, the use of surgical interventions requires further studies, but current evidence supports the use of surgery in pre-pubertal children with Crohn’s disease that fails to respond to other treatments. Surgery is also an option for children experiencing growth retardation.
Many different surgical techniques are performed for the treatment of Crohn’s disease. The surgical procedure used depends on the anatomical site and features of the individual’s disease.
Abscess drainage
Individuals whose Crohn’s disease is complicated by abscesses may undergo surgery to drain the abscesses. In this case, laparotomy is likely to be used – the surgeon will gain access to the abscesses via an incision in your abdomen. If abscesses recur, drainage will need to be performed again and the doctor may also recommend bowel resection (see below).
Strictureplasty
Strictureplasty is a conservative surgical technique requiring removal of smaller sections of the bowel compared to bowel resection (see below). It is now a preferred approach for managing Crohn’s disease in individuals with obstruction caused by strictures. The procedure involves diseased sections of the bowel being cut away to relieve obstructive symptoms. Healthy sections of the bowel are re-attached with stitches. The treatment improves food tolerance and enables weight gain.
Individuals who undergo strictureplasty may need a second operation in the future. The need for reoperation is similar to the need with bowel resection, although strictureplasty is associated with fewer side effects and illness compared to bowel resection. It is important that individuals undergo thorough assessment to rule out non-Crohn’s disease causes for their symptoms before undergoing strictureplasty. For example, the doctor may use CT scans or colonoscopy to view the gastrointestinal organs before performing strictureplasty.
Individuals who are likely to benefit from strictureplasty include those:
- With diffuse (widespread) disease affecting the small bowel involving multiple strictures (sections in which the bowel is narrowed);
- With stricture formation following major bowel resection (surgery);
- Who develop strictures early in the course of Crohn’s disease;
- Who experience rapid recurrence of obstructive symptoms following treatment;
- With short bowel syndrome (a malabsorption syndrome that occurs as a result of removal or dysfunction of the small intestine) and stricture formation; or
- With strictures in the duodenoum (the first section of the small intestine connecting to the stomach).
The procedure is contraindicated (cannot be performed) in people with:
- Perforation of the small bowel;
- Inflammation due to infection of the bowel tissues;
- Fistulae when the surgery is to be carried out near the site of the fistula;
- Multiple stricture in a short section of bowel;
- Strictures close to a site selected for surgery;
- Strictures affecting the colon;
- Infectious complications; or
- Unfavourable anatomy (abnormally-shaped or positioned organs, or structures in the gastrointestinal tract which make surgery more risky).
Bowel resection
Bowel resection is a surgical procedure in which diseased sections of the bowel are removed and healthy sites joined together. The amount of bowel removed depends on the extent of disease. Mini-resections are preferred over radical resection in order to prevent short bowel syndrome. The procedures may be conducted by laparoscopy (minimally invasive, camera-guided surgery), laparotomy (surgery performed through an incision in the abdomen) or open surgery. Laparoscopy is typically preferred as it is less invasive and involves shorter post-operative recovery periods.
Resection may be undertaken for people with:
- Abscess that fails to heal following drainage: In these cases, abscess drainage by laparotomy is performed again before surgical resection of the diseased area of bowel. The surgery may be delayed if large sections of non-diseased bowel will be lost as a result of surgery;
- Bowel obstruction, either acute or chronic: These complications often fail to respond to other treatments. Early surgical intervention is recommended for individuals with obstructive complications;
- Ileocaecal disease (disease affecting the junction between the small and large intestine).
Bowel bypass
Bowel bypass, once the mainstay of surgical treatment for Crohn’s disease, is now rarely used due to improvements in the safety and effectiveness of medicines and more conservative surgical techniques. It may still be used for a limited number of individuals who fail to respond to other therapies.
Colectomy
Colectomy (removal of all or part of the colon) may be used to treat individuals with Crohn’s disease that fails to respond to other treatments. Unlike with ulcerative colitis, colectomy rarely cures Crohn’s disease, as inflammation can reappear in other sections of the gastrointestinal tract.
More Information
 |
For more information on inflammatory bowel disease, including how the digestive system works, types of IBD and useful videos, see Inflammatory Bowel Disease (IBD). |
Crohn’s Disease (Inflammatory Bowel Disease) Prevention
Crohn’s disease cannot be prevented. Correctly taking the medication prescribed by your doctor is the key measure for preventing acute recurrence of the disease.
Crohn’s Disease (Inflammatory Bowel Disease) References
- von Roon AC, Reese GE, Orchard TR, Tekkis PP. Crohn’s disease. BMJ Clin Evid (Online). 2007. Available from: [Abstract | Full text]
- Murtagh J. Crohn’s disease: Patient information. Aus Doctor. 2005; June. Full text
- Geboes K. Chapter 18: Histopathology of Crohn’s disease and ulcerative colitis. In: Satsangi J, Sutherland LR. Inflammatory Bowel Diseases (4th edition). New York: Churchill-Livingstone; 2003: 255-76. Chapter | Book
- Knutson D, Greenberg G, Cronau H. Management of Crohn’s disease: A practical approach. Am Fam Physician. 2003;68(4):707-14. Available from: [Abstract | Full text]
- Selby WS. Current issues in Crohn’s disease. Med J Aust. 2003;178(11):532-3. Full text
- Loftus EV Jr, Schoenfeld P, Sandborn WJ. The epidemiology and natural history of Crohn’s disease in population-based patient cohorts from North America: A systematic review. Aliment Pharmacol Ther. 2002;16(1):51-60. Available from: [Abstract | Full text]
- Shanahan F. Crohn’s disease. Lancet. 2002;359(9300):62-9. Abstract | Full text
- Castori M, Grammatico P. Chapter 3: Genetics. In: Tersigni R, Prantera C (eds). Crohn’s Disease: A multidisciplinary approach. Milan: Springer-Verlag; 2010: 17-25. Book
- Rizzi M. Chapter 2: Epidemiology. In: Tersigni R, Prantera C (eds). Crohn’s Disease: A multidisciplinary approach. Milan: Springer-Verlag; 2010: 9-16. Book
- Lichtenstein GR, Hanauer SB, Sandborn WJ. Management of Crohn’s disease in adults. Am J Gastroenterol. 2009;104(2):465-83. Available from: [Abstract | Full text]
- Strong SA. Surgical management of Crohn’s disease. In: Holzheimer RG, Mannick JA (eds). Surgical Treatment: Evidence-based and problem-oriented. Munich: Zuckschwerdt Verlag; 2001. Available from: [Chapter | Book]
- Werbin N, Haddad R, Greenberg R, et al. Free perforation in Crohn’s disease. Isr Med Assoc J. 2003;5(3):175-7. Available from: [Abstract | Full text]
- Newby EA, Sawczenko A, Thomas AG, Wilson D. Interventions for growth failure in childhood Crohn’s disease. Cochrane Database Syst Rev. 2005;(3):CD003873. Abstract | Full text
- Eilam O, Goldin E, Shouval D, et al. Sclerosing cholangitis associated with Crohn’s disease and autoimmune haemolytic anaemia. Postgrad Med J. 1993;69(814):656-8. Available from: [Abstract | Full text]
- Canbay A, Bechmann LP, Best J, et al. Crohn’s disease-induced non-alcoholic fatty liver disease (NAFLD) sensitizes for severe acute hepatitis B infection and liver failure. Z Gastroenterol. 2006;44(3):245-8. Abstract
- Kane S. Urogenital complications of Crohn’s disease. Am J Gastroenterol. 2006;101(12 Suppl):S640-3. Available from: [Abstract]
- Bernstein CN, Blanchard JF, Houston DS, Wajda A. The incidence of deep venous thrombosis and pulmonary embolism among patients with inflammatory bowel disease: A population-based cohort study. Thromb Haemost. 2001;85(3):430-4. Available from: [Abstract]
- Weston LA, Roberts PL, Schoetz DJ Jr, et al. Ileocolic resection for acute presentation of Crohn’s disease of the ileum. Dis Colon Rectum. 1996;39(8):841-6. Available from: [Abstract]
- Grieco MB, Bordan DL, Geiss AC, Beil AR Jr. Toxic megacolon complicating Crohn’s colitis. Ann Surg. 1980;191(1):75-80. Available from: [Abstract | Full text]
- Griffiths AM, Nguyen P, Smith C, et al. Growth and clinical course of children with Crohn’s disease. Gut. 1993;34(7):939-43. Available from: [Abstract | Full text]
- Romdhane H, Karoui S, Serghini M, et al. Crohn’s disease, primary sclerosing cholangitis and antiphospholipid syndrome: An uncommon association [in French]. Tunis Med. 2009;87(5):349-51. Available from: [Abstract]
- Leighton JA, Shen B, Baron TH, et al. ASGE guideline: Endoscopy in the diagnosis and treatment of inflammatory bowel disease. Gastrointest Endosc. 2006;63(4):558-65. Available from: [Full text]
- Gore RM, Balthazar EJ, Ghahremani GG, Miller FH. CT features of ulcerative colitis and Crohn’s disease. AJR Am J Roentgenol. 1996;167(1):3-15. Available from: [Full text]
- Ferguson A, Glen M, Ghosh S. Crohn’s disease: Nutrition and nutritional therapy. Baillières Clin Gastroenterol. 1998;12(1):93-114. Available from: [Abstract]
- Mallon DP, Suskind DL. Nutrition in pediatric inflammatory bowel disease. Nutr Clin Pract. 2010;25(4):335-9. Available from: [Abstract]
- Brown CJ. Heineke-Mikulicz and Finney strictureplasty in Crohn’s disease. Op Tech Gen Surg. 2007;9(1):3-7. Available from: [Full text]
- Surgery for Crohn’s disease [online]. New York, NY: Crohn’s and Colitis Foundation of America; January 2009 [cited 15 June 2011]. Available from: [URL link]
- ACR appropriateness criteria: Crohn’s disease [online]. Reston, VA: American College of Radiology; 2008 [cited 3 July 2011].
All content and media on the HealthEngine Blog is created and published online for informational purposes only. It is not intended to be a substitute for professional medical advice and should not be relied on as health or personal advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. Never disregard the advice of a medical professional, or delay in seeking it because of something you have read on this Website. If you think you may have a medical emergency, call your doctor, go to the nearest hospital emergency department, or call the emergency services immediately.







